In a move towards objectivity and higher precision, researchers at the University of Georgia have identified a number of brain-based biomarkers that can be used to improve diagnosis of psychiatric conditions.
To diagnose infections, doctors run blood tests. To diagnose brain aneurysms, doctors do comprehensive brain scans. But to diagnose a psychiatric condition, doctors ask how you’re feeling. Progress of medical technologies has made it possible to scan, X-ray, sequence, probe patients in countless ways to get at accurate diagnoses. However, no objective tests exist for diagnosing mental illness.
Instead of quantitative tests, diagnosis of psychiatric conditions is heavily dependent on observable symptoms. Clinicians rely on the Diagnostic and Statistical Manual of Mental Disorders (DSM) to subjectively categorize patients’ symptoms into certain disorders. This system of classifying mental illness has been criticized for being inherently incomplete and often biased. Incidentally, the DSM text is over 60 years old and has had a history of revisions.
"Psychiatry still relies on symptoms as the basis of a diagnosis," said the study's lead author Brett Clementz. "It would be like using the presence of fever to diagnose a specific infection. We need some means to help us more accurately differentiate mental disorders."
Inspired by objectivity of molecular diagnostic tools, the research team set out to identify disease types based on quantitative neurobiological measures. The large biomarker panel consisted of measures for many different brain functions, including those specific to cognition, visual, auditory, and sensory deficits. They also obtained data on social functioning, structural magnetic resonance imaging, family biomarkers and clinical information.
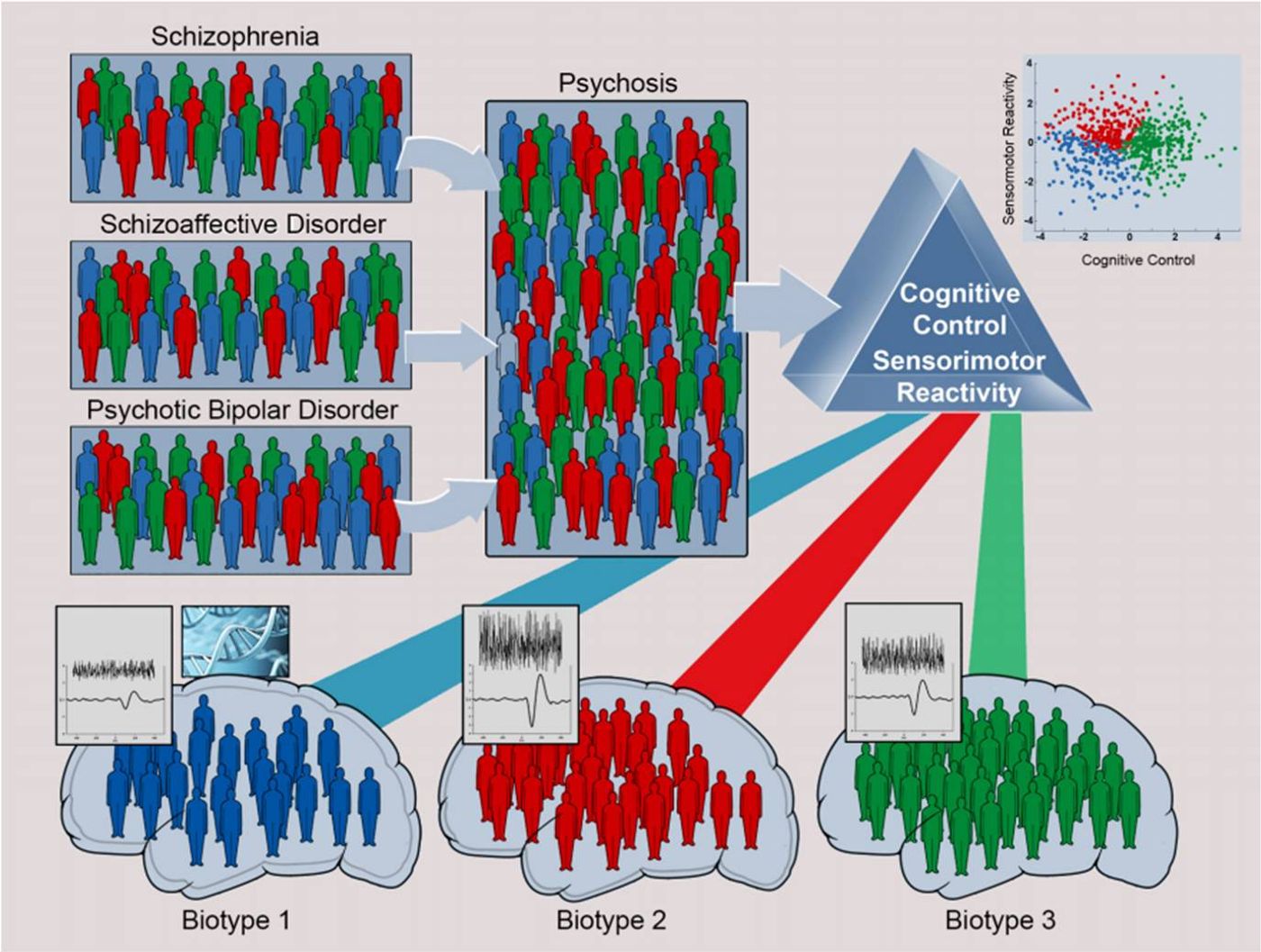
To see if the biomarker panels could delineate different psychiatric conditions, the researchers tested 711 patients with generalized psychosis, which is a defining characteristic of Schizophrenia, Schizoaffective Disorder, and Psychotic Bipolar Disorder. They then compared the data from patients with psychosis to data from over 1,000 first-degree relatives and healthy patients.
From their data analysis, the team identified 3 distinct “biotypes,” meaning 3 subgroups with different biomarker characteristics. Here are the 3 biotypes as summarized by the study results:
Biotype-1 cases were fewest in number, had low grey matter volume, significant neurobiological impairment, high numbers of clinically affected relatives, and poor psychosocial functioning.
Biotype-2 cases had high neural reactivity, modestly small grey matter volumes, and more modest but still significant cognitive impairment.
Biotype-3 cases were most numerous, had nearly normal cognition and neural reactivity, lowest numbers of clinically affected relatives, and the best psychosocial functioning.
The researchers reported their method of biotype classification was superior to the traditional DSM standards. "We were better able to predict who had family histories of psychoses, structural brain abnormalities and measures of social functioning when compared with DSM standards," Clementz said.
The results of this study challenge what used to be considered the gold standard of mental diagnosis. However, these biotype measures won’t be replacing the DSM soon, as more work needs to be done to evaluate its reliability across broader conditions. "We're a long way from identifying specific disease mechanisms, but we're a step closer than we were when we focused on clinical symptoms alone," said Clementz.
Watch the video to learn how clinical professionals react to the most recent update of the DSM.
Sources:
American Journal of Psychiatry,
Eurekalert