A heart attack creates a state of inadequate blood supply to organs and tissues that damages heart function and forms scar tissue for many weeks after the event. Using a pre-clinical heart attack model in mice, researchers from the University of Utah tested multiple combinations of stem cells, plasmid-based genes, and growth factors to see which concoctions created effective treatments for different conditions induced by a heart attack.
The researchers looked at three types of cells:
- Umbilical cord-derived sub-epithelial cells (UC-SECs),
- Bone marrow-derived mesenchymal stem cells (BM-MSCs),
- Induced pluripotent stem cell-derived cardiomyocytes (iPSC-CMs),
two types of plasmid-based genes:
and a growth factor, VEGF165.
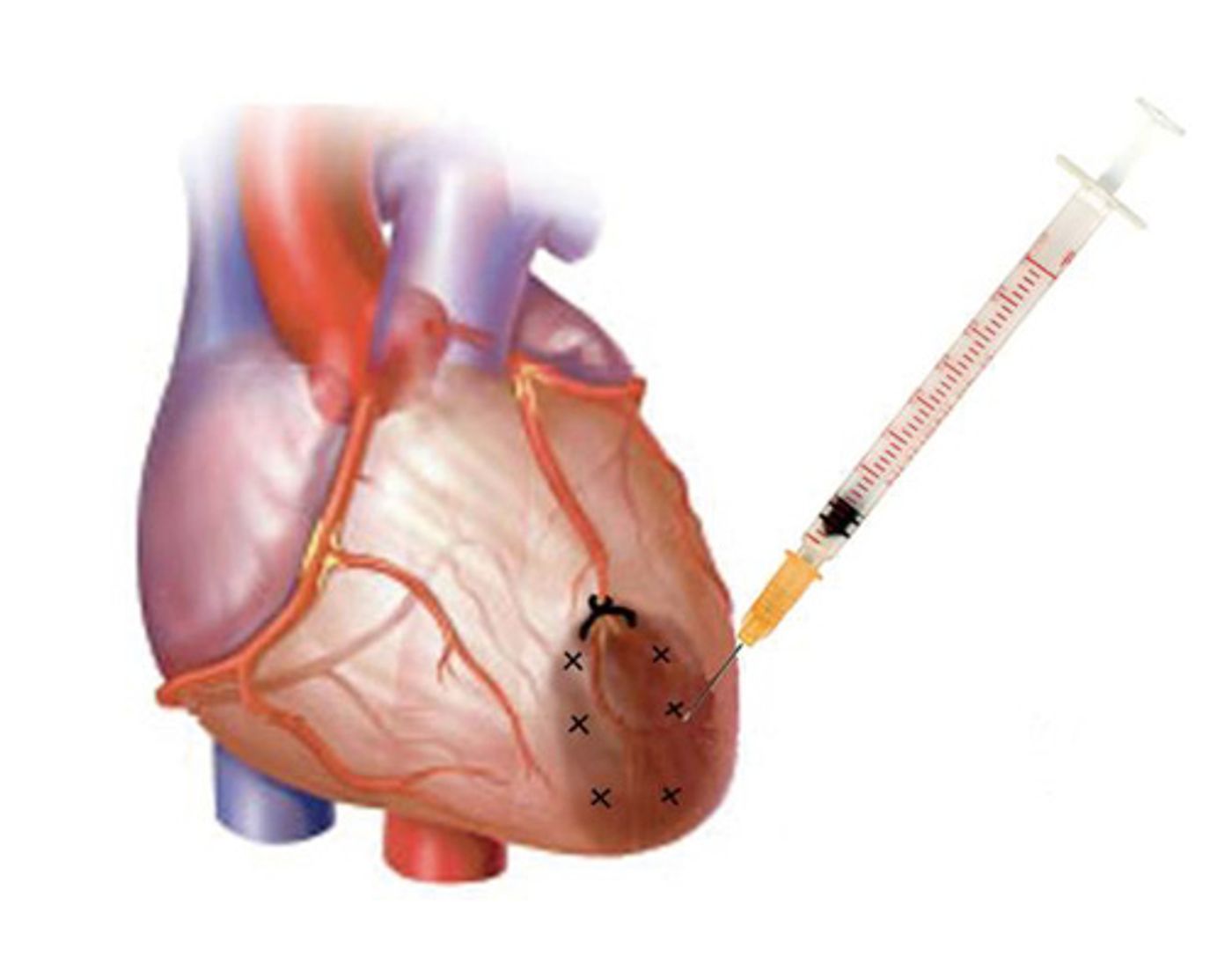
To mimic the biological and physiological aspects of heart muscle ischemia when the blood supply to the heart is obstructed as in during a heart attack, the researchers performed left anterior descending artery ligation on the mice models of disease. This technique is commonly used to imitate the impact of a heart attack on the body. With a single stich, researchers can tie off, or ligate, a blood vessel creating a state of inadequate blood supply to the heart that is almost immediately evident. After this procedure, the researchers could freely test different therapeutics to see what effect they had on the condition of the mice hearts.
The tissue-based cells were expanded under hypoxic conditions before injection, meaning they were deprived of adequate oxygen supply. The researchers injected each combination of cells, genes, and/or growth factor intramyocardially, and followed up at 4 and 12 weeks post-injection.
After measuring, analyzing, and comparing measurements of echocardiography, hemodynamic catheterization measurements and histology throughout the study, the researchers saw several trends where certain therapeutic injections were best suited for correcting specific heart conditions that follow a heart attack.
First, UC-SECs appeared to be the best candidate for scar remodeling, but the two plasmid-based genes also proved to be better for scar remodeling than controls and other genes, cells, and growth factor combinations.
iPSC-CMs and S100a genes equally improved contractile function the best out of the samples tested, followed by UC-SECs. Lastly, angiogenesis, the creation of new blood vessels, was most successful when treated with VEGF165.
Study co-author Dr. Amit N. Patel said the study “demonstrated that, depending on which aspect of cardiac recovery is being evaluated, scar remodeling, improvement in contractile function, angiogenesis, or inflammation, a different [gene or cell] may be best suited.”
Indeed, this study provided background knowledge for further development of cellular and genetic therapies for preserving cardiac function. Presently, there is no approved therapy to address scar remodeling or replacement with fresh cardiomyocytes.
In conclusion, the researchers recommended that “further studies should aim to evaluate dose and combination therapies in order to decipher the most clinically applicable treatment.”
Their study was recently published in the journal
Cell Transplantation.
Sources:
Cell Transplantation Center of Excellence for Aging and Brain Repair,
Journal of Visualized Experiments