Making the decision to move from co-testing to primary Human papillomavirus (HPV) screening was one thing. Implementing it has been another, for one medical group.
The University of Louisville Physicians-Family and Geriatric Medicine (UofL), Louisville, Ky, had contracted with one of the largest providers of diagnostic testing services in the United States in the past. They were forced to find a different lab when they decided to implement primary HPV screening alone for all women 25 years and older, and continue to screen with primary cytology and HPV triage for those 21 to 24 years.
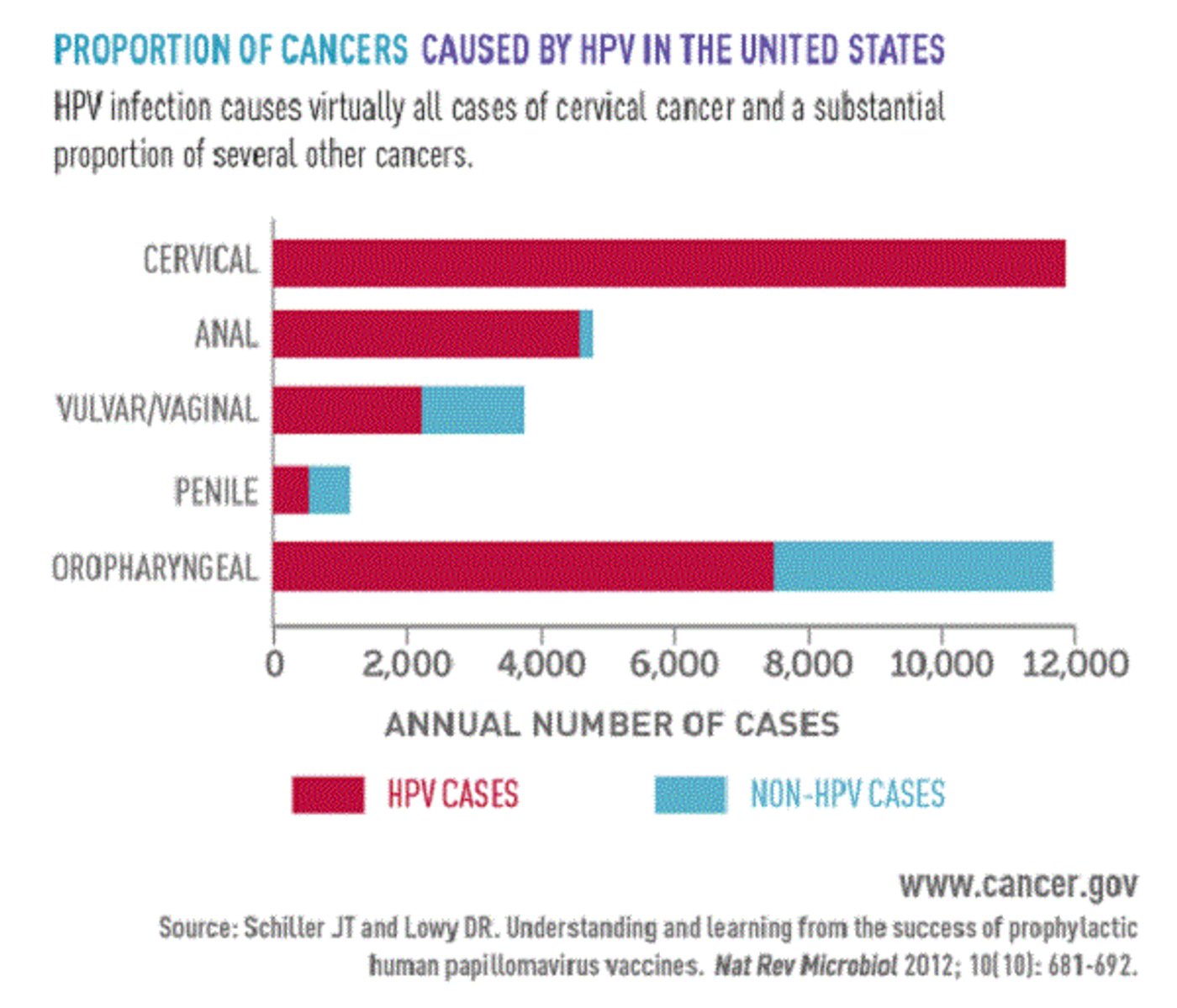
The facility
Diane M. Harper, MD, MPH, MS oversees HPV testing at UofL, which includes three clinic sites: Cardinal Station Family Medicine offices, Newburg Family Medicine offices, and the Centers for Primary Care. The staff comprises some 44 providers in total (including residents). Harper says her goal was to change the standard of care for women's health cervical cancer screening, and that meant opting for the only test approved by the FDA in 2014 for primary screening, the cobas HPV Test, from Roche Diagnostics.
“The benefits are our ability to better detect those women who are at real risk of having a CIN-3 lesion, and not identifying nondiseased women,” Harper says. “[The cobas HPV Test] has a high true-positive rate, with minimal false-positives identified.”(Invasive squamous carcinoma of the cervix is caused by a progression of preinvasive precursor lesions, cervical intraepithelial neoplasia (CIN), or dysplasia, with CIN-3 being considered severe.)
