New work reported in Developmental Cell by researchers at Johns Hopkins University has demonstrated that a protein known to control nerve cell development also acts on the pancreas, prompting the release of insulin. Insulin helps the body maintain the proper level of sugar, or glucose, in the bloodstream, and that process goes wrong in diabetes. This new work could potentially lead to new treatments for the diabetes one day. The short video below from the Centers for Disease Control outlines the basics of diabetes.
Type-2 diabetes is the most common form of the disorder, and affects almost ten percent of Americans. Unlike type-1 diabetes, in which the body no longer produces insulin, in type-2 the body still makes insulin, just not enough of it, or uses it inefficiently. Type-2 diabetes can appear at any time of life and is on the rise worldwide, making it a growing public health problem.
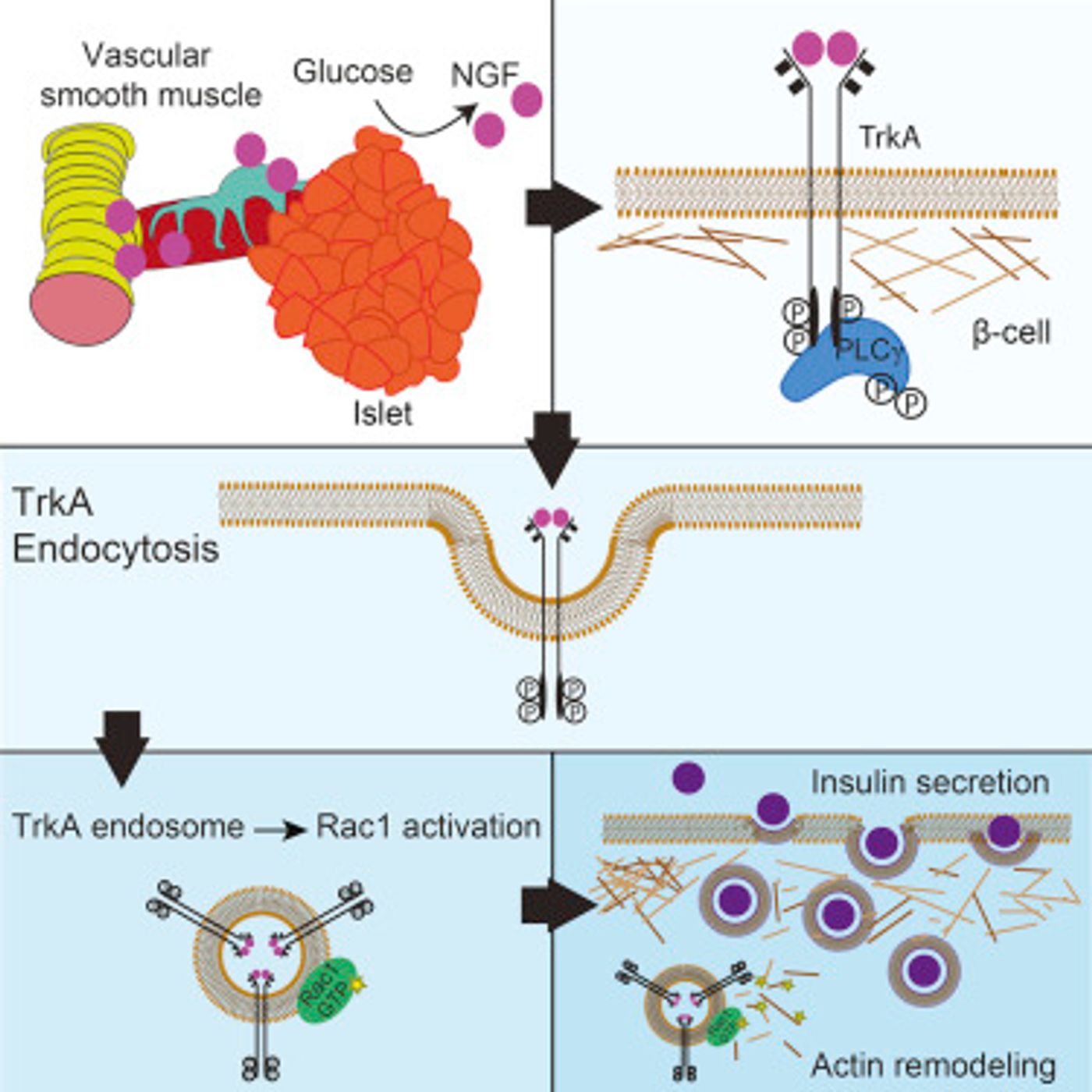
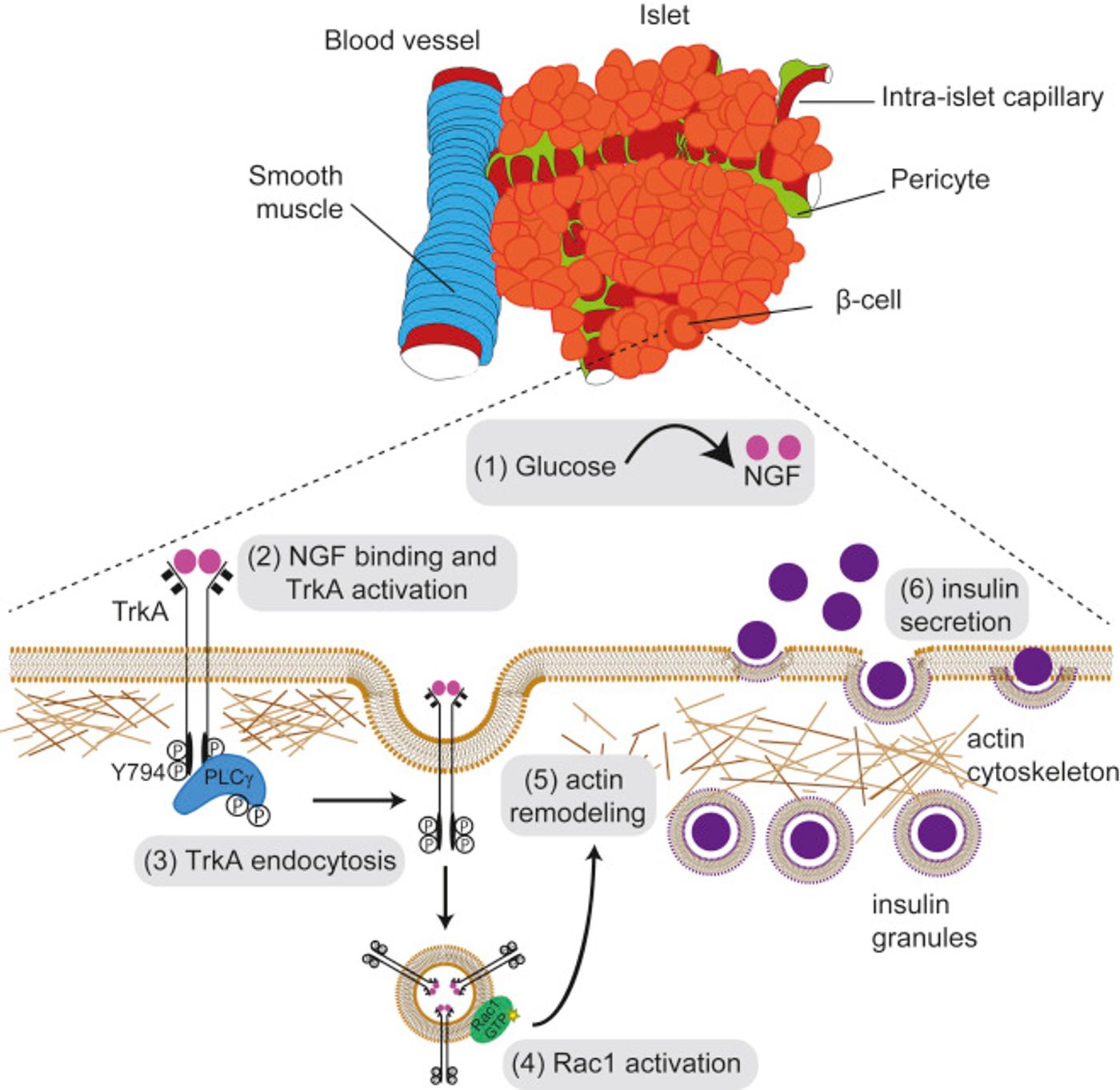
It has been known for many years that pancreatic beta cells, which produce insulin, have many signaling receptors and a molecular composition that are similar to neurons. Those receptors are critical for the coordination of biochemical cascades and pathways. Beat cells of the pancreas and neurons both have receptors for picking up neurotrophins – proteins that stimulate the development, maintenance and functions of neurons.
