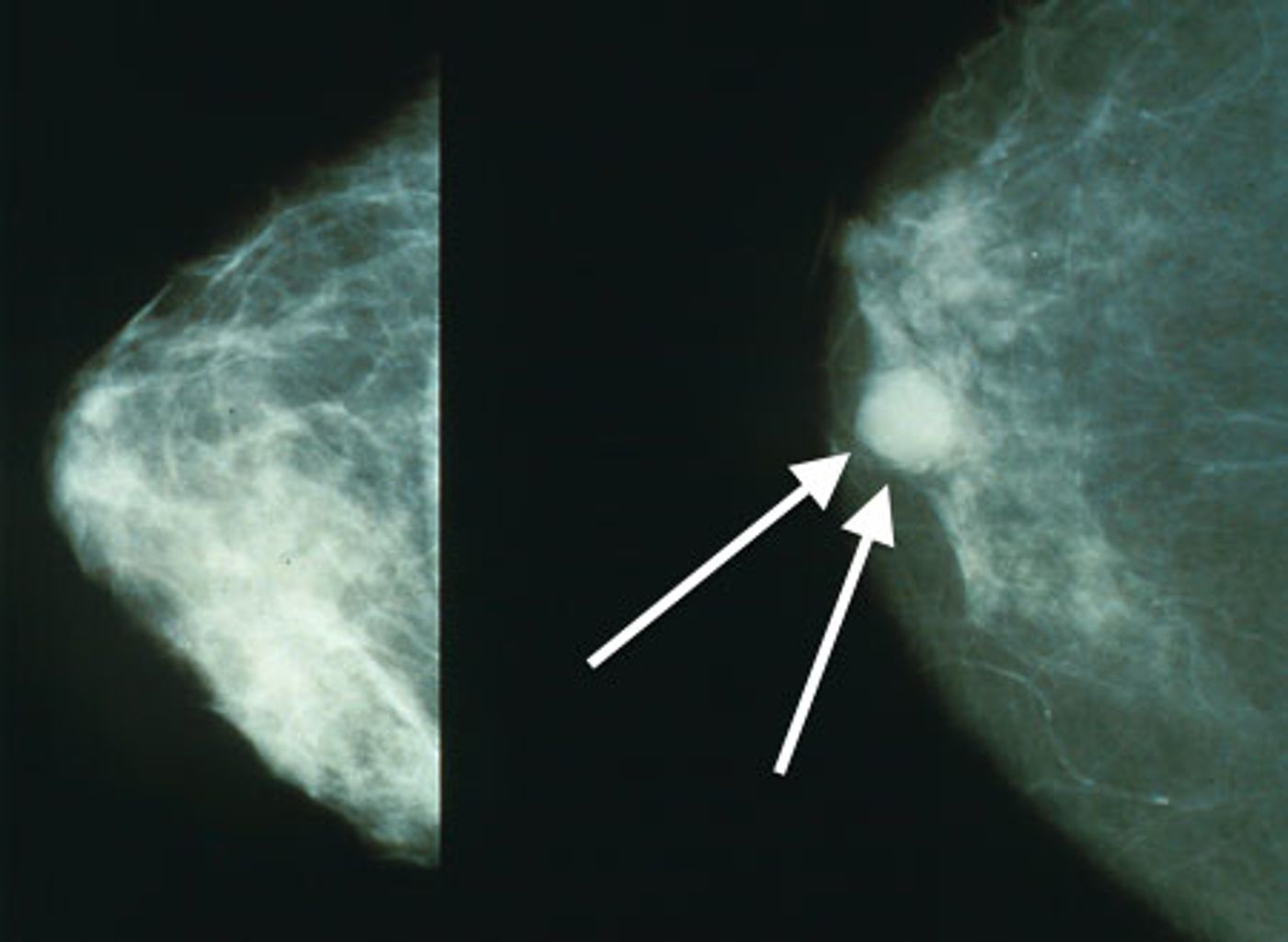
In the United States, about 67 percent of women 40 and older get a screening mammogram every one to two years. If the radiologist sees something on the image that looks abnormal, he or she will recommend the patient get additional imaging, epidemiologist Louise M. Henderson explained to LabRoots. They will focus in on the area and do magnification views. Based on that, the doctor will decide whether they believe the patient has cancer or not. They may ask the patient to get additional tests, like an ultrasound. Usually, if the image is still unclear, they will do a biopsy. Then the patient will know whether they have cancer or not.
Over a course of 10 mammograms, women who get screened yearly have a 61 percent chance of receiving at least one false-positive result. Women who get mammograms every two years have a 42 percent chance of receiving at least one false-positive result.
Now, research shows that women who have received a false-positive mammogram in the past may be at increased risk of developing breast cancer for up to 10 years after the false-positive result.
A group of researchers, led by Henderson, wanted to know more about the risk of breast cancer among women who have received a false-positive result. They questioned whether there would be a greater risk among women who were referred to get a biopsy compared to women who were referred to just get additional imaging. The researchers also wanted to know whether the results would be independent of breast density.
Henderson and her research team analyzed data from 1994 to 2009 from the Breast Cancer Surveillance Consortium. The data came from seven different registries in different parts of the United States. It included 2.2 million screening mammograms performed on 1.3 million 40 to 74-year-old women. The women were tracked over the course of 10 years after the initial screening. This allowed the researchers to evaluate the women’s breast cancer risk over time.
Henderson and her team found that, after receiving a false-positive, women who were just referred to additional imaging had a 39 percent higher risk of developing breast cancer during the 10 year follow-up period compared with women with a true-negative result. Women who had false-positive results and were ultimately recommended for a biopsy had a 76 percent increased risk of developing breast cancer.
Different breast density revealed similar results for women. However, “among women with almost entirely fatty breasts, both the [biopsy and imaging] false-positive groups had about a 70 percent higher [risk] compared to women with a true-negative mammogram result,” Henderson said in a press release. It didn’t matter whether they were asked to get a biopsy or just imaging.
The results suggest that suspicious findings on mammograms mark a higher cancer risk in the future. "Given that the initial result is a false-positive, it is possible that the abnormal pattern, while noncancerous, is a radiographic marker associated with subsequent cancer,” Henderson said.
"We don't want women to read this and feel worried," Henderson said. "We intend for our findings to be a useful tool in the context of other risk factors" such as age, race, and family history of breast cancer. The study is a step forward in identifying additional risk factors and is useful when thinking about things like risk prediction models.
The study was published December 2 in the journal
Cancer Epidemiology, Biomarkers & Prevention.
Source:
Press release via
EurekAlert!, direct contact with author, journal paper via media contact at
American Association for Cancer Research