For women at high risk for cervical cancer, Hopkins researchers say they have a
new diagnostic test that’s both non-invasive and more accurate than current tests on the market.
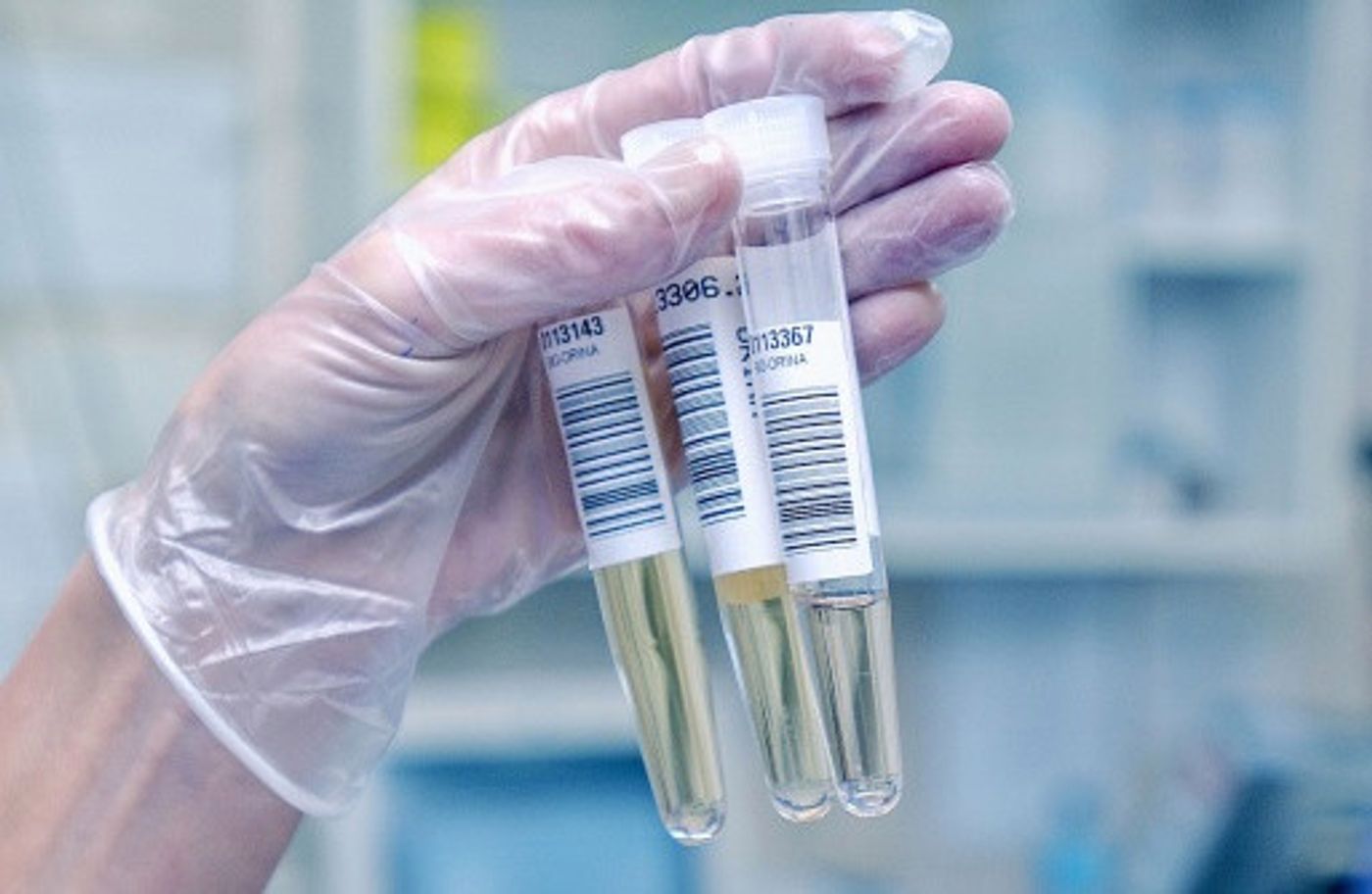
In profiling the genetic mutations that underlie cervical cancer, the research team identified a four-gene combination that can serve as biomarkers for the disease. Furthermore, they say the test can be done with urine samples, instead of using tissues collected from Pap tests.
Currently, routine Pap tests are recommended every 3 years for women between 21 and 65 years old. The test takes a swab of the cervical tissue to look for cancer cells. Women who have an abnormal Pap results and also test positive for the human papillomavirus (HPV) are then asked to undergo a biopsy to rule out cervical cancer. However, this method of screening is invasive, costly, and may not be necessary in at least 50 percent of cases.
Using hundreds of cervical cells collected, the Hopkins team built a diagnostic platform that consisted of a 4-gene panel. Three genes (FKBP6, INTS1 and ZNF516) were identified because they are highly associated with cervical cancer. The fourth gene (HPV16-L1) is an HPV gene that becomes methylated with cancer progression. With this four-gene panel, the team reported a sensitivity of 90.9 percent and a specificity of 60.9 percent.
"When developing a new cancer screening test, we want something in the range of 90 to 95 percent sensitivity, which is competitive with the effectiveness of tests developed and now marketed in Europe," said Rafael Guerrero-Preston, professor at the Johns Hopkins School of Medicine, and the study’s first author.
The new test is reported to surpass the sensitivity of two commercial tests, which have sensitivity of only 64 percent. In addition, because the tests rely on DNA methylation, Pap smears are required.
"If further studies confirm these findings, we see a significant use of urine screening as a way to quickly and inexpensively determine if a biopsy is warranted, or if physicians can use a 'watch and wait' approach before intervening," said Guerrero-Preston.
"Our urine test would serve as a molecular triage," he says, "at times supplementing Pap test information. In developing countries that don't have the money, medical infrastructure or cultural approval for Pap test, our test could be used instead."
Additional sources: Hopkins press release via
News Wise
 In profiling the genetic mutations that underlie cervical cancer, the research team identified a four-gene combination that can serve as biomarkers for the disease. Furthermore, they say the test can be done with urine samples, instead of using tissues collected from Pap tests.
In profiling the genetic mutations that underlie cervical cancer, the research team identified a four-gene combination that can serve as biomarkers for the disease. Furthermore, they say the test can be done with urine samples, instead of using tissues collected from Pap tests.