Advances in Cancer Research Through Organoids
Researchers have been using a new tool in biomedical research to more closely mimic human biology. Instead of animal models, scientists have found a way to grow cells in culture that form simple, 3D versions of human organs, like the brain. These so-called organoids have offered an incredible opportunity to study tumor growth or assess drug efficacy. Now, scientists have combined organoids with an investigation of one of the deadliest brain cancers, glioblastoma multiforme (GBM). They tweaked two genes used when creating cerebral organoids in the lab, generating severe GBM tumors. The model, by the Verma lab at the Salk Institute, offers an unprecedented opportunity to earn more about the development and treatment of GBM.
Scientists used to harvest patient tumor tissue and apply it to animal models, a xenograft, to learn more about disease development. There are problems with this technique, however. "As tumors grow in mice, the environment changes the tumor's features," explained Junko Ogawa, a Salk senior research associate. "We don't know if it's similar to the patient's original cancer." Ogawa is the first author of a paper in Cell Reports about this work.
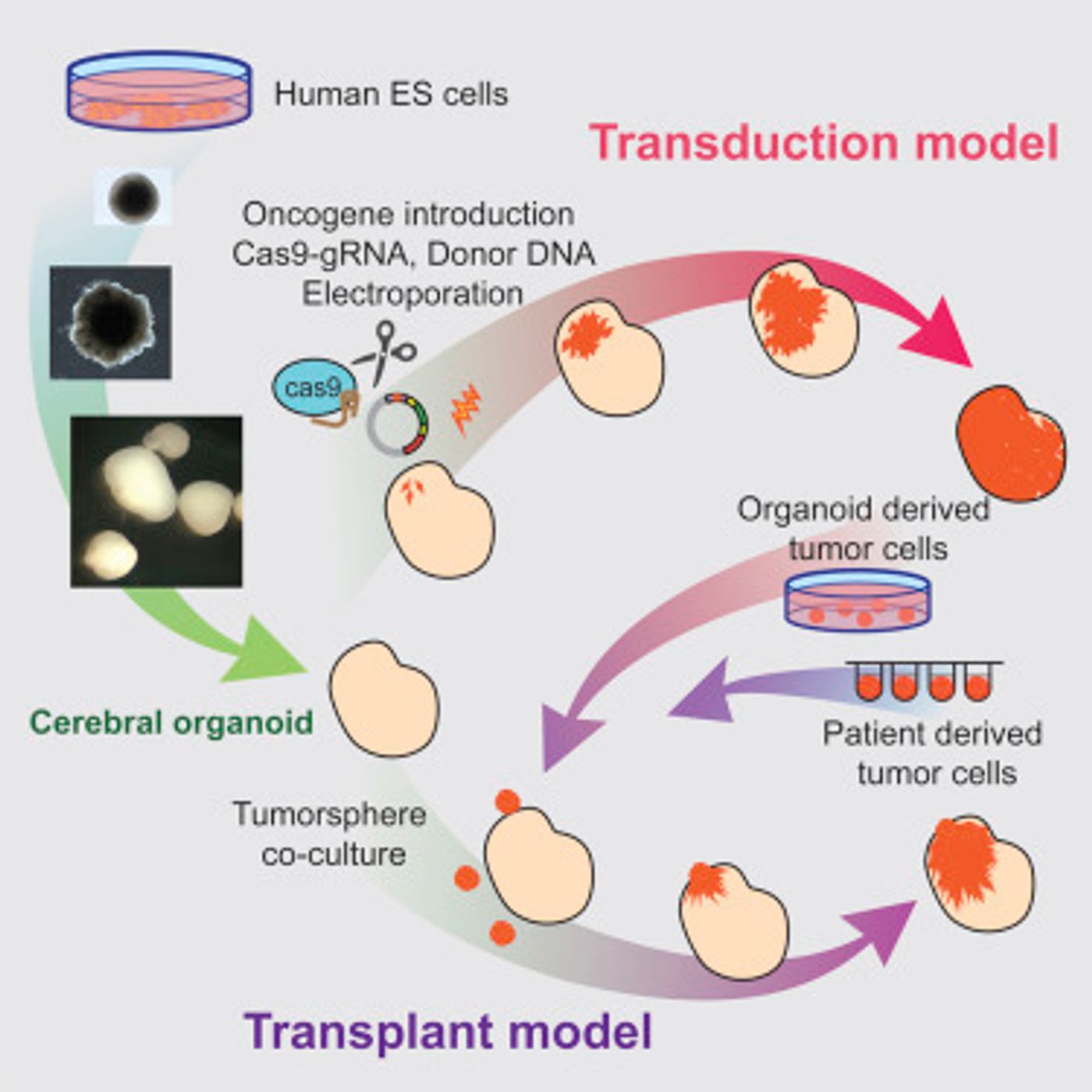
CRISPR/Cas9 is a gene-editing technique that was utilized by the scientists to alter two genes linked to cancer, p53 and HRas. While HRas drives cell growth, p53 suppresses tumors; by manipulating both, the researchers changed their organoids dramatically. Growth was promoted, and the brakes on that growth were removed.
