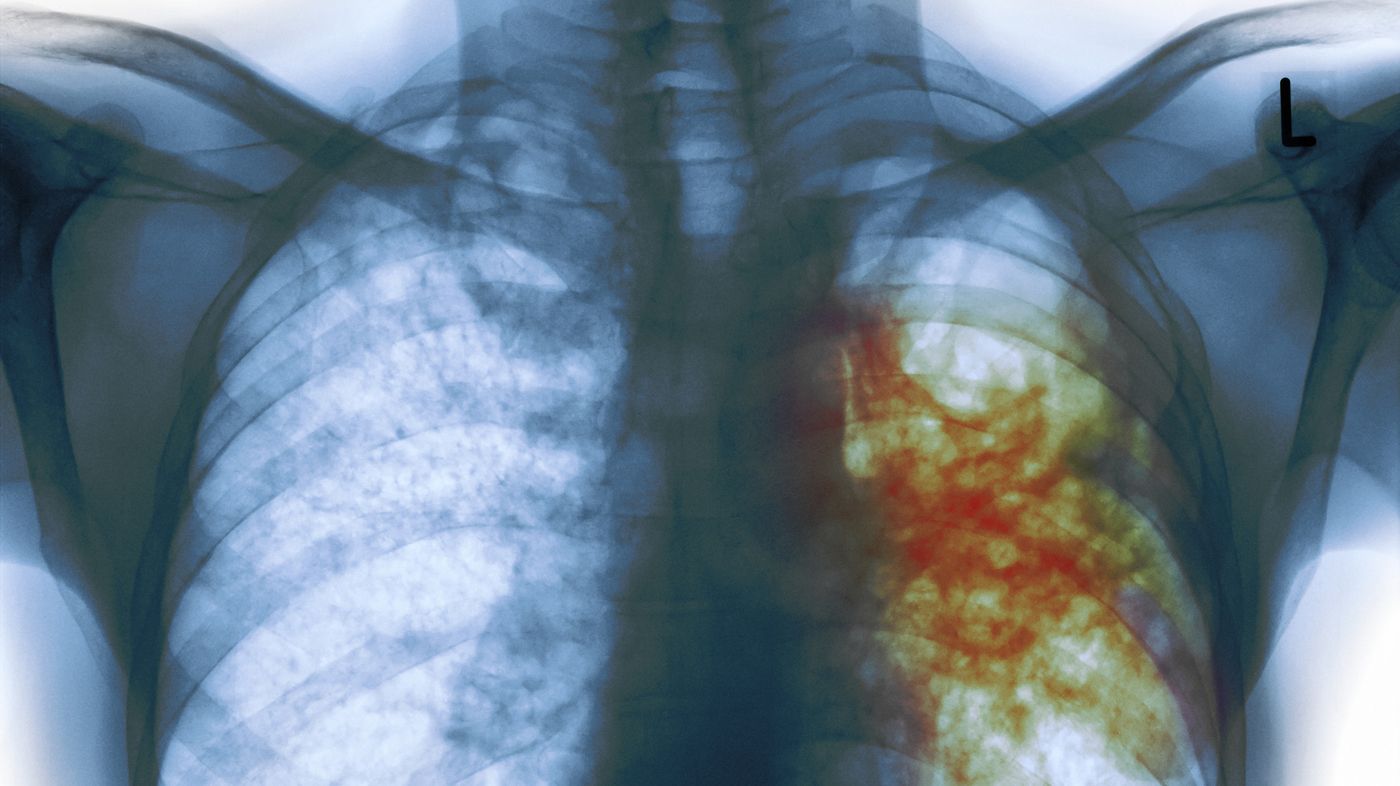
Mycobacterium tuberculosis, the bacterial species behind tuberculosis infections, is the leading cause of bacterial death globally. This microbe got to the top by outsmarting macrophages, key phagocytic cells of the immune system.
A new study in
Nature Immunology conducted by New York University scientists exposes that unique ability of
Mycobacteria to evade destruction by the immune system, even after being captured by a macrophage.
Mycobacteria manipulate macrophages to make certain cuts in their bacterial DNA so they can express more microRNA-33, a small RNA that promotes bacterial survival by inhibiting macrophage ability to “package” bacteria for degradation. Normally, macrophages recruit phagosomes to envelop foreign particles and lysosomes to break them up into pieces. By avoiding this process,
Mycobacteria can then exist freely in the cell’s cytosol.
Macrophages also incorporate a back-up process for removing foreign objects, called autophagy. This process also controls lipid levels and recycles old cell parts, and
Mycobacteria have a way around autophagy too. The researchers found that bacterial proteins activating an immune signaling pathway that prompts a protein complex called NFKappaB to produce even more microRNA-33, which in turn disrupts autophagy so lipid levels are left uncontrolled.
Disrupting both the phagolysosome and autophagy means that tuberculosis bacteria are evading two key protective processes, a factor that is “central to the infection’s deadliness,” said senior study author Kathryn Moore, PhD.
While the NYU study was done in mice, similar patterns are also seen in humans. Because of these parallels between species during tuberculosis infections, scientists are hopeful that they can develop a new drug to fight tuberculosis, possibly revolving around reversing lipid buildup in macrophages as
Mycobacteria evade autophagy.
Their first idea was to usestatins as a treatment because they inhibit cholesterol synthesis. Although this would effectively treat lipid buildup in macrophages, it would also be helping tuberculosis bacteria become even more virulent. NYU researchers recognized an interesting connection between statin drugs microRNA-33. The small RNA that tuberculosis bacteria rely on to be infectious is encoded in the same gene that statins target; cholesterol reduction and microRNA-33 production go hand in hand.
The researchers are not without hope, though. The next potential comes from antisense oligonucleotides, which could possibly be used to remove microRNA-33, cutting tuberculosis bacteria off from their evasive maneuvers.
Source:
New York University