What Happens To Your Brain After Cardiac Arrest?
Only 25 percent of adults will survive an in-hospital cardiac arrest, and even then the damage done to the brain can have lifelong consequences. Plus, out-of-hospital cardiac arrests, which are much more common, have an even lower chance of survival - about 12 percent. For those that do make it through, it’s difficult for physicians to predict how patients’ brains will heal. In a new study, scientists aim to improve methods used to predict brain healing and function in the months and years following cardiac arrest.
From Johns Hopkins University School of Medicine and the Radiological Society of North America, lead author of the new Radiology study Robert D. Stevens, MD, is looking for better ways to predict outcomes and guide treatment plans for cardiac arrest patients. "We need better methods to help clinicians understand the magnitude of these injuries and make more accurate predictions on recovery, thereby enabling more informed decision-making,” he explained.
It’s important to understand the distinction between heart attack, which is caused by a blockage in the blood vessels, and cardiac arrest, where the heart stops pumping completely, as a result of an irregular heartbeat. Learn more about the difference between these two conditions. Brain damage from cardiac arrest occurs because the brain is one of the many organs starved for oxygen when blood flow - and the heart - stops pumping. Learn more about what happens after cardiac arrest.
In a study of 46 comatose post-cardiac arrest patients, Stevens and his team measured and analyze the brain’s functional connectivity using advanced MRI techniques:
-
Diffusion tensor imaging
-
Resting-state functional MRI (fMRI)
These imaging techniques focused on several neural networks well-understood by scientists, including the “default mode network,” which is active when a person is “not engaged in a specific task,” and the “salience network,” where parts of the brain sift through different stimuli to decide the few that are important to focus on.
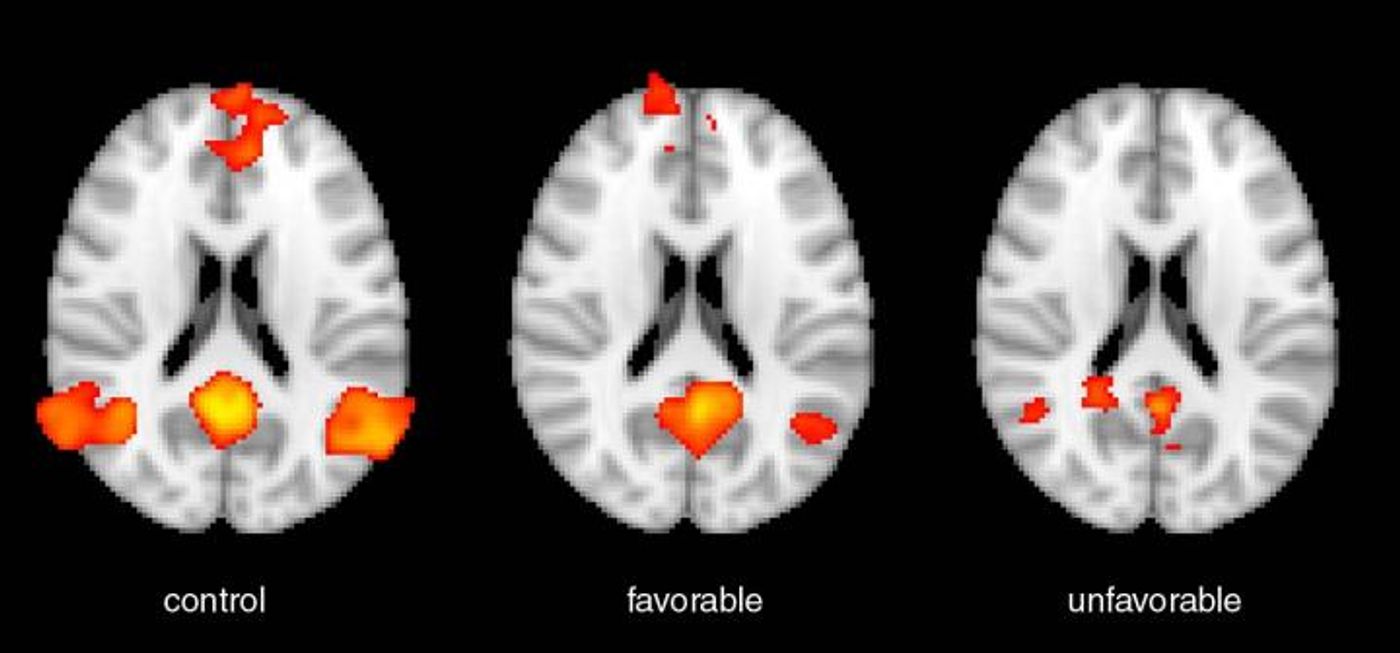
Functional MRI activation (shown as red-orange) as seen in a representative healthy control subject (left), a cardiac arrest patient who had a good functional outcome (middle), and a cardiac arrest patient who had a poor functional outcome (right). Credit: Radiological Society of North America
The imaging was done within two weeks of each patient’s cardiac arrest, and after one year, researchers followed up with an assessment of neurological function, using the “Cerebral Performance Category Scale,” which is commonly used with cardiac arrest survivors.
Out of the 46 original patients, 11 performed particularly well on the test, with strong functional connectivity associated with high levels of independence. Compared to the data collected with advanced MRI techniques nearly a year earlier, researchers found that the functional MRI techniques proved to be much more accurate in their prediction of functional connectivity changes in the brain than structural MRI tests.
"This is game-changing information about what happens in the brains of people who suffer cardiac arrest," Stevens said. "We realize that network architectures can be selectively disrupted in this setting."
In the future, physicians could depend on advanced MRI techniques to provide patients and their families with information about the future of their health, as well as aid treatment plans based on how well they know the brain will heal.
Sources: American Heart Association, Radiological Society of North America