Stem Cell Treatment for Dementia is Promising in Model
Reporting in Science Translational Medicine, researchers have now determined that an experimental stem cell therapy successfully repaired brain damage and improved memory function in a mouse model of stroke and dementia. Dementia is thought to affect 5 million Americans, and more are diagnosed every day as the population ages. There is a spectrum of symptoms associated with the disorder, including attention, memory, communication, and physical problems. Alzheimer's disease and small strokes in the brain's white matter are the most common causes of dementia.
"It's a vicious cycle: The two leading causes of dementia are almost always seen together and each one accelerates the other," said senior study author Dr. S. Thomas Carmichael, interim director of the Eli and Edythe Broad Center of Regenerative Medicine and Stem Cell Research at UCLA.
In this work, the researchers utilized a special type of cell known to support neurons, called glial cells. Mice with brain damage were given injections of these special glial cells directly to their brains.
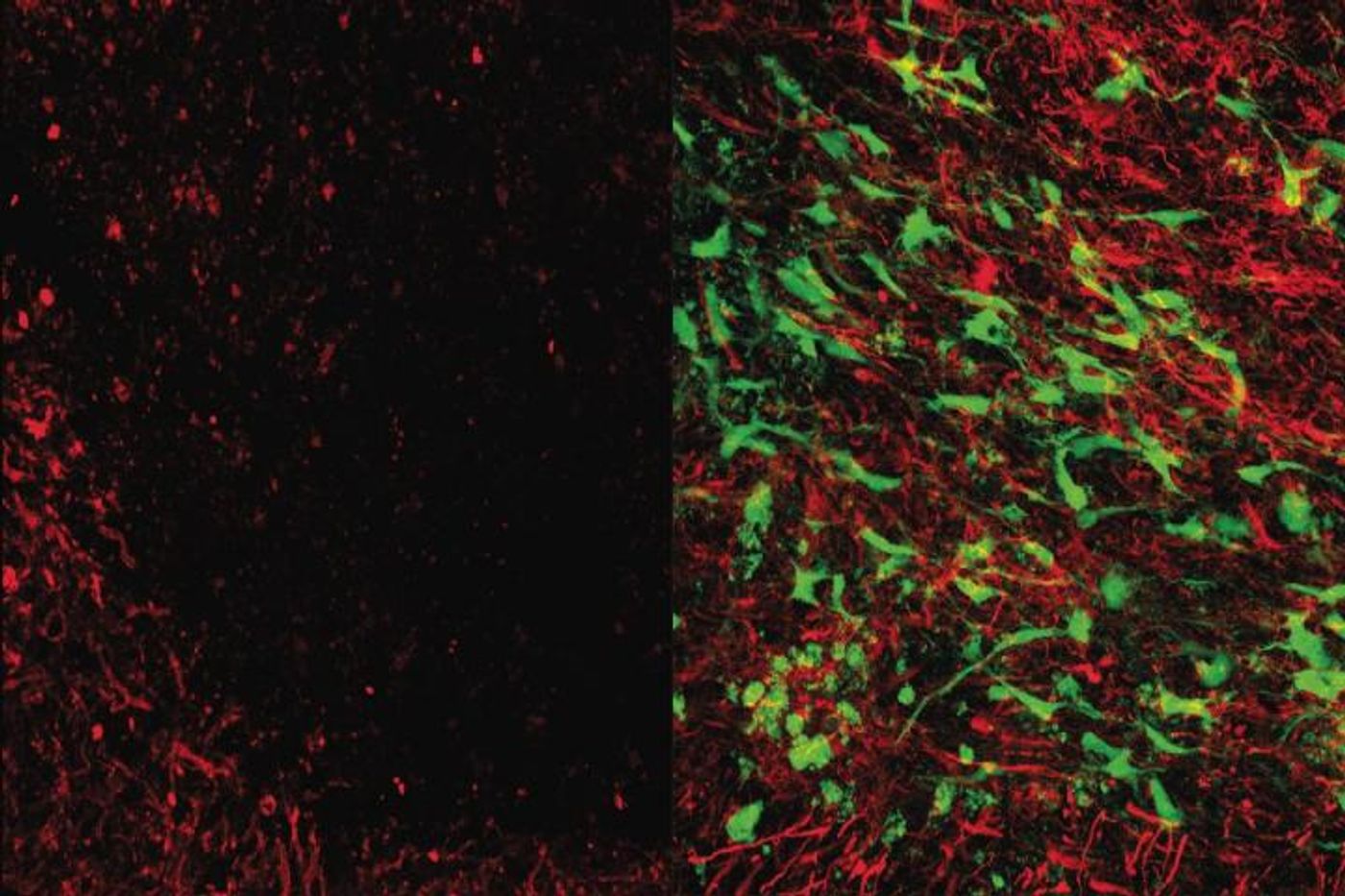
"Upon injection, our cell therapy traveled to damaged areas of the brain and secreted chemicals called growth factors that stimulated the brain's stem cells to launch a repair response," said first study author Dr. Irene Llorente, an assistant research professor of neurology at the David Geffen School of Medicine at UCLA.
When the repair process was triggered, brain damage was limited, and the formation of new neural connections was enhanced. The production of a sheath that protects neurons called myelin was also increased.
"Understanding the role that glia play in repairing white matter damage is a critically important area of research that needs to be explored," noted Francesca Bosetti, a program director at the National Institutes of Health's National Institute of Neurological Disorders and Stroke, a study funder. "These preliminary results suggest that glial cell-based therapies may one day help combat the white matter damage that many stroke and vascular dementia patients suffer every year."
Right now, there are no treatments that enhance the brain's regenerative capabilities or halt the dysfunction caused by white matter strokes. This work may help change that, although this approach still needs to be evaluated in humans. The researchers are hopeful that it will one day be especially useful in clinics because it does not require each treatment to be tailored to the patient; it may be less expensive and more accessible, and it would be faster to apply.
"The damage from white matter strokes is progressive, so you don't have months to spend producing a treatment for each patient," noted Carmichael. "If you can have a treatment that's already in the freezer ready to go during the window of time when it could be most effective, that's a much better option."
The researchers also found that the positive results from the treatment were maintained even when the transplanted cells were removed. The therapy was stimulating natural repair processes in the brain.
"Because the cell therapy is not directly repairing the brain, you don't need to rely on the transplanted cells to persist in order for the treatment to be successful," Carmichael said.
The researchers are hoping to get approval to start clinical trials soon.
Sources: AAAS/Eurekalert! via University of California - Los Angeles (UCLA) Health Sciences, Science Translational Medicine