Cellular reprogramming has been a hot topic in translational and regenerative medicine ever since it was first described almost a decade ago. Recently, a team from the University of North Carolina (UNC) Chapel Hill
harnessed this potential, turning ordinary skin cells into predators that kill brain cancer cells. This innovation is hailed as a breakthrough in medical science, as it provides the potential of a new treatment option for an intractable form of brain cancer known as glioblastoma.
Glioblastoma (GBM) is the most common and deadly form of primary brain cancer. In GBM, malignant glial cells form vast networks of tendrils throughout the brain, making it nearly impossible to surgically remove all the cancerous tissues. Dubbed as the “octopus tumor,” GBMs can evade even the most aggressive surgeries, chemotherapies, and radiotherapies, leaving patients with a five-year survival rate of less than 10%.
"Patients desperately need a better standard of care," said Shawn Hingtgen, senior study author and assistant professor in the UNC Eshelman School of Pharmacy.
To combat hidden GBM tumor cells, the research team turned to neural stem cells (NSCs), which have an innate ability to move throughout the brain, accessing hard-to-reach solid and invasive cancer cells. But the limited supply of NSCs deep within the adult brain is not enough to fight GBM. So researchers at UNC decided to make more of these NSCs.
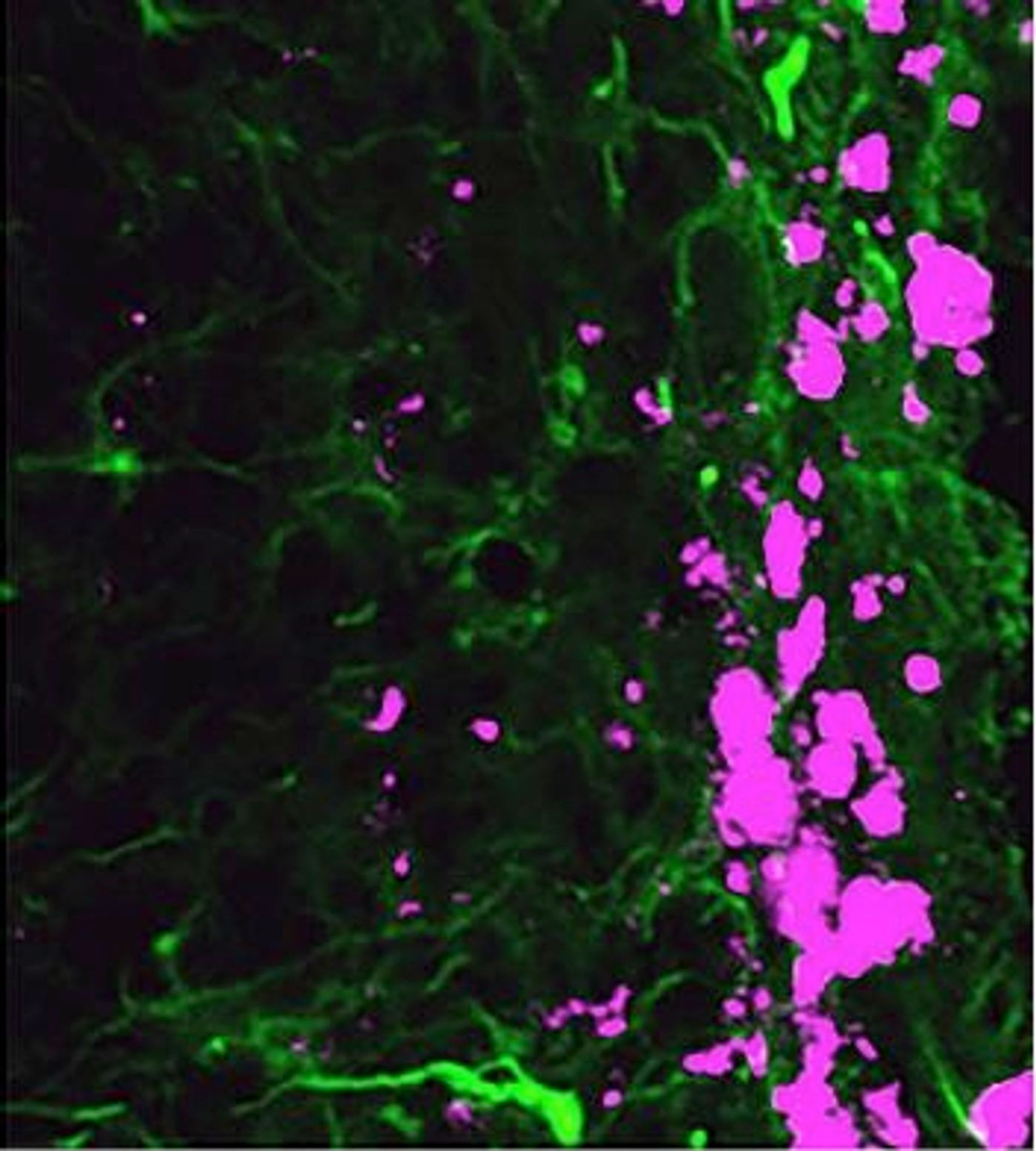
Starting with fibroblasts, which are ordinary skin cells that produce collagen and connective tissues, the researchers added reprogramming factors and coaxed these cells to become induced neural stem cells (iNSCs). When transplanted into mice, these iNSCs had the ability to move throughout the brain, along with the penchant for killing brain tumor cells. In mice with different tumor types, the iNSCs increased survival time by 160 to 220 percent.
The researchers are exploring genetic modifications that would enable the iNSCs to release toxic tumor-killing proteins. Additionally, the iNSCs can be adapted to carry anti-cancer drugs, which would then be ferried directly to the cancer cells, killing cancer at its home base. Both types of modifications would make the iNSCs an even more aggressive assassinator of cancer cells in the brain.
"Our work represents the newest evolution of the stem-cell technology that won the Nobel Prize in 2012," Hingtgen said. "We wanted to find out if these induced neural stem cells would home in on cancer cells and whether they could be used to deliver a therapeutic agent. This is the first time this direct reprogramming technology has been used to treat cancer."
Additional source:
EurekAlert!
 Cellular reprogramming has been a hot topic in translational and regenerative medicine ever since it was first described almost a decade ago. Recently, a team from the University of North Carolina (UNC) Chapel Hill
Cellular reprogramming has been a hot topic in translational and regenerative medicine ever since it was first described almost a decade ago. Recently, a team from the University of North Carolina (UNC) Chapel Hill