There's More to Neutrophil Function Than We Knew
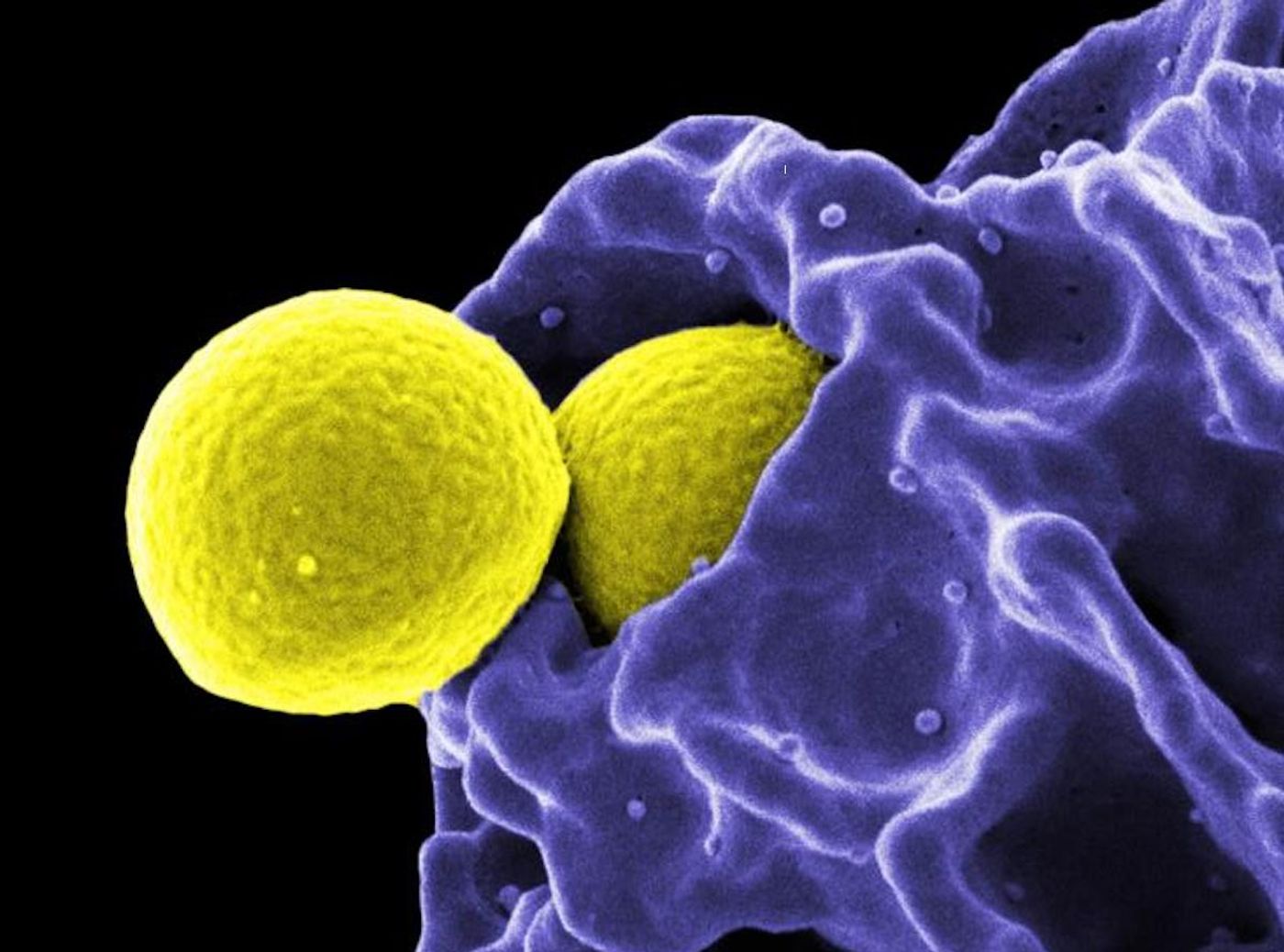
Neutrophils are the most abundant type of white blood cell that circulates in the blood, defending against pathogenic invaders; they can engulf and destroy foreign microbes. They can also help repair wounds. New research has shown they may have many more functions than we knew and seem to be involved in the maintenance of organs. Reporting in Cell, this work could have implications for the treatment of diseases including cancer.
Our adaptive immune system can form memories of infections so the body responds to a pathogen more quickly the second time it's encountered. Lymphocytes like T and B cells are part of this system. The innate immune system, meanwhile, can defend the body in a more general, non-specific way. White blood cells like neutrophils are part of innate immunity.
"Lymphocytes produce antibodies or receptors that specifically target viruses or bacteria to build immunity against these pathogens. The cells of the innate immune system, on the other hand, provide a faster but nonspecific response that can sometimes trigger uncontrolled inflammation, as happens in the lungs of patients with severe COVID-19, for example," explained lead study investigator Dr. Andrés Hidalgo of Centro Nacional de Investigaciones Cardiovasculares (CNIC).
Neutrophils are produced in huge quantities by the bone marrow, and every day, large amounts of these cells move into the bloodstream and out to most tissues. They have to be constantly replenished because a neutrophil only hangs around for about 24 hours. That is thought to be a reason why neutrophils have a limited ability to adapt and take on new functions.
In this work, however, the researchers saw differently. "We found that when neutrophils leave the circulation and migrate into tissues they acquire new, previously unknown properties," said Hidalgo.
"What is fascinating is that neutrophils appear to acquire functions useful to the specific tissues in each organ. For example, we found that neutrophils in the lung acquire the ability to contribute to the formation of blood vessels, whereas neutrophils in the skin help to maintain the integrity of the cutaneous epithelium," noted Hidalgo. "This ability to change cell properties was identified in healthy individuals, which suggests that neutrophils participate in a great variety of normal functions in the body and are not limited to combating infection."
The innate immune system may not only use general strategies and is likely capable of a targeted response. "This is particularly exciting because if we can define the mechanisms that control how these cells acquire new functions we will be able to design new treatments to exploit this plasticity of neutrophil responses for the benefit of patients," suggested the co-first study author Iván Ballesteros.
"The results show that neutrophil immune plasticity is not dependent on the presence of disease, suggesting that it has beneficial functions that sometimes get short-circuited in pathological settings," Ballesteros added.
Cancerous tumors have to get around the immune system to create a blood supply for themselves. Neutrophils may also become heterogeneous during disease, and these changes are seen in cancer and after bone marrow transplants. Not much is known about the mechanisms underlying these observations, however.
"Essentially, what we have demonstrated is that neutrophils, despite their [short] lifespan, can change their function and that they do this when they enter tissues. The identification of these adaptations allows a better understanding of the roles of different immune cells in disease," noted Andrea Rubio, CNIC bioinformatician and co-first study author on the study.
Sources: AAAS/Eurekalert! Via Centro Nacional de Investigaciones Cardiovasculares Carlos III (F.S.P.), Cell