Effective Cervical Cancer Screening for Underserved Populations
New findings about cervical cancer could be great news for women all over the world, if the findings are heeded. It seems that only a small cell sample from women who are at high risk for developing cervical cancer would be an effective and low-cost way to make an important, early diagnosis in places considered to be low and middle income countries (LMICs). The work was led by Queen Mary University of London (QMUL) with funding from Cancer Research UK and it has been published in the Journal of Global Oncology. For women in the developing world, cervical cancer is the second most common cancer. Worldwide, it is responsible for the deaths of around a quarter of a million women every year, many of them occurring in LMICs.
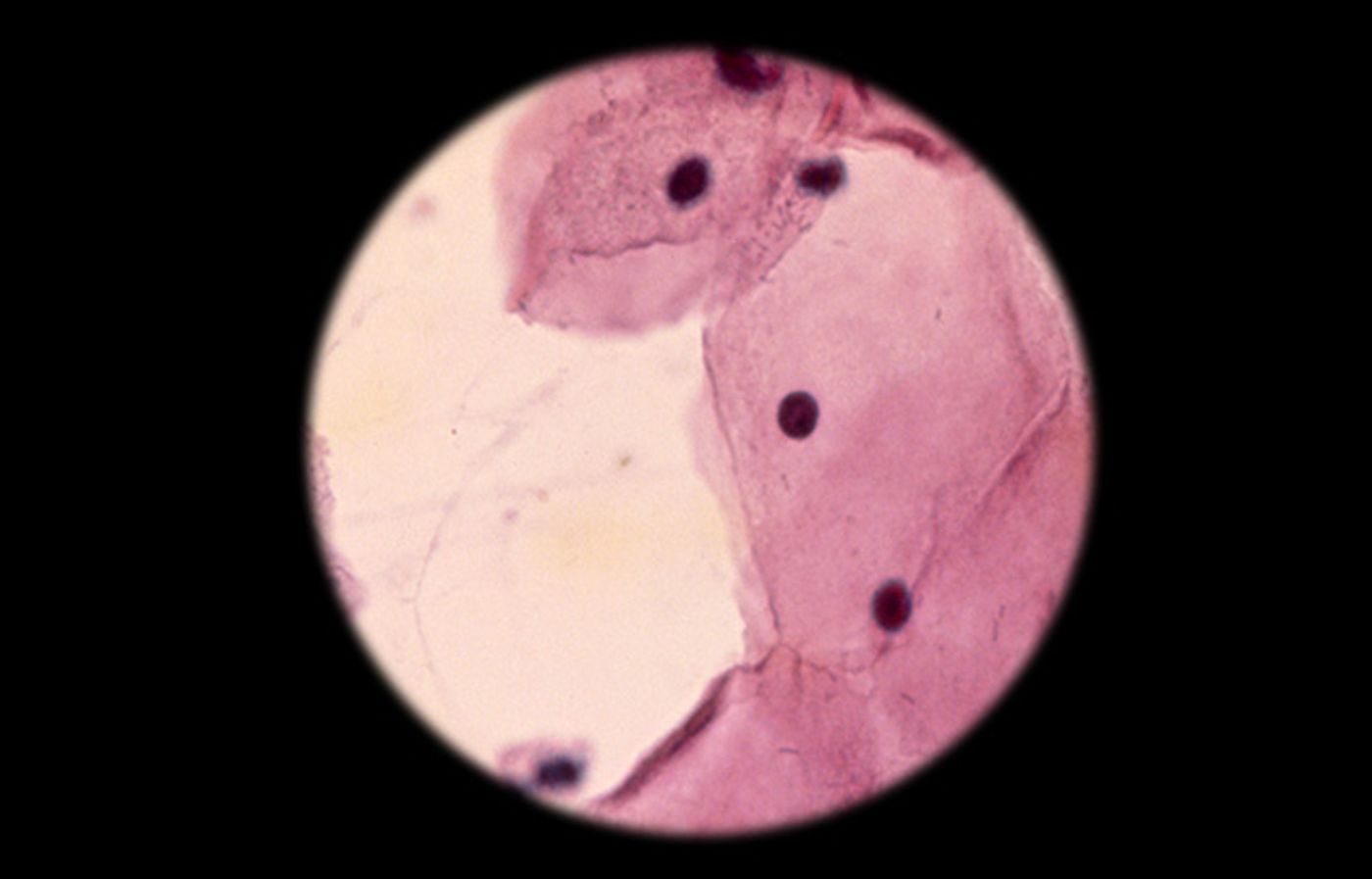
It's a typical part of routine health screens for women that have access to health care in developed countries. However, in countries without good health care infrastructure or resources like diagnostic laboratories, there has been a glaring lack of such screening methods. Those methods, cytological or cell based processes, are usually very effective at diagnosing the threat of cervical cancer before it fully progresses to cancer.
This is the first study that examines how effective cytology is at diagnosing cervical cancer in LMICs. The investigators examined cytology data from 23 studies in a variety of countries including fIndia, Bangladesh, China, Thailand, Kenya, South Africa, Uganda, Peru, El Salvador, Costa Rica, Nicaragua, Brazil, Argentina and Egypt, covering 717 cervical cancers. The researchers postulated that it's possible to make an earlier diagnosis of cervical cancer in these countries by employing cytology.
It was found that even in settings with limited access to resources, cytology is still very sensitive and consistent at diagnosing invasive cancer. Cytology successfully identified cancer with 95.9 percent accuracy in high-risk women that were showing symptoms.
"Cytology has long been established as an excellent screening tool to prevent cervical cancer by detecting precancerous lesions. However, little research has been carried out regarding its sensitivity to cancer," explained the corresponding author of the work, Dr. Alejandra Castanon of QMUL.
"We've found that this is an excellent tool for targeted screening of populations at high risk of cervical cancer, leading to early diagnosis. In resource-poor settings with limited facilities to treat advanced cancers, this could have a big impact on cervical cancer mortality."
Cytology could be used only on women with symptoms, and only sending those affected by severe lesions for additional treatment would result in far fewer women needing more investigation. There would subsequently be a reduction resource and cost burden, and may help catch cervical cancers at an earlier stage, thus improving the overall survival in those affected by the disease.
"The implications are that, even when a country lacks infrastructure to implement a quality-assured cervical screening program nationally, it might be able to facilitate early diagnosis of cervical cancer by using cervical cytology, and only referring women with severely abnormal smears," explained one co-author of the work, Professor Peter Sasieni from QMUL.
If you would like more information on how improved screening for cervical cancer could help underserved, check out the webinar above, "Cervical Cancer Screening of Vulnerable Populations," in this case about people in developed nations like the US.
Sources: AAAS/Eurekalert! via QMUL, Journal of Global Oncology