Atopic Dermatitis: A Harbinger of Autoimmune Diseases?

Results come from a systematic review and meta-analysis consisting of 14 observational studies, pooling odd ratios (OR) using a random effects model. Patients with atopic dermatitis were found to have a higher prevalence of the following autoimmune diseases: alopecia areata (OR of 9.72), celiac disease (OR of 1.98), Crohn's disease (OR of 1.66), rheumatoid arthritis (OR of 1.18), systemic lupus erythematosus (OR of 1.74), ulcerative colitis (OR of 1.95), and vitiligo (OR of 4.52).
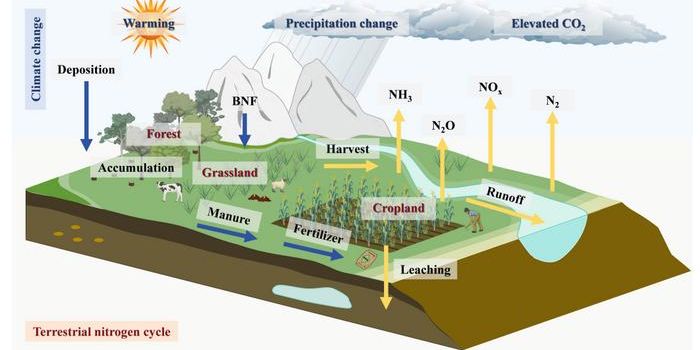
Atopic dermatitis, the most common chronic inflammatory skin disease, is estimated to affect at least 230 million people across the globe. Symptoms usually start early in life and include the formation itchy lesions. Suspected causes include reduced epidermal barrier function, dysregulation of the immune system, and/or altered microbiome.
In some cases of atopic dermatitis, reduced epidermal barrier function was traced back to reductions in or the complete absence of the protein filaggrin required for normal epidermal structure. This change in structure leads to increased transepidermal water loss in patients with atopic dermatitis. These disruptions in skin barrier function have been found to cause a strong Th2 inflammatory response, a process of the adaptive immune system. Th2 responses drive antibody and eosinophil production. The connection between atopic dermatitis and autoimmunity could be related to similar changes in adaptive immune function.
Genetic variants associated with atopic dermatitis may also be associated with specific autoimmune diseases. Researchers in this study noted that in a recent meta-analysis of genome-wide association studies, 10 new susceptibility loci for atopic dermatitis overlapped with those associated with multiple autoimmune diseases.
Reported study limitations included small sample sizes for some of the studies included in the meta-analysis, inconsistency between the studies in terms of which confounding factors they controlled for, and the use of subjective questionnaires in some studies to assess atopic dermatitis and autoimmune disorders.