Some say eyes are the window to your soul. Eyes can tell you a lot about your health as well. Eye doctors have been able to see signs of blood pressure issues, autoimmune disorders, and even infection just by what is going on in your eyes.
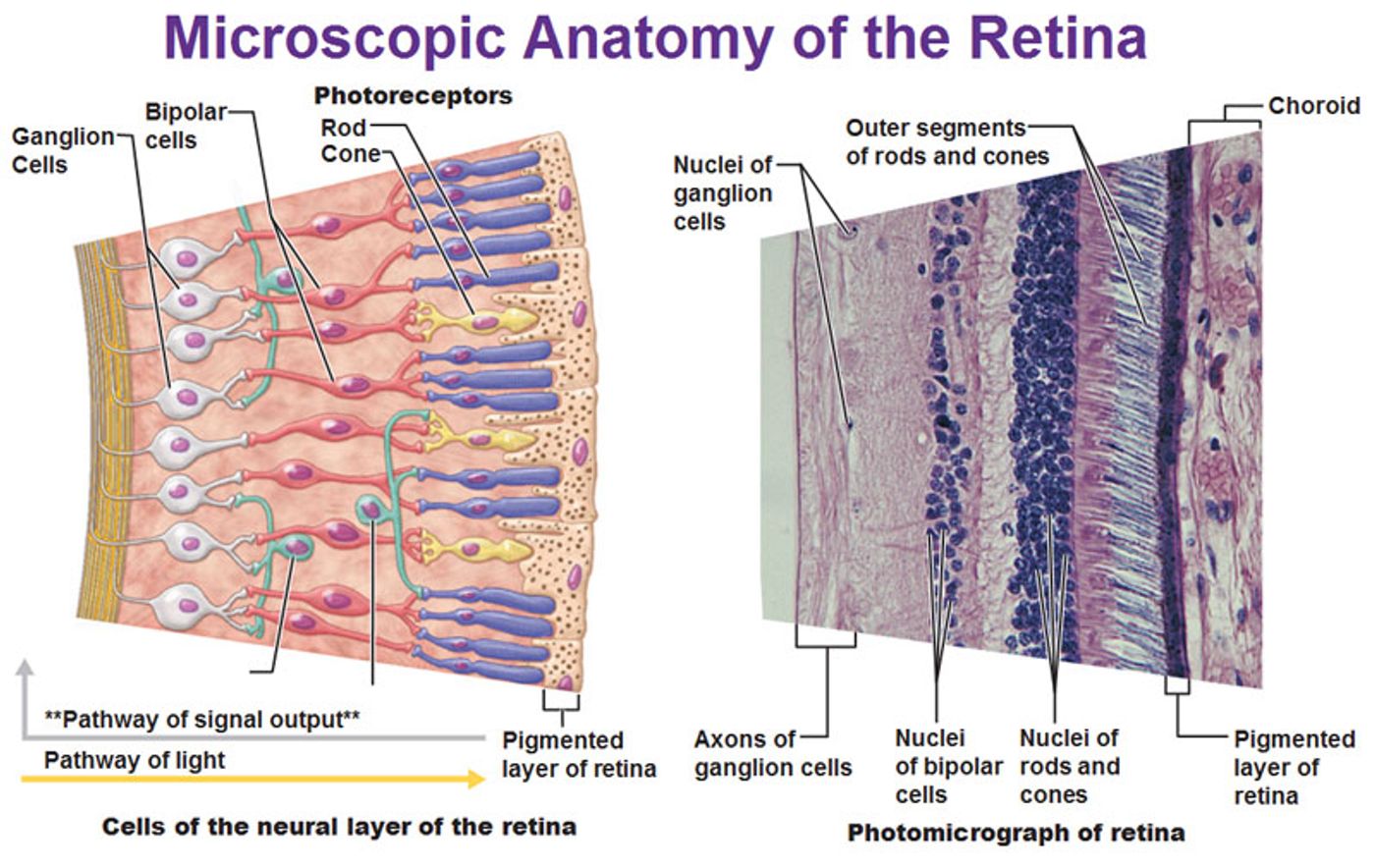
The retina plays an important role in vision, taking in light and converting stimuli into electrical signals sent to the brain to construct images. Retinal diseases usually result in blindness due to the importance of the retina in gathering and converting visual information. For example, diseases such as macular degeneration and glaucoma stem from damaged or older retinal cells that cannot regenerate.
A new study from researchers at the Yale University School of Medicine published in
Cell Reports is examining the regeneration capabilities of certain retinal cells in zebrafish and looking to stimulate regeneration in human retinal cells.
A specific type of retinal cells, called Muller Glial cells (MGs), provide structural support and maintain homeostasis for retinal neurons. Unlike MGs in zebrafish, MGs in mammals lack any regenerative capability except when injured, when these cells can spontaneously re-enter stem cell status resulting in regeneration. However, only stimulating regeneration after injury is counterproductive to the cells since injury would most likely result in severe retinal cell death.
A team led by Dr. Bo Chen, Associate Professor of Ophthalmology at Yale, hypothesized that if species such as zebrafish have this regenerative capability, and if human retinal cells can be stimulated to regenerate through injury, there must be an activation pathway to stimulate regeneration in human retinal cells directly without injury. The ability to activate this biological pathway could be used in therapies for retinal diseases to rebuild a healthy retina.
Based on previous studies showing that a certain Wnt signaling pathway is activated in zebrafish retinal stem cells, the team characterized this same pathway as the one activated in mammalian cells after cell injury, promoting injury-induced MG cell proliferation. The researchers then wanted to find a way to stimulate this Wnt pathway in the absence of injury. Using cell-type specific gene transfer methods, they were able to determine the specific protein activators and regulators of the Wnt signaling pathway in mouse and human MG cells. Deletion of an identified pathway regulator resulted in activation of the pathway and proliferation of the MG cells.
Success of this experiment and further signaling pathway studies could have a big impact on therapy development to treat the vision of people with advanced retinal diseases.
“In the future we are hoping to manipulate these cells to replenish any lost retinal neurons, either in diseased or physically damaged retinas,” Chen noted. “Potentially, it’s a therapy to treat many different retinal degenerative diseases.”
Sources:
YaleNews,
Cell Reports,
Mayo Clinic,
Blindness.org