These organoids, which are about four millimeters and grow in a dish as 3D structures, became like tumors after the gene edits. Several biomarkers associated with GBM were found in the organoids. The scientists could also transplant them into animals, where they grew aggressively.
The scientists note that by generating the GBMs this way, it more faithfully replicates the human condition; instead of a xenograft of a tumor, the cancer growth starts off as a handful of aberrant cells, as it would naturally.
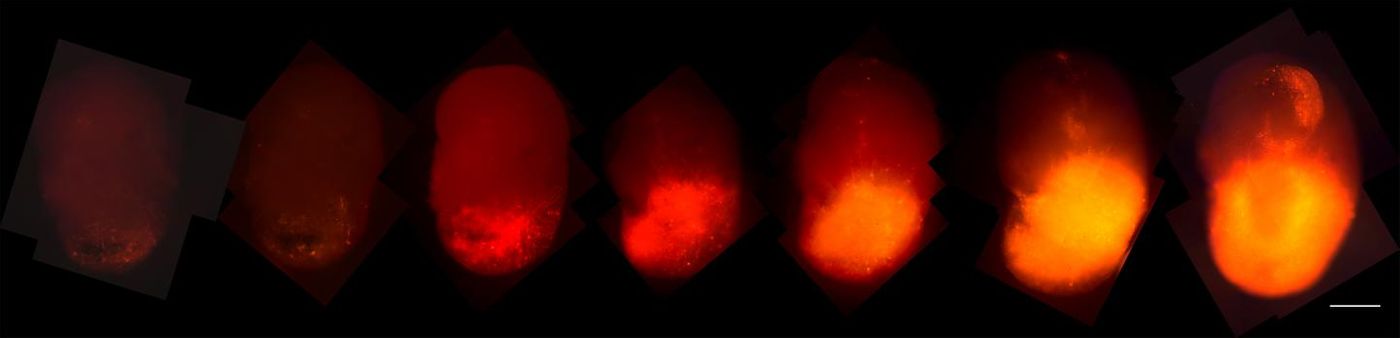
The scientists also put a fluorescent tag, tdTomato, onto the cancer-causing HRas. That allowed the researchers to observe the progression of cells that contained the modified gene as they took the organoid over. After transplantation into animals, they resembled patient tumors more closely and also offered a repository of tumor tissue.
"You can phenocopy the properties of the tumors in a mouse," said Ogawa, "and now we can give them drugs to see if they are effective. We can also test the tumor's ability to invade normal brain tissue."
It may be possible to personalize the treatment of GBM in patients by using organoids that boost samples from patients. The organoids do lack the complexity of human physiology but clearly offer advantages over animals. It may be possible to apply this strategy to other cancers.
Learn more about how organoids are helping advance our understanding of brain cancer from the video above by the Cure Brain Cancer Foundation.
Sources: AAAS/Eurekalert! Via Salk Institute, Cell Reports