Learning More About the Causes of Endometriosis Pain
It’s estimated that as many as 176 million women suffer from endometriosis, which can be an extremely painful disorder that significantly impacts quality of life, and is described in the video. Now scientists have learned more about the cause of this pain, which can help improve diagnostics and treatments for the disorder. The findings have been reported in The FASEB Journal.
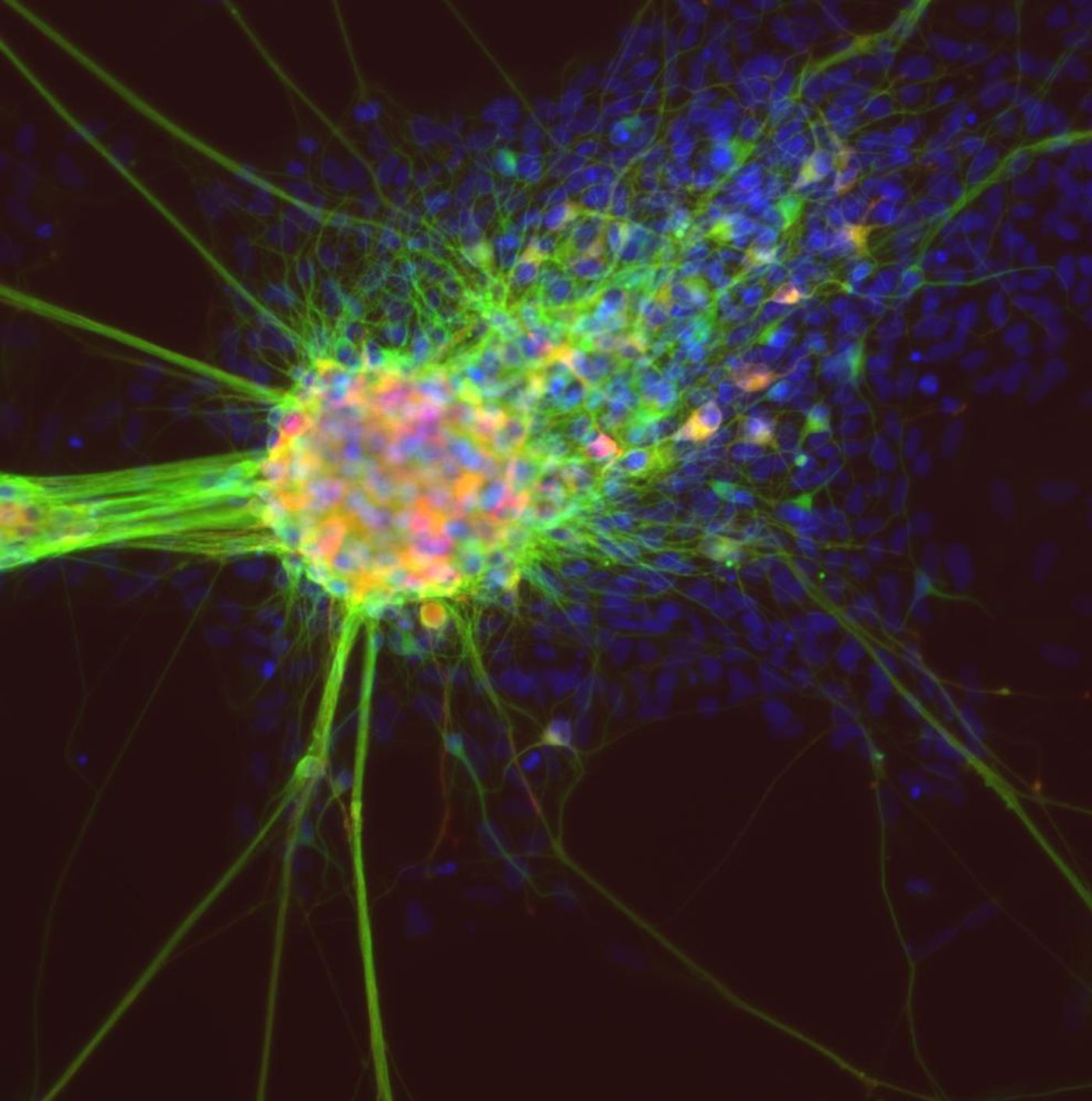
In endometriosis, the tissue that lines the uterus - the endometrium begins to grow on the outside. It still behaves like the uterine lining, however, and thickens and breaks down, but has nowhere to go. When the ovaries are impacted, cysts can form and irritate the adjacent tissue, causing lesions and scarring. This painful condition, which may cause infertility, can only be treated by surgically removing the lesions or administering drugs to reduce the production of ovarian hormones; better options are needed.
“Endometriosis is sometimes considered a hidden disorder because of a reluctance to discuss what can be passed off as women's problems,” noted the lead study author Dr. Erin Greaves of Warwick Medical School. “Hormonal solutions rely on suppressing ovarian function but are not ideal as they can cause unwanted side effects, and prevent the user from becoming pregnant. We are trying to find non-hormonal solutions.”
Scientists in the Greaves lab in collaboration with researchers at the University of Edinburgh have found that the functions of immune cells called macrophages are altered by endometriosis. The cells are attracted to the lesions caused by the disease, and many can reside there. When scientists cultured some of these altered macrophages, they determined that they had ramped up production of a molecule called insulin-like growth factor-1 (IGF-1). When neurons were exposed to this IGF-1, it encouraged growth and activation. It illustrated how macrophages can lead to pelvic pain and sensitivity in endometriosis.
The researchers followed up with patients, assessing their peritoneal fluid for IGF-1. It seems that higher levels of IGF-1 correlated with patients reporting higher pain levels.
This is the first study that has connected endometriosis and macrophages, though the immune cells have been linked to other chronic pain conditions.
“If we can learn about the role of macrophages in endometriosis then we can distinguish them from healthy macrophages and target treatment to them,” said Greaves. “Macrophages are so crucial to our immune system tissue function and we need to know more about their roles, so this research goes some way in defining how macrophages are different in endometriosis.”
In the macrophages in endometriosis lesions, gene expression changes. This can not only contribute to increased pain and sensitivity, it might also serve as a biomarker of disease severity or treatment approaches.
“Endometriosis can affect women throughout their lives and is a very common condition,” Greaves added. “This discovery will go some way towards finding ways to relieve symptoms for women who suffer from endometriosis. We hope that in the future we can learn exactly how disease-modified macrophages in endometriosis promote disease and how we can target them in order to treat endometriosis.”
Sources: AAAS/Eurekalert! via University of Warwick, The FASEB Journal