Antimicrobials may Stop Sepsis in Pneumonia Patients
Sepsis is a life-threatening condition that happens when the immune system’s response to an infection gets out of control and causes inflammation all over the body. Rapid treatment with antibiotics can help the sepsis patient, but it’s not always effective. New work has shown that treating specific immune cells with antimicrobials could be a way to prevent sepsis in people that are affected by pneumonia. The study, which was reported in Nature Microbiology, has shown that the bacterium that causes pneumonia uses cells of the immune system to multiply, so the infection gains a foothold in the body.
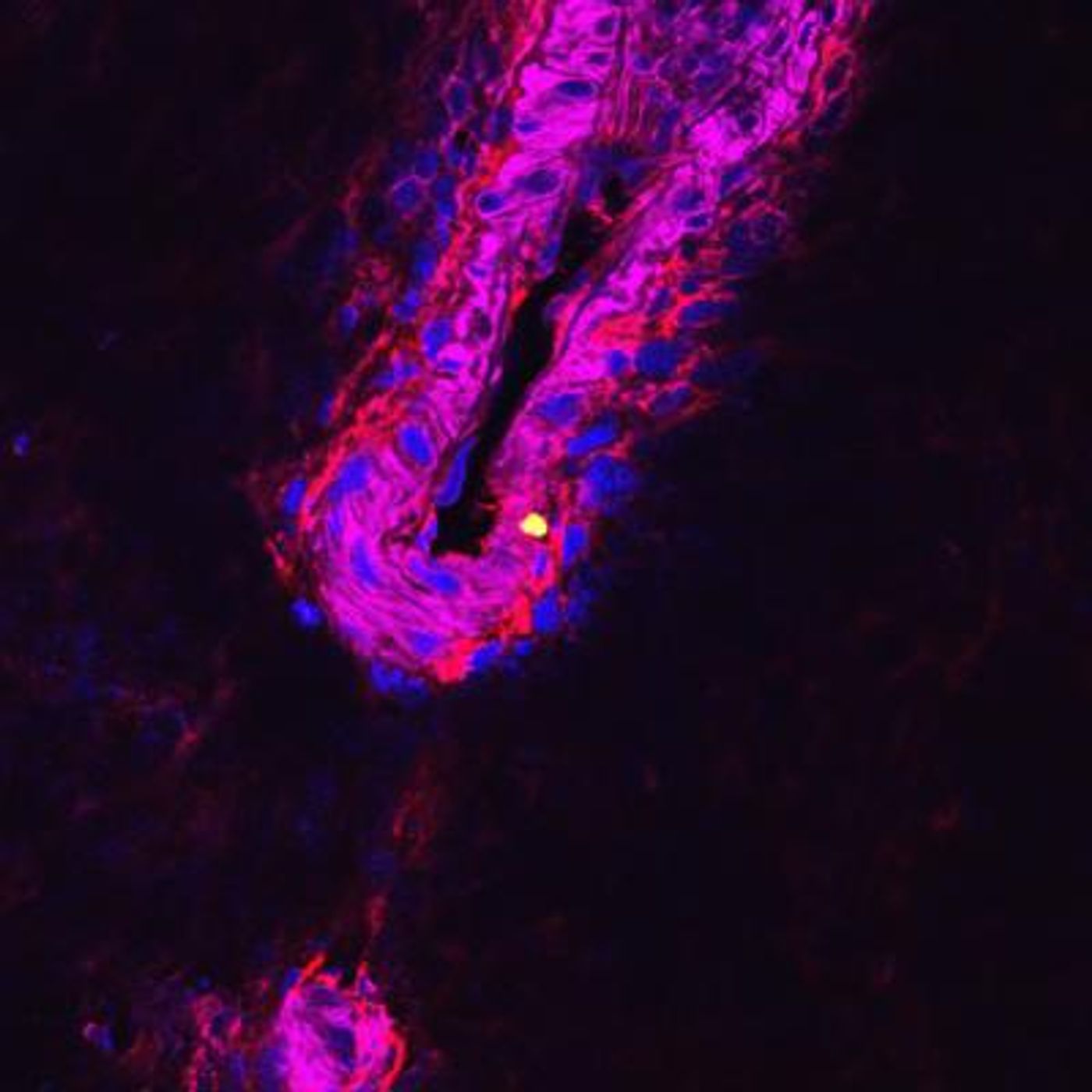
Led by Professor Marco Oggioni, investigators determined that after initial infection, a bacterium called Streptococcus pneumoniae (pneumococcus) uses a specific kind of immune cell, a type of splenic macrophage, to replicate before it launches an invasive illness that can be fatal.
Because the bacterium reproduces inside of this immune cell, it doesn’t get killed by most drugs or by other cells from the immune system.
"Understanding infections is important in determining how best to treat an infection," noted Oggioni, of the University of Leicester's Department of Genetics and Genome Biology. "Our work shows that we can treat potentially deadly infections more effectively using antibiotics that are already available.
The research has also shown that when antimicrobial treatments target specifically this mechanism of replication inside of cells, pneumococcal septicemia, which is common in many pneumonia patients, can be stopped. Pneumonia can cause death and is a serious risk in some groups individuals, like the elderly.
"By discovering the mechanism of how and where bacteria initiate disease, we think we can give a strong message to the medical community to stimulate the revision of currently used therapies and this could potentially result in a reduction of disease burden and mortality in the UK and elsewhere," added Oggioni, who is also an honorary consultant biologist at Leicester's Hospitals.
The researchers used a variety of different models in their experiments and utilized confocal microscopy to observe and track immune cells and the bacteria that were infecting them. A totally new model was also developed, in which surplus pig spleens were obtained from agriculture, and used in the study to mimic an infection in a person, while sparing live animals from the experiment.
Learn more about sepsis from the video.
Sources: AAAS/Eurekalert! via University of Leicester, CDC, Nature Microbiology