Harper, professor and chair of the Department of Family and Geriatric Medicine, University of Louisville, has more than 140 peer-reviewed, published works on this topic. She also holds joint appointments in the Departments of Obstetrics and Gynecology in the School of Medicine, Bioengineering in the Speed School of Engineering, and Epidemiology and Population Health and Health Promotion and Behavioral Health Sciences in the School of Public Health and Information Sciences; has served as an advisor to the World Health Organization for the past 15 years; and reviews research grants at the federal level for NCI, PCORI, AHRQ and the European Commission on Research, in addition to the Wellcome Trust, as well as others.
The lab
Unable to find a lab that runs this test in the greater Louisville area, UofL is now sending out its tests to a lab in a neighboring state—Tennessee, to be exact.
“The HPV test alone, for a certain group of women, is a [more] sensitive method of getting the correct snapshot on that patient’s cervical health than a combination of other tests,” such as doing a Pap and a co-test says board-certified cytopathologist Bradly D. Clark, MD, medical director, Women’s Health Laboratories, Poplar Healthcare/Women’s Health Laboratories, Memphis, Tenn. “It’s very efficient in its design in that you just do one test and have a better sensitivity than you would by doing cytology.”
The primary HPV screening tool, developed by Roche and performed on its cobas molecular platform, was approved for FDA use in early 2014. This screening method looks for presence of HPV nucleic acid in patients 25 years or older. Fourteen subtypes of high-risk HPV are detected. The two subtypes known to play the largest role in cervical dysplasia—HPV 16 and HPV 18—are discerned by the cobas method. Simultaneously, the cobas system also provides pooled-results detection of twelve other high-risk subtypes. The molecular testing uses a small portion of the liquid-based ThinPrep Pap test, which is standard in many provider settings.
In this new screening scheme, a patient who is negative for the HPV screen is placed on the provider’s standard screening interval(s). A patient who is found positive for either HPV 16 or HPV 18 is immediately referred to colposcopy. For the patient who is positive for the pooled HPV 12 subtypes, a Pap slide is prepared and reviewed by the cytology department. The next steps for that patient are driven by the reading of that slide. “In this new setting, a negative cobas HPV primary screening test provides about twice the reassurance for a patient they’re not going to develop a high-grade lesion in the next three years,” Clark says.
The medical profession, using cytology-based screening, has done a fantastic job of reducing the amount of cervical dysplasia, Clark notes. “But we’re up against technology now, since cytology has limitations,” he says. “Instead of co-testing [Pap slide plus HPV test], why can’t we just shortcut the entire method? Start, instead, with just an HPV test.”
Pap screening schemes have seen several iterations in the past generation. First, we saw the yearly Pap. Then came the attenuated interval, which spaced the Paps between every three to five years, depending on the age of the patient. Yet another iteration was addition of co-test (HPV test) to negative Pap test for patients 30 years or older.
For patients who are infected with a high-risk HPV, it generally it takes several years for it to develop into something serious, such as a high-grade lesion or worse, into cancer. “So, if you have that extended period of time, why would you Pap on a yearly basis?” Clark says. “This rational Pap testing interval for patients 25 years or older, uses a more sensitive method versus the ASC-US triage strategy we have used in the recent past. Instead, a positive cobas HPV test identified those at greatest risk.
Despite his embrace of the new testing algorithm, Clark’s not ready to write an obit for cytology just yet. “GYN cytology and the Pap slide are not going away,” he says. “The primary screening by HPV is used for those age 25 and above. Pap slides will still be necessary for those in a younger age group.
And further, slide interpretation will be necessary for the 12-pooled HPV positive, he says. “We’ve got a better technology now, and so the idea of doing a yearly Pap slide—that paradigm is being challenged—being replaced by a Pap every three or five years. Now there is the arrival of the primary HPV screening,” Clark says.
The future of HPV testing at UofL
As of March 23, 2015, UofL clinics are no longer performing co-testing. “Everything for our 25-and-older age range moves to primary HPV testing with HPV 16 and 18 genotyping (positives) going straight to colposcopy,” Harper says. “The 12 high-risk HPV types positive are triaged with cytology and those negative for high-risk HPV types return in five years for their next screen.
“The purpose for going to primary HPV screening is the superior detection of disease with minimal false positives and the increased screening interval that has been proven in multiple European trials (POBASCAM, SWEDESCAN, ARTISTIC, NTCC), as well as ATHENA,” Harper says. “Going to a less-than-five-year-repeat interval for screen-negative women violates the entire principle of cost-effective primary care, which is critical to the transformation of our current health care system.” About 4,000 patients there will be affected by the change in testing methods.
Harper urges the continual reinforcement of the cervical cancer screening message for both those choosing no HPV vaccination and those choosing HPV vaccination. “Gardasil and Gardasil 9 provides time-limited protection for only 43 percent of CIN 3 lesions, mandating cervical cancer screening to keep our rates of cervical cancer low,” she says.
This is the third article in a series about HPV testing. The prior articles are found here:
New Year Brings Overhaul of CPT Test Codes for HPV
https://labroots.com/user/news/daily/id/298/title/new-year-brings-overhaul-of-cpt-test-codes-for-hpv-trio-of-new-codes-differentiate-hpv-genotypes-by-cancer-risk-
Early-Adopter Backs Using HPV as Primary Screen for Cervical Cancer
https://labroots.com/user/news/daily/id/301/title/earlyadopter-backs-using-hpv-as-primary-screen-for-cervical-cancer-two-medical-societies-recently-issued-interim-guidance
Written by: Judy O'Rourke