Personalized Medicine for Cystic Fibrosis
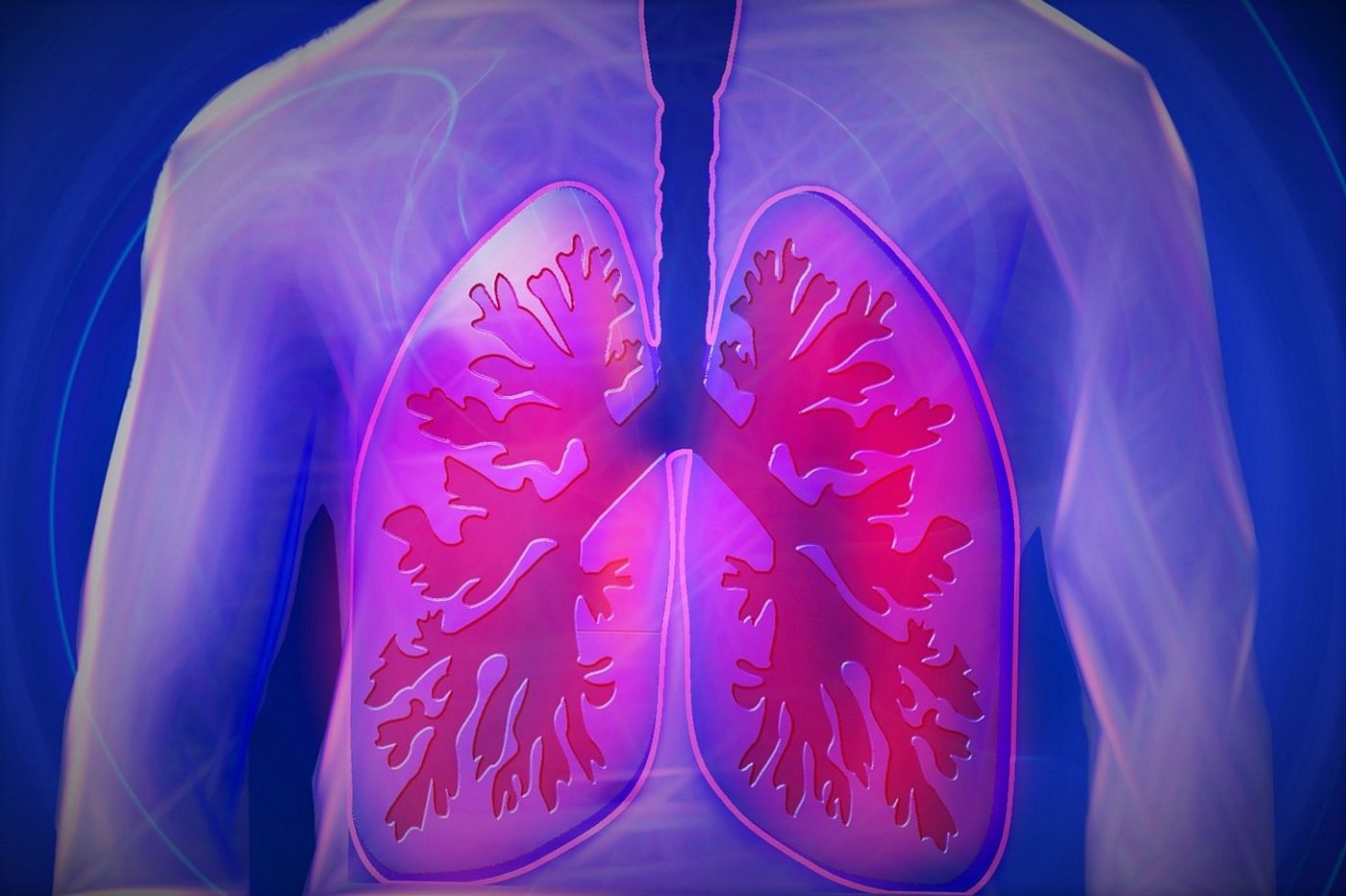
Cystic fibrosis is a disease which is best known for effecting the lungs, but can also impact other organs such as intestines, liver, kidneys, and pancreas. In the lungs, this is a debilitating disease that causes congestion, difficulty breathy, and increased risk for lung infections. Cystic fibrosis is a genetic disease caused by bi-allelic mutation of the cystic fibrosis transmembrane conductance regulator, or CFTR, protein which has known roles in the production of fluids such as mucus, sweat, and those of the digestive tract. When CFTR protein is mutated, these fluids are secreted in a much thicker form than usual. To date, there is no known cure for cystic fibrosis and life expectancy for those harboring this disease ranges from 42-50 years old.
Recently, strides toward effective treatments for cystic fibrosis have been made, but not every treatment works in every patient, so there has been a push towards personalized medicine. In the most recent November issue of the Journal of Clinical Investigation, researchers from the University of North Carolina at Chapel Hill published a study utilizing a test to predict which potential treatment option is optimal for each patient based on their individual profile, demonstrating that this type of approach is worthwhile.
Cystic fibrosis presents a challenge for drug targeting as it is a result of thousands of genetic alterations in addition to CTFR, and the mutations specific to each patient will effect how they respond to different therapeutic modalities. Jennifer Guimbellot, MD of the University of Alabama in Birmingham, previously of the University of North Carolina at Chapel Hill, stated “Any given drug may not be the drug that works best for a given patient, because there’s so much variation from person to person. We still have a long way to go to get a really optimized therapy for most cystic fibrosis patients, and the only way we can do that is to have a model like ours where we can take cells from each individual patient and test them with each individual drug to find out which one is the best match.”
This holds a lot of promise, but the execution of such an idea is less straight forwards. Currently therapeutic options treat the symptoms of cystic fibrosis, but what we really are drugs to treat the disease itself and potentially “cure” it. To test all of the candidate therapeutics is seemingly impossible to do – multiple drugs on one single patient to determine which has best efficacy in itself isn’t viable, in addition to the time, material, and costs involved. So Dr. Guimbellot came up with another way to test the same concept in collaboration with Martin Gentzsch, PhD at the University of North Carolina. This method is to utilize nasospheroids which are fluid filled balls of nasal cells taken directly from the patient in question and grown in laboratory culture, and test potential drug candidates to see which will work, and then use the identified drugs to treat the patient.
This provides a non-invasive, inexpensive, quick screening platform to provide highly individualized treatment and care to cystic fibrosis patients. The authors indicate that their initial studies demonstrate that this proof of concept works, but more testing will still be needed prior to translating this into the clinic. At any rate, this is promising and exciting news in the field of cystic fibrosis research and treatment.
Sources: Journal of Clinical Investigation, UNC Healthcare News, Wikipedia, Pixabay, Pulmozyme, 3DSteve, Youtube
-
MAY 07, 2024Is It Anti-RNP or Anti-Sm/RNP?
-
MAY 08, 2024Expand your Multiomic Capabilities with RNAscope™
- See More
-
APR 30, 2024Immuno-Oncology Virtual Event Series 2024
-
MAY 07, 20243rd International Biosecurity Virtual Symposium
-
MAY 23, 2024For the Love of Digital PCR 2024
- See More