For couples who have trouble conceiving naturally, assisted reproductive techniques like in vitro fertilization (IVF) may be an effective treatment. But the expensive and invasive procedures have a low success rate, with live births occurring in only about one-third of the time. To improve the efficiencies of for assisted reproductive techniques, researchers at the Florida Atlantic University went back to the basics. That is, they asked how doctors can select the best fit sperm to fertilize the egg.

Infertility is more widespread than we imagine. Around the world, over 48 million couples experience fertility problems and can’t conceive after years of trying. In a large percentage of the cases, the problem is that sperm can’t reach the egg. This may be due to low sperm count, poor sperm motility, and other physical traits that make sperm unfit for the travel to the egg. Another reason for infertility related to sperm is that the sperm may carry too much DNA damage.
“DNA damage is one of the more important characteristics of sperm, because higher levels of damage are associated with lower pregnancy rates, early loss of pregnancy, and increased disease rates of offspring who are conceived through assisted reproductive technologies," said Waseem Asghar, assistant professor in the Department of Computer and Electrical Engineering and Computer Science at Florida Atlantic University. "That's why it is so important to develop methods to select the healthiest sperm for assisted reproductive technologies."
The current reproductive technology Asghar refers to involves centrifugation, or fast spinning, of the semen sample to select for the most motile sperm. In theory, this process should find the best fit sperm. However, the process can cause DNA damage in the sperm, which could thwart a healthy pregnancy. In addition, the process can’t discriminate sperm that’s too old and more likely to be unstable.
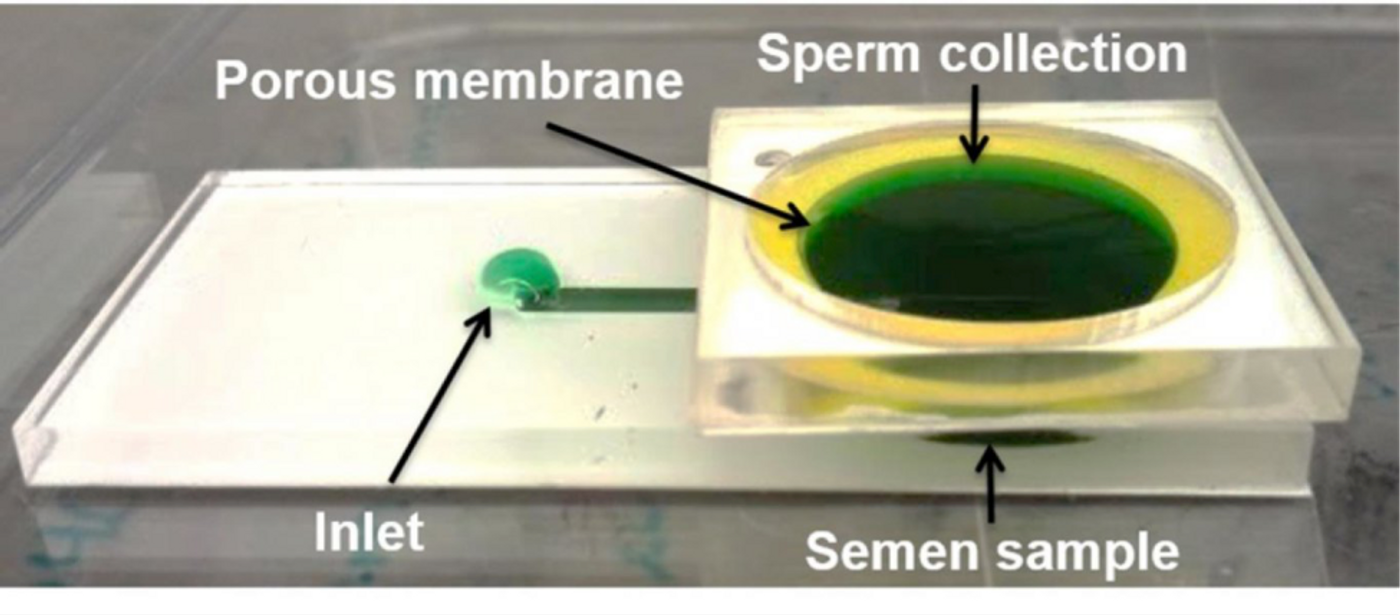
To circumvent these problems, Ashgar and his team utilized a
microfluidic system whereby healthy, motile sperm are separated from the weaker, non-functional sperm via a porous membrane sieve.
"Microfluidic based technologies have surfaced as a novel substitute to conventional methods that use centrifugation," said Asghar. "These are devices that use small volumes of fluid, can enable more control to precisely sort cells within small volumes, and are created to mimic what happens naturally in the female genital tract. Sperm sorting methodologies based on microfluidic procedures are a valuable option since these techniques eliminate the damaging centrifugation steps."
This technique is similar to the one conceptualized by a team at the University of Toronto, who observed that healthy sperm tend to slither from side to side. Furthermore, this slithering action increased sthe peed of the sperm by 50% in liquid conditions of higher viscosity, like that of the female reproductive tract. The case for speed is strengthened as previous work in microfluidics has shown that fast-moving sperm tended to have higher DNA integrity and are more likely to produce a viable embryo.
In addition to upping the chances of selecting a healthy sperm, Asghar’s sorting device doesn’t require any fancy machines. "Sperm separation techniques should be quick, easy, low-cost, and have the ability to select motile and morphologically normal sperm while decreasing damage done to sperm DNA," said Asghar. He estimates that a technician can collect the healthy sperm within 30 minutes.
Additional source:
Florida Atlantic University press release