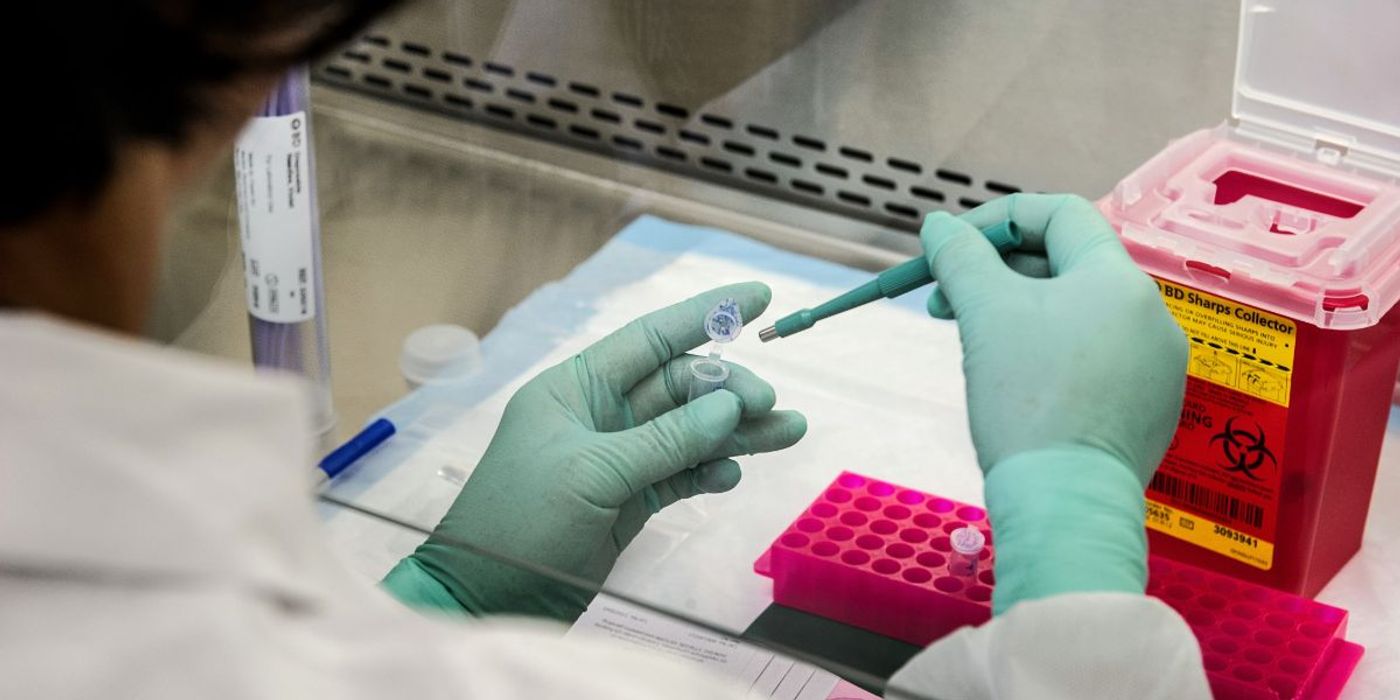
Can We Cure Down's Syndrome with Gene Therapy?
Down’s Syndrome (DS) is a genetic disorder brought on by the presence of all of part of a third copy of chromosome 21. Linked to delays in physical growth, mild to moderate intellectual impairment and distinctive facial features, there is currently no cure for the disease. Given all the hype around new findings in gene therapy however, could this emerging technology hold a possible cure?
There are two ways in which gene therapy could tackle DS: somatically ie. making changes to an individual’s genome that can not be inherited, or via the germline ie. making changes to the genome of very early embryos that may then be inherited.
Somatic avenues for treating DS with gene therapy may be able resolve elements of the condition such as the loss of nerve cells leading to weak musculature. However, difficulties arise both in defining the precise genes responsible for DS characteristics, and then being able to target them both safely and efficiently within the billions of relevant live cells in a patient at a sufficient rate to treat the condition.
Researchers from the University of Massachusetts Medical School for example faced this challenge when devising a gene therapy treatment. In a study from 2014, they were able to “turn off” the extra chromosome 21 responsable for DS by adding an RNA gene known as X-inactive specific transcript (XIST) to human stem cells. By inserting the XIST gene onto the extra chromosome in cells taken from those with Down’s syndrome, they were able to ignite a buildup of RNA that eventually coated the extra chromosome and shut it down. To be effective in eliminating DS however, this procedure would have to be replicated across most, if not all cells in an organism- a mammoth task beyond current possibilities.
This thus makes germline treatments, in which fewer cells may be treated at once, more attractive. Although in theory this method could be applied on a germline basis to embryos, as it is not possible to predict in advance which embryos will have trisomy 21, such options are also limited. Moreover, even though it is possible to screen for the condition using preimplantation genetic testing (via in vitro fertilization (IVF)), as IVF yields multiple embryos to choose from, it would be preferable to simply select an embryo that is already trisomy 21-free for implantation, and thus gestation, rather than go through the effort and risk to genetically engineer out an extra chromosome 21.
Another example of a gene therapy treatment for DS came in 2017, when Chinese scientists successfully managed to use CRISPR/Cas-9 technology to edit and/ or eliminate sex chromosomes and autosomes in culture cells, embryos and in vivo tissues. Although able to eliminate human chromosome 21 in human stem cells with trisomy 21 (an extra chromosome 21) via CRISPR, they were unable to do so in a embryos. This led them to surmise that single-autosomal deletion leads to embryonic lethality, and thus suggest the usage of CRISPR/Cas9 editing to limit chromosome functionality, rather than delete it. But once again, how such an intervention would be delivered among cells remains an issue.
To conclude, although advances are certainly being made in gene therapy to be able to combat genetic disorders such as DS, major hurdles remain to be overcome before an effective treatment option is available. In particular, how to edit or eliminate the extra chromosome in enough cells to yield significant results remains a sizable challenge, alongside how to be able to intervene at a stage early-enough that this needn’t be an issue.
Sources: Genome Biology, BioNews, Futurism, Biomedical Central and NPR