For unknown reasons, a new study has uncovered the ability of a protein called hepatoma derived growth factor (HDGF) to determine how severe a certain case of pulmonary arterial hypertension (PAH) is in a patient. There is currently no cure for PAH, but this research is helping doctors improve diagnostics and develop better treatment plans.
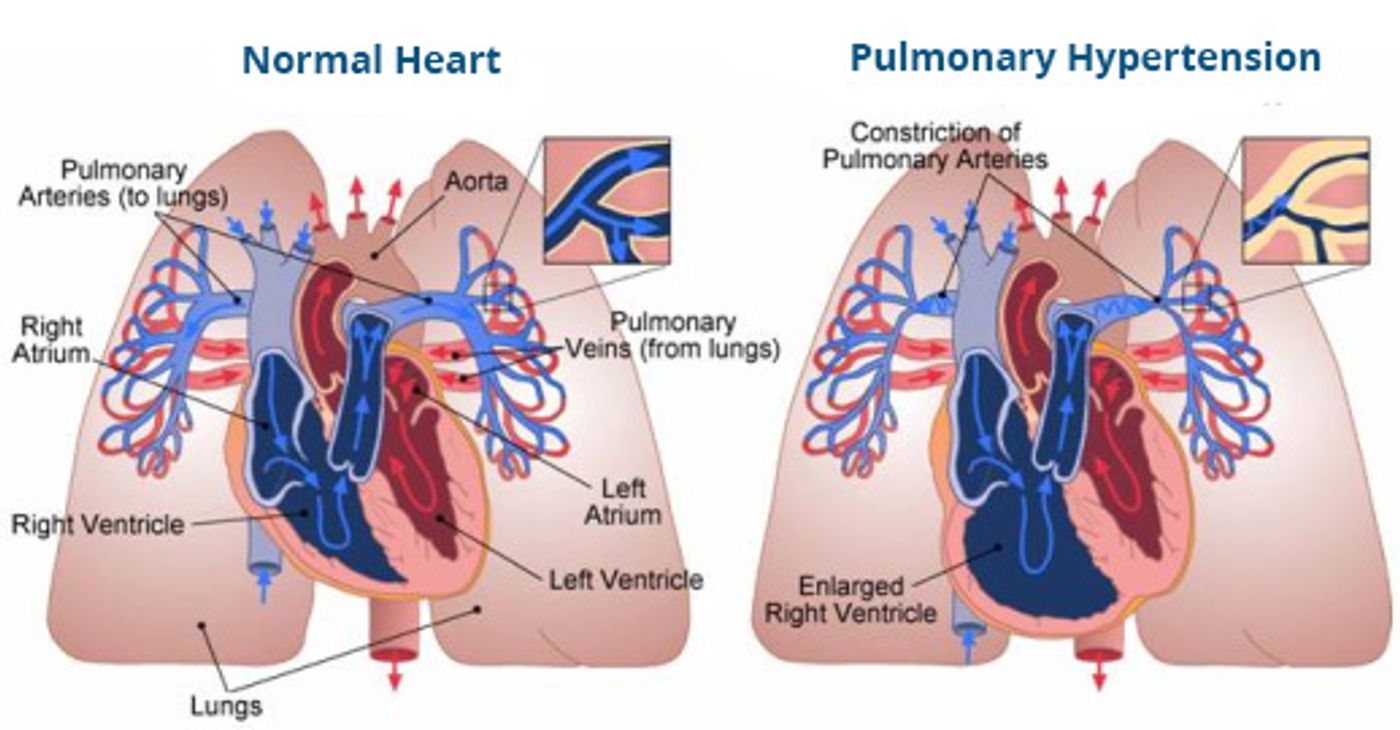
PAH is a chronic condition that puts stress on the heart as it tries to push blood through narrowed arteries of the lungs that grow stiff and tight over time. Affecting approximately 200,000 Americans, PAH can be inherited or occur as a result of infections, congenital heart disease, connective tissue disorders, or continuous exposure to a high-altitude environment. Most people afflicted with PAH have almost no other health problems and are often relatively young. Drugs are available to alleviate symptoms and attempt to improve blood flow, and lung transplant procedures are done if nothing else seems to work.
PAH has historically been hard to diagnose and assess if a patient is improving or worsening, especially in children. From Johns Hopkins Medicine, scientists bring a light amidst the darkness of this disease. They’ve developed a noninvasive test for PHA using HDGF to make more accurate diagnoses of patients so they can receive the right medication for their condition. In the past doctors have used an invasive procedure called cardiac catheterization, but the new test is more specific and can accurately portray the current health status of the lungs.
The Johns Hopkins researchers confirmed the connection of HDGF to PAH status by conducting a series of comparisons between healthy people and PAH patients. They used blood samples from 39 PAH patients considered severe cases because treatment hadn’t worked, and they were on the waiting list for lung transplants. These samples were compared to a group of 39 healthy volunteers with the same ratio of ages, races, and gender. The median level of HDGF in the healthy group was 0.29 nanograms per mL, but the median level of HDGF in the PAH patients was a whopping 1.93.
Continuing with a follow-up study, the researchers collected an additional 73 blood samples from PAH patients, this time over five years, comparing results between survivors and non-survivors. HDGF was lower in survivors than in non-survivors, and an HDGF reading of over 0.7 indicated more severe heart damage and shorter distances achieved in a six-minute walking test. This study also showed that higher levels of HDGF made PAH patients 4.5 times as likely to die, even after adjusting the data for a variety of potentially skewing factors.
With these trials completed and data analyzed, the Johns Hopkins researchers knew that elevated levels of HDGF indeed indicated a more severe case of PAH, but they still don’t know what biochemical processes are causing the association. HDGF is known to be important for forming new blood vessels in the lung, and it also has “mitogenic and DNA-binding activity.” Elevated HDGF expression has also been implicated in cases of enhanced tumor growth, but scientists aren’t sure if that is even related to the current study.
Senior author Allen Everett, M.D. thinks that HDGF levels might rise to prompt blood vessel repair when arteries in the lungs are strained due to PAH. For now, Everett is satisfied to declare HDGF as a useful diagnostic tool for determining PAH severity. For tomorrow, he’ll answer why.
Sources:
Johns Hopkins Medicine,
American Journal of Respiratory and Critical Care Medicine, Pulmonary Hypertension Association,
National Center for Biotechnology Information