The Cause of Post-Surgical Scarring, Revealed
Our bodies can heal many injuries we endure, and while the process often works well, problems can also arise. After abdominal and pelvic surgery, for example, a common complication called adhesions can arise in which excess scarring occurs in the peritoneal cavity. That's a space between membranes that surround the abdomen.
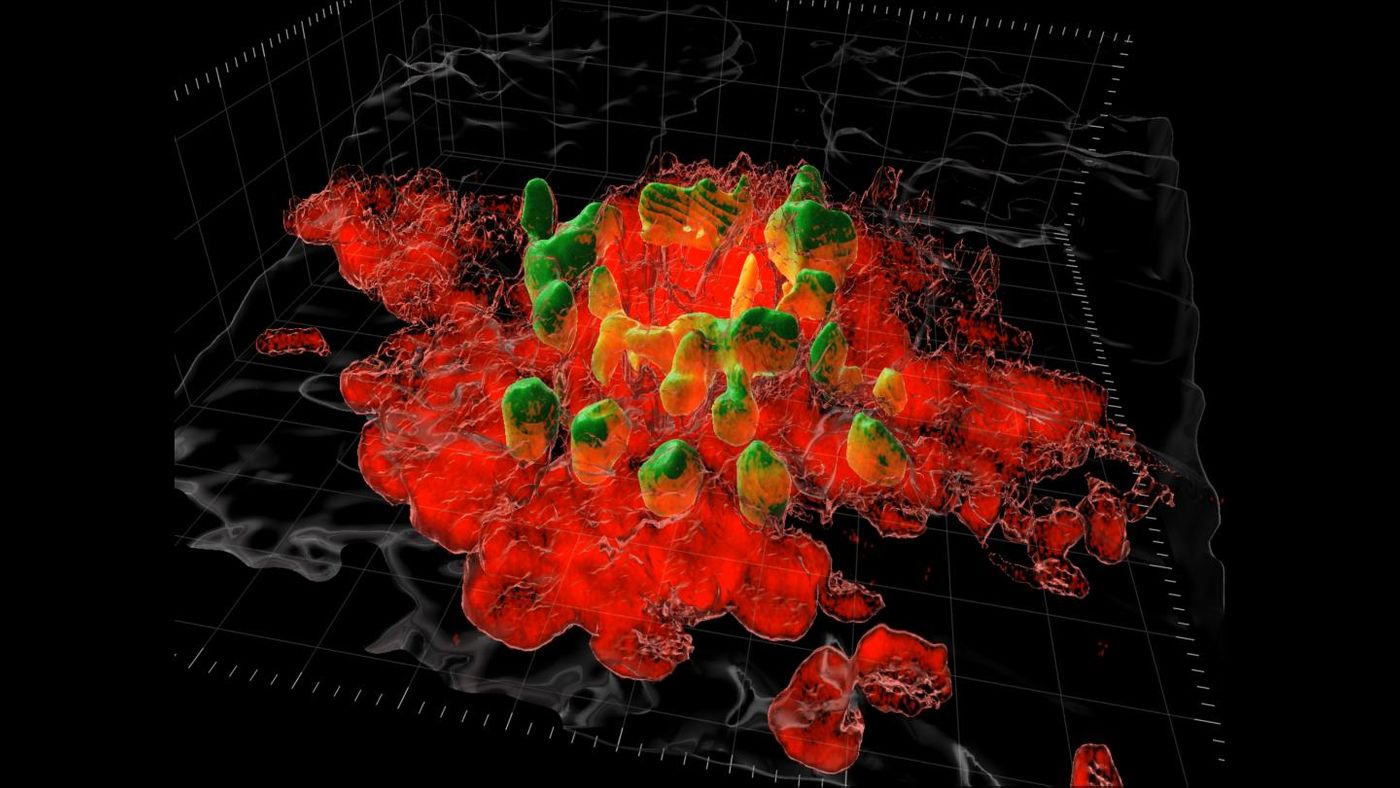
Reporting in Science, researchers have now used a mouse model to show that the excessive post-surgical scarring or adhesions in the peritoneal cavity is caused by a type of immune cell called macrophages, which form structures that resemble clots. These white blood cell aggregates may help the healing and they can plug wounds, but their activity also has to be carefully controlled by the body.
"This is a worldwide concern. Complications from these peritoneal adhesions cause pain and can lead to life-threatening small bowel obstruction, and infertility in women," explained first study author Dr. Joel Zindel, M.D. of the University of Bern who worked on this research at the University of Calgary. "People sometimes require a second surgery."
In this study, the researchers used intravital imaging, which enables the visualization of the cells in a live animal. In this technique, a special surgery implants a window into a mouse, often a model organism that expresses a protein tagged with a fluorescent protein.
"Joel developed a new method using the highly specialized imaging equipment in my lab that gave scientists the first look at what these macrophages are doing in real-time," noted principal study investigator Dr. Paul Kubes, Ph.D., a professor at the Cumming School of Medicine. "We are still working to understand why the macrophages take on this repair work as they are known for attacking pathogens. Whatever they are responding to, it's clear their involvement is causing the scarring problem."
This work also showed that these abdominal scars or adhesions could be stopped by removing macrophages, or by using a drug that prevented the macrophages from getting sticky.
"We believe the macrophage response has not made the evolutionary leap to understand that surgery is beneficial and not a threat to survival," said Kubes. "It's possible, that the body is reacting to the surgery, that having the organs exposed to the environment is interpreted as a threat, like an attack from a predator. The body doesn't understand that the surgeon will do the critical repair work."
Since macrophages are found in humans, the researchers suggested that this work will apply to people, and they are hopeful that trials evaluating drugs that prevent stickiness in human macrophages will start soon.
"Every surgeon does operations for people who have these abdominal adhesions," said Zindel. "It would be amazing to be able to prevent this surgical complication. It would not only benefit individuals, it would create significant savings for the healthcare system, by reducing hospital costs for readmission and surgery."
Sources: AAAS/Eurekalert! via University of Calgary, Science