Vitamin D May Aid in Treating Diabetes
Diabetes is a growing problem in the United States and around the world. As our population gets older and more overweight, it’s expected that we’ll only add to the 27 million people currently afflicted with type 2 diabetes. The disease is caused by problems in the body’s ability to use insulin to deal with blood sugar. Sometimes insulin becomes less effective, but dysfunction in beta cells, which reside in the pancreas and make insulin, is also a primary cause of diabetes. Now scientists at the Salk Institute have learned more about how beta cells can be protected with vitamin D, which has been previously linked to diabetes.
Reporting in Cell, the researchers used cells in culture and a mouse model to demonstrate that vitamin D can help treat beta cells that have been damaged. They also learned more about how diabetes and vitamin D are connected.
"We know that diabetes is a disease caused by inflammation," explained senior author Ronald Evans, a Howard Hughes Medical Institute investigator and Salk's March of Dimes Chair in Molecular and Developmental Biology. "In this study, we identified the vitamin D receptor as an important modulator of both inflammation and beta cell survival."
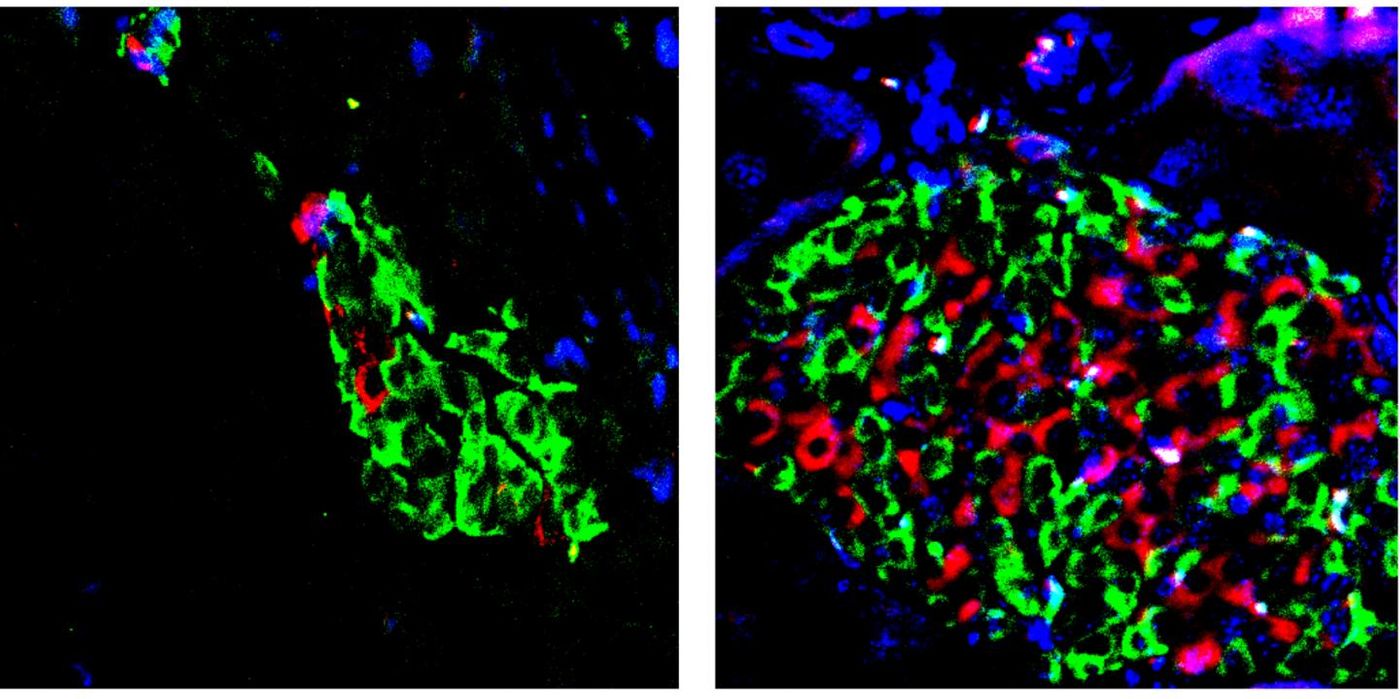
For this work, the researchers created beta cells from embryonic stem cells. They were then able to identify a molecule, iBRD9, that could boost the activation of a receptor that binds to vitamin D. That, in turn, improved beta cell survival when combined with vitamin D.
The compound was found after using a screening test, which sought molecules that helped beta cells survive in a dish. After the screen, a mouse diabetes model was used to test iBRD9 and vitamin D in combination. The researchers saw that glucose levels were brought back to normal.
"This study started out by looking at the role of vitamin D in beta cells," said first author Zong Wei, a research associate in Salk's Gene Expression Laboratory. "Epidemiological studies in patients have suggested a correlation between high vitamin D concentrations in the blood and a lower risk of diabetes, but the underlying mechanism was not well understood. It's been hard to protect beta cells with the vitamin alone. We now have some ideas about how we might be able to take advantage of this connection."
It seems the vitamin D and iBRD9 increase the expression of protective genes in diseased cells. "Activating the vitamin D receptor can trigger the anti-inflammatory function of genes to help cells survive under stressed conditions," noted co-corresponding author Michael Downes, a Salk senior staff scientist. "By using a screening system that we developed in the lab, we've been able to identify an important piece of that puzzle that allows for super-activation of the vitamin D pathway."
These findings show how understanding a fundamental physiological mechanism can improve a wide array of patient therapeutics.
"In this study, we looked at diabetes, but because this is an important receptor it could potentially be universal for any treatments where you need to boost the effect of vitamin D," suggested study co-author Ruth Yu, a Salk staff researcher. "For example, we are especially interested in looking at it in pancreatic cancer, which is a disease that our lab already studies."
The researchers did not find evidence of side effects in their mouse model, but more testing will be required before they move to clinical trials.
A different study by the University of California San Diego School of Medicine and Seoul National University looked at the connection between vitamin D deficiency and the development of type 2 diabetes. That work is briefly outlined in the video and was published in PLOS One.
"Further research is needed on whether high 25-hydroxyvitamin D levels might prevent type 2 diabetes or the transition from pre-diabetes to diabetes," said the co-author of that report, Cedric F. Garland, DrPH, adjunct professor in the UC San Diego School of Medicine Department of Family Medicine and Public Health. "But this paper and past research indicate there is a strong association."
Sources: AAAS/Eurekalert! Via Salk Institute, UCSD, PLOS One, Cell