Algorithm Predicts Glioma Survival Better Than Specialists
For people newly diagnosed with glioma, a lethal brain cancer, the most they can hope for is an accurate diagnosis, so doctors can choose the best treatment plan, and a careful prognosis, so they can plan for their future. New technology from Emory University provides an option to produce both.
Glioma is characterized by any tumor that develops from the supportive tissue of the brain, called glia, which regulates neuron function. Symptoms and treatment depend on the exact type of glial cell that is affected by cancer, and the exact cause of glioma is unknown. Doctors do know that those diagnosed with glioma often die within two years of diagnosis, but some people survive for more than a decade. How can doctors distinguish between the two groups so glioma patients know how to plan for their future?
Existing options for glioma diagnosis and prognosis include genomic tests and microscopic examinations of tissue samples. However, genetic testing cannot predict a patient’s future on its own, and microscopic exams are open to interpretation by different doctors.
"Genomics have significantly improved how we diagnose and treat gliomas, but microscopic examination remains subjective,” explained lead scientist Daniel J. Brat, MD, PhD. “There are large opportunities for more systematic and clinically meaningful data extraction using computational approaches.”
The opportunity seized by Emory scientists focused on artificial intelligence (AI) software designed to predict which glioma patients will survive longer than a couple of years. The program is based on tissue biopsies. And so far, the software has been more accurate than predictions made by glioma specialists.
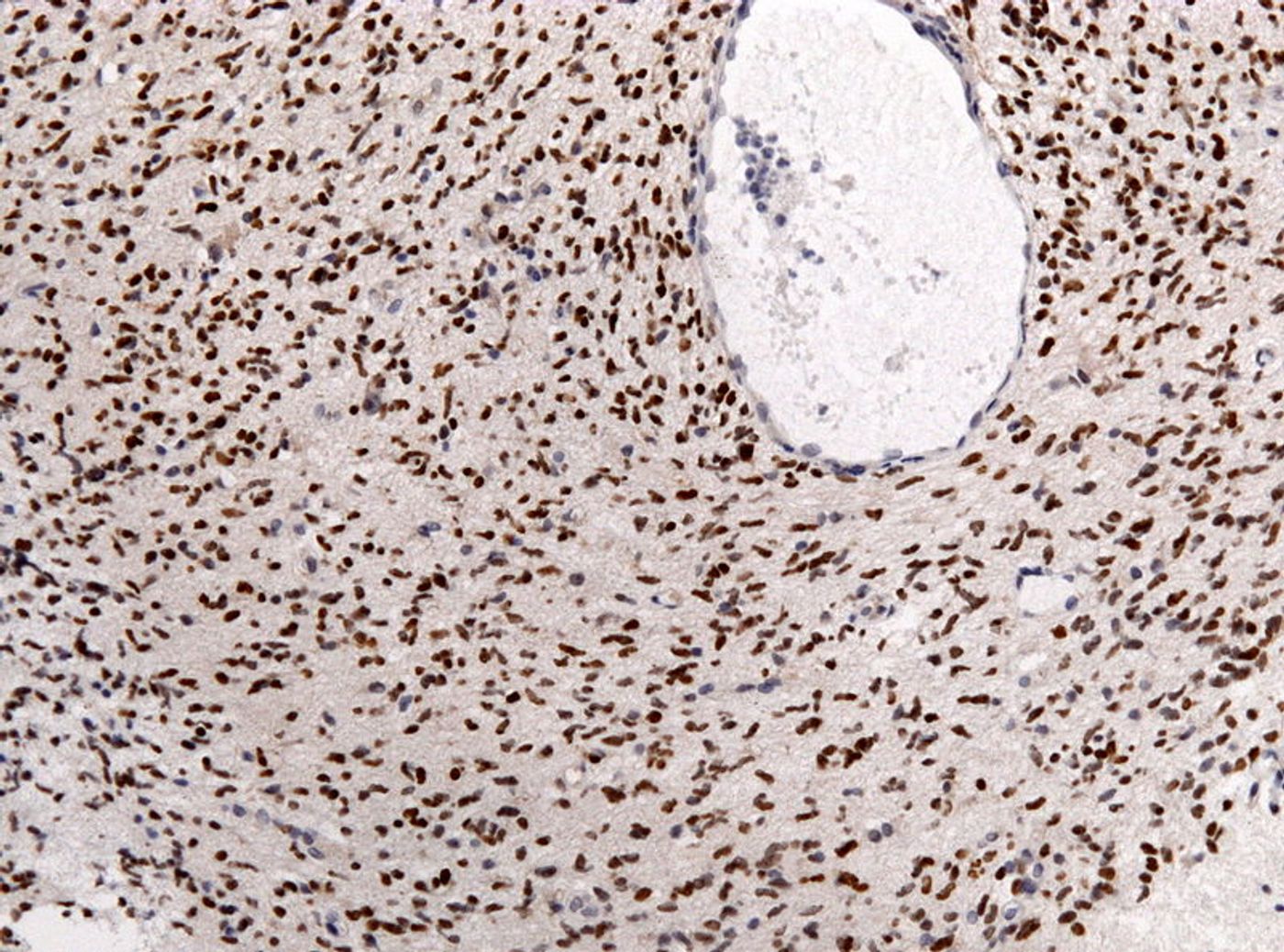
Microscopic images of brain tumor tissue samples and a process called “deep-learning” were used to program software to act as glioma specialists, looking for visual clues that indicate a patient’s odds of survival. Researchers primed the software with both images and genomic data.
After testing the software, its predictions of how long glioma patients survived following their diagnoses was more accurate than predictions made by human pathologists. Over time, the software “learns to recognize many of the same structures and patterns in the tissues that pathologists use when performing exams.”
Scientists want to see this program making predictions for doctors seeing glioma patients. This could greatly enhance decision making about treatments and future planning. Researchers are also looking for new opportunities to further test the program’s ability to improve outcomes for patients newly diagnosed with glioma.
"What the pathologists do with a microscope is amazing. That an algorithm can learn a complex skill like this was an unexpected result,” said lead author Lee A.D. Cooper, PhD. “This is more evidence that AI will have a profound impact in medicine, and we may experience this sooner than expected."
The present study was published in the journal Proceedings of the National Academy of Sciences.
Sources: American Brain Tumor Association, Emory Health Sciences