Discovery of Cell's Mechanism for Sensing Oxygen Wins Nobel
Dr. William G. Kaelin Jr. of the Dana-Farber Cancer Institute, Dr. Gregg L. Semenza of Johns Hopkins University, and Dr. Peter J. Ratcliffe of Oxford University have won the 2019 Nobel Prize in Physiology or Medicine for their discovery of how cells sense oxygen and react to low oxygen levels (hypoxia). This work “revealed the mechanism for one of life’s most essential adaptive processes,” said the Nobel committee.
“Applications of these findings are already beginning to affect how medicine is practiced,” said Randall Johnson of the Karolinska Institute in Stockholm, who was part of the prize selection committee.
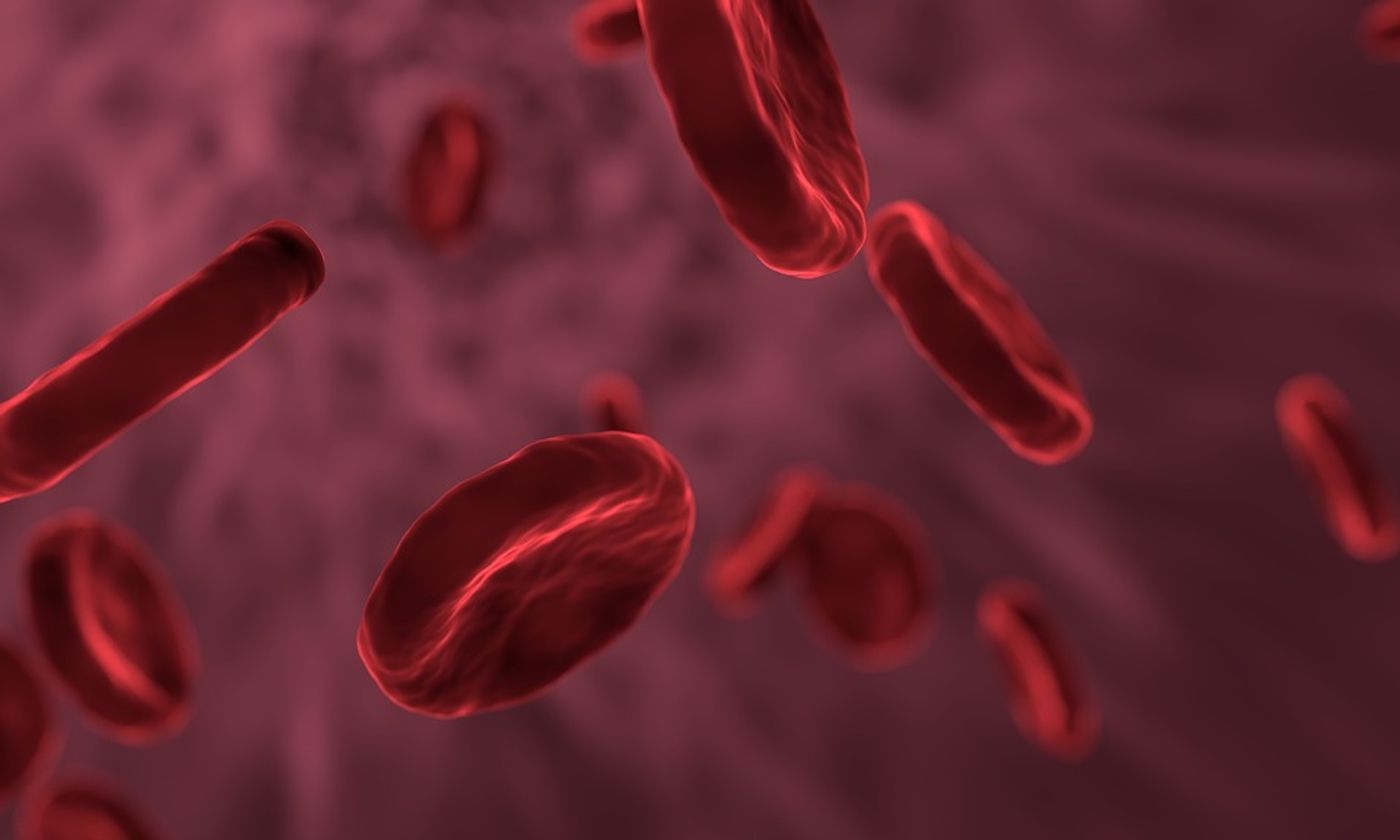
When people live at high altitudes, their cells have to deal with the conditions - there’s less oxygen available in that environment. Wounds that disrupt blood supply can also interfere with oxygen levels, which might trigger the body to generate new blood vessels, produce more red blood cells, or cause an immune response.
Semenza identified the hypoxia-inducible factor (HIF) protein, which attaches to a regulatory part of a gene called EPO when oxygen levels are low. One part of HIF, called HIF-1alpha, directly senses oxygen. Independent work by the three researchers showed how amino acids in the protein change in normal conditions, which leads to the disposal of HIF-1alpha. In low-oxygen states, however, the amino acids remain unchanged, and HIF-1alpha ends up moving to the nucleus, where it changes the expression of hundreds of genes, including EPO.
Kaelin’s work showed that cancer cells that lack a protein involved in this mechanism can activate genes related to hypoxia. Science magazine explains the work in detail here.
This research can open up new avenues in drug development. It may be possible to attack cancer or treat anemia or other diseases by interfering with a cells’ ability to sense oxygen. In China and Japan, a drug has been approved for the treatment of anemia, which is sometimes seen in chronic kidney disease. The drug is expected to be approved in the U.S. soon, Kaelin said. Reduced blood flow after a heart attack or stroke can lead to the loss of limbs, and this research could help patients with those conditions as well.
Ratcliffe began his work as a kidney specialist; he just wanted to know how cells sensed the oxygen levels in their environments.
“I thought it was a definable problem and just thought we’d find out how it worked,” he said. About two years into his team's work, which started decades ago, they began to see that it had wider applications, Ratcliffe added.
“We saw that it wasn’t just cells in the kidney that know how to sense oxygen, but all cells in the body. ... There are hundreds and thousands of processes the body uses to adapt to and regulate its oxygen levels.”
It will still be years before the full ramifications of the research can be realized and brought to the clinic for the benefit of thousands of patients, he acknowledged.
Semenza said that their work would probably be useful in the treatment of kidney cancer first. A therapeutic based on their research has the potential to make chemotherapy more effective. He is hopeful that people with other kinds of cancer will soon benefit as well.
Semenza credited his high school biology teacher, Rose Nelson, for the inspiration to embark on a career in medicine.
“She used to say, ‘Now when you win your Nobel Prize, I don’t want you to forget that you learned that here,’” Semenza said. “It’s my great sadness that she is not still alive to share the moment because I know it would have meant a lot to her. She was my inspiration. That’s the importance of teachers,” he added. “To make that kind of spark.”
The mechanism the researchers revealed is widely found in animals, noted Steven McKnight of the UT Southwestern Medical Center in Dallas. He said the Nobel-winning work is “of a heroic nature.”