Mending Holes in the Hearts of Extremely Premature Babies
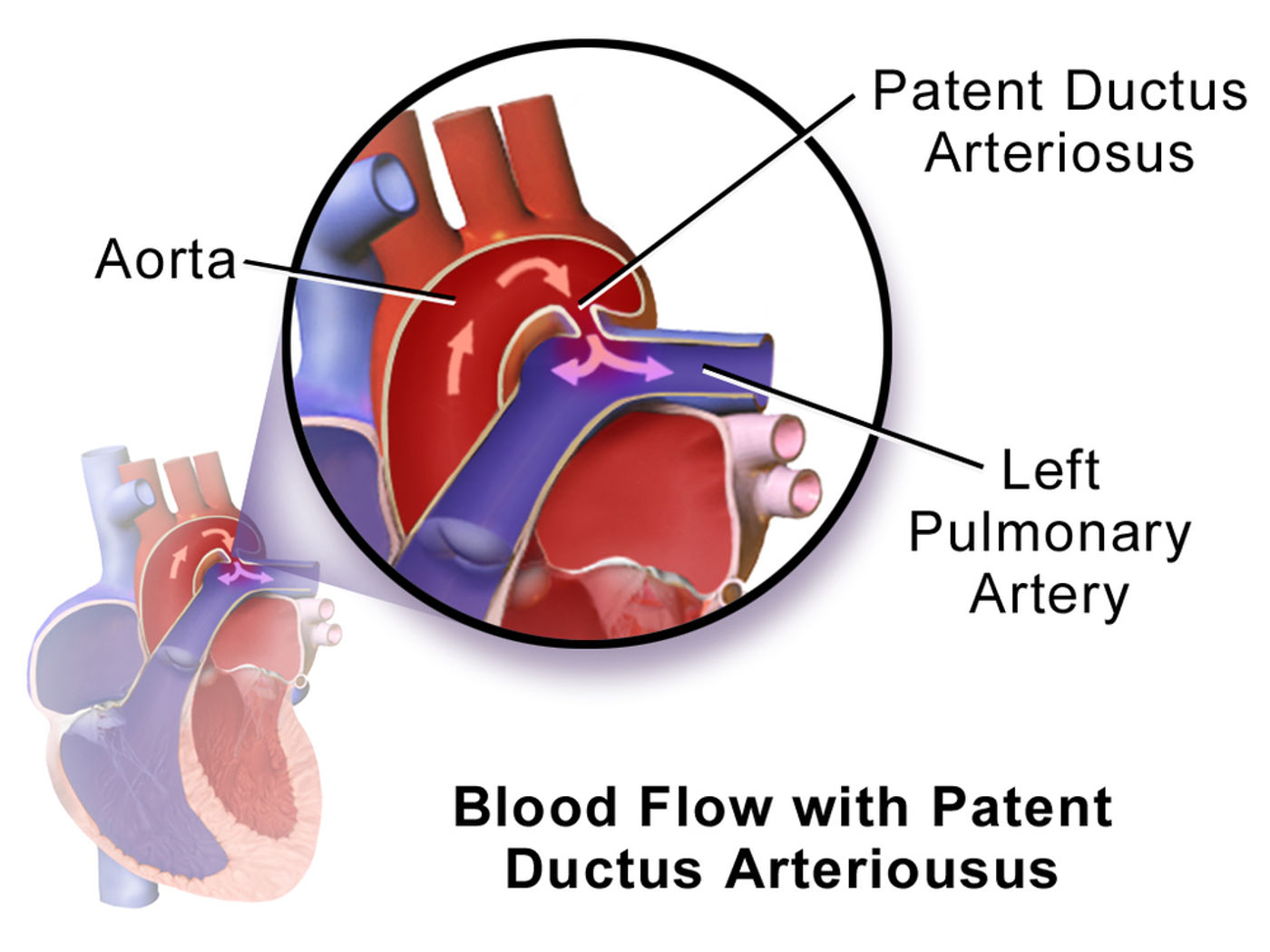
As babies make the transition of depending on the mother for oxygen and depending on their own lungs during birth, an arterial connection has to close on its own. Normally this transition occurs seamlessly, but for premature babies, an unclosed hole can cause major birth defects.
A newly developed procedure for repairing the holes, a condition defined as patent ductus arteriosus (PDA), eliminates the need for dangerous surgery and ineffective medication to give premature babies a better chance at living a full life.
The new procedure is a minimally invasive, transcatheter-based approach for PDA, the most common cardiac birth defect in extremely premature newborns. The nonsurgical repair technique is what Eduardo Marbán, MD, PhD, director of the Cedars-Sinai Heart Institute, calls a “sea change in the treatment of congenital heart disease.”
The procedure involves a catheter, inserted through a vein in the leg and guided by ultrasound waves, that makes its way to the heart to close the hole. This can be successfully performed bedside in a neonatal intensive care unit (NICU) in just a few minutes. So far, the procedure has had a high success rate in newborns as small as 1.6 pounds only a few days old.
“If left untreated, PDA can cause heart failure and lifelong complications," said Evan M. Zahn, MD, an expert in the field of congenital heart disease, namely catheter-based interventions. "Current treatment options are not optimal and are fraught with complications."
Current interventions for PDA include medication and surgery. Medication is only successful in no more than 60 percent of newborns and causes side effects like kidney failure and bleeding. Surgery is accompanied with short-term risks associated with all surgeries and exacerbated by the fragility of the premature newborns. Untreated PDA causes difficulty with breath and feeding, brain hemorrhages, and death.
Zahn and his research team performed the procedure in 24 extremely premature infants, meaning they were morn after only 24 to 32 weeks’ gestation. The procedure was successful in 21 of the infants. Although the catheter-based procedure was not successful in the three remaining infants, the babies did experience successful surgical repair just a few days later.
This new procedure can also be done in PDA patients who don’t receive a diagnosis until later in life. Zahn said that “"it is always better for the patient when we can treat a condition without subjecting the patient to the risks and discomfort of surgery."
“As Dr. Zahn and his team further develop these techniques, parents will no longer have to choose between the risks of surgery and the risks of medications,” Marban said. “And babies will get a healthier start in life.”
Zahn’s study was recently published in the Journal of the American College of Cardiology: Cardiovascular Interventions.
Sources: Cedars-Sinai Medical Center, National Heart, Lung, and Blood Institute, American Heart Association