A Color-Changing "Invisible Tattoo" for Long-Term Health Monitoring
German researchers have developed an innovative method for continuously tracking and monitoring biomarkers and drugs circulating in the body. This implantable device sits under the surface of the skin and measures spikes and dips in the concentrations of these molecules over the course of weeks and months, opening up a wealth of possible applications in personalized medicine or pharmaceutical development.
Conceptually, implantable biosensors for health monitoring have been around for a while. The problem, however, is that once implanted, the body sees them as foreign and rejects them. Here, immune responses activate the formation of fibrous tissue which cocoons the devices’ sensors, rendering them inactive.
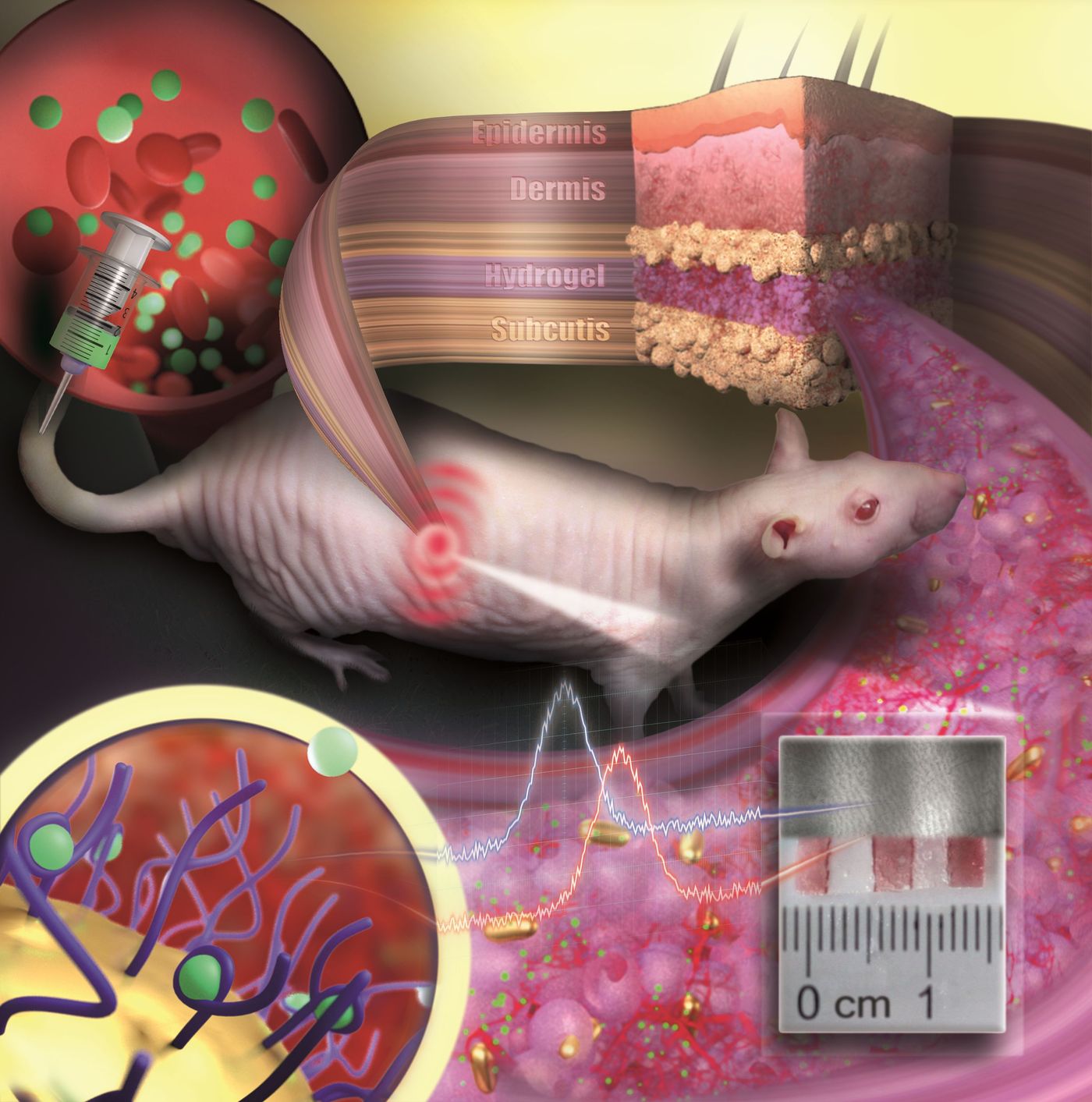
To overcome this problem, researchers at the Johannes Gutenberg University Mainz have turned to nanotechnology. The team created a small device consisting of programmable gold nanoparticles suspended within a hydrogel. This polymeric hydrogel plays a central role in keeping the immune system at bay by acting as a scaffold for blood vessels and other tissues to grow into it.
Tiny blood vessels begin to invade the hydrogel, carrying specific analytes of interest (disease biomarkers, or circulating drugs, for example) toward the suspended nanoparticles. This then triggers a color change in the nanoparticles, a signal output that is influenced by the concentration of the target analyte. This colored signal can then be detected non-invasively through the skin. The research was published in Nano Letters.
“We are used to colored objects bleaching over time. Gold nanoparticles, however, do not bleach but keep their color permanently. As they can be easily coated with various different receptors, they are an ideal platform for implantable sensors,” said one of the device’s inventors, Katharina Kaefer.
Another advantage is that the implants are small and discrete, minimally impacting the user.
“Our sensor is like an invisible tattoo, not much bigger than a penny and thinner than one millimeter,” said another scientist in the study, Carsten Soennichsen. The team validated their device in a hairless rat model where the sensors were programmed to monitor concentrations of an administered antibiotic over the course of several months.
Sources: Nano Letters, MedGadget.