Will Genetic Sequencing Become a Routine Part of Health Care?
While the information obtained from genetic testing is not useful for many healthcare decisions that patients and their doctors make today, it is likely to become a much bigger factor in the future. The more we reveal about the human genome, the more clinicians and patients will be able to make more tailored choices about health issues that may arise. The Geisinger Institute wants to improve healthcare, and they are trying to do it for as many people as possible with a new project.
As we reveal more about the genome, many new possibilities arise in preventive health care and patient-specific treatments. This issue will become more relevant to everyday medicine in the near future, as patients and doctors become more equipped to make choices about healthcare. One major concern is that not everyone will be able to benefit from these new possibilities and the better health they may afford. The Geisinger Institute is aiming to confront these issues.
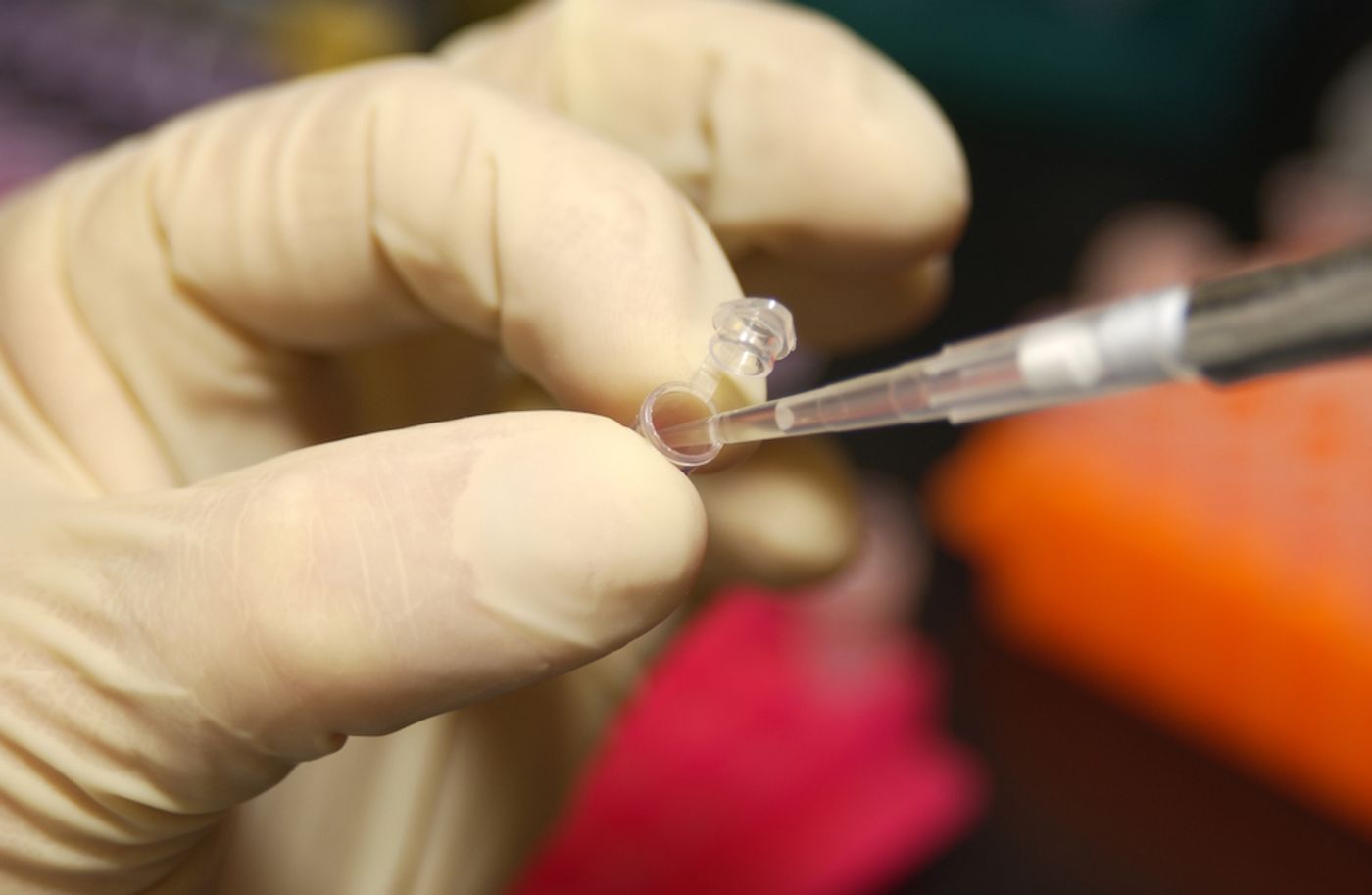
The Danville, Pennsylvania-based Geisinger Health System has developed and run what is known as the MyCode Community Health Initiative. The project sequenced the exomes, or protein-coding regions of DNA, of over 92,400 people so far. More than 166,000 people have enrolled in the study; the ultimate goal is to recruit half a million patients from the 3.3 million that use Geisinger services. About 85% of the participants have also agreed to participate in the experimental program in which they receive their information, called GenomeFIRST Return of Results.
Geisinger wants, of course, to use the genetic data to prevent and treat disease, but they want to examine other questions as well. They are interested in how primary care physicians that may have very little knowledge of genetics are able to advise patients who have learned of disease-causing genetic mutations, and how the new information impacts family members who find out they might be at risk. This research will help doctors decide what is appropriate to reveal to people about their genomes. "This is the future of health care," commented Michael Snyder, the Director of Stanford Medicine's Center for Genomics and Personalized Medicine in Palo Alto, California. "Incorporating a person's genome sequence information into disease risk assessment is a no-brainer,” he told Science.
Patients find out if they carry a mutation in any of 76 genes, all of which have been conclusively linked to 27 disorders, like heart disease or breast cancer. The conditions are all treatable, said the Head of Clinical Genomics at Geisinger, Michael Murray. If a variant does not have an established, accepted treatment, the patient is not notified. It’s estimated that 3.5 percent of participants will learn they have a variant associated with disease. Their primary care physician is told first, and the physician gets more information about the variant and how to explain it to the patient.
Some scientists have expressed concern that not enough information is disclosed. Other commend the restraint, because there are many variants we simply do not yet know enough about in order to tell people what it will really mean for their health.