How Bacteria Enter the Brain to Cause Meningitis
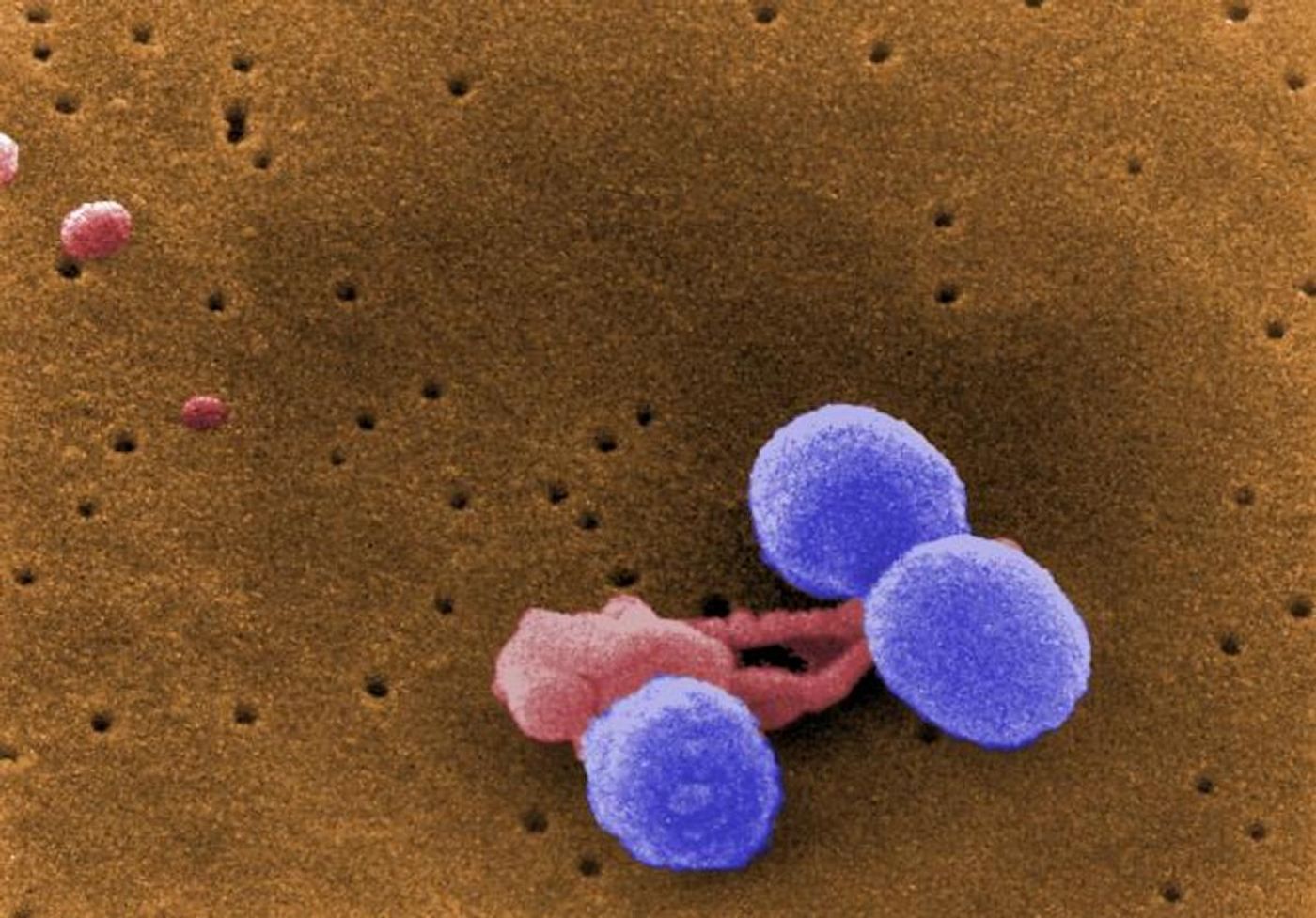
Infections with many different types of bacteria including Streptococcus pneumonia, Listeria monocytogens, and Neisseria mengitidis can cause bacterial meningitis. It's estimated that every year over 1.2 million cases of bacterial meningitis happen around the world, and without treatment, this deadly disease is fatal to seven of ten people who are sickened by it. Even with antibiotic treatments, three of ten patients die. Survivors are left with issues like chronic headaches, seizures, loss of vision or hearing, and other neurological consequences. New research reported in Nature has revealed how bacteria are able to penetrate the meninges that surround and protect the brain to cause bacterial meningitis. The findings have shown that bacteria use neurons to evade immunity and infect the brain, and the work may aid in the creation of new therapeutics.
Right now, antibiotics can help eliminate the bacterial pathogens that cause this illness. But steroids are also needed to control the dangerous inflammation that can occur along with the infection. However, reducing inflammation also weakens the immune response, making it harder to get rid of the infection.
In this research, the scientists used Streptococcus pneumoniae and Streptococcus agalactiae bacteria, which can both cause bacterial meningitis in humans. They determined that when these bacteria get to the meninges, they release a toxin, which activates neurons in the meninges that sense pain. This pain neuron activation could explain why bacterial meningitis patients get horrible headaches, noted the researchers.
The activated pain neurons then release a signaling molecule called CGRP, which binds to a receptor called RAMP1 on the surface of immune cells called macrophages. Once CGRP binds to RAMP1 on macrophages, the immune cells are basically disabled, and they stop responding to bacterial infections like they normally would.
The link between CGRP and RAMP1 on macrophages also stops them from signaling to other immune cells, which allows the bacterial infection to not only penetrate the meninges but to spread infection.
This work was confirmed with the use of a mouse model that lacked the pain neurons that are activated by bacteria. Compared to mice with those neurons, the engineered mice had less severe brain infections when they were exposed to bacteria that cause meningitis. There were also lower levels of CGRP in the engineered mice compared to normal mice. The normal mice, however, had higher levels of bacteria in the meninges.
Additional experiments also showed that when mice were treated with drugs that block RAMP1, the severity of the bacterial infection was reduced. Mice treated with RAMP1 blockers were able to clear their infections faster too.
It may be possible to help the immune system clear cases of bacterial meningitis with medications that block either CGRP or RAMP1, potentially in conjunction with antibiotics. There are already drugs that can do this, and they are generally used to treat migraine.
Sources: Harvard Medical School, Nature