One author of this new work has spent a lot of research time on developing neurons of the peripheral nervous system. Rejji Kuruvilla of the Department of Biology at Hopkins has studied neurotrophins and particularly, nerve growth factor (NGF), in depth. "This project was sparked by seeing NGF receptors present in beta-cells," said Kuruvilla. The researchers wanted to know: "What are these receptors doing outside the nervous system?"
The investigators found that NGF has a role in the pancreas that is unrelated to neurons. They learned that elevated blood glucose levels cause the release of NGF from pancreatic blood vessels. The NGF causes the beta cells in the pancreas to ease their rigid structure, which releases insulin particles into the blood stream. While beta cells do make NGF, the scientists determined the NGF that came from the blood vessels is what is required for the secretion of insulin.
By altering genes and using pharmacological agents in mice, the researchers disrupted NGF signaling in beta cells. Their work confirmed that the NGF pathway is required in mice for enhanced insulin release and glucose tolerance. Critically, Kuruvilla’s team determined that the NGF effect of enhanced insulin secretion due to high glucose also happens in human cells.
It remains to be seen how this system is working, or not, in those with diabetes. "We are very interested in knowing whether aspects of this pathway are disrupted in pre-diabetic individuals," Kuruvilla concluded.
Figuring out whether NGF or other molecules that can bind and activate NGF receptors in the pancreas might be useful in type-2 diabetes therapeutics. These, and other questions, shall be pursued in future studies.
Sources:
AAAS/Eurekalert! via
Johns Hopkins,
Journal of Histochemistry & Cytochemistry,
Developmental Cell