Post-Trauma Treatment Relieves System-Wide Immune Reaction
The immune response after a traumatic physical injury is essentially the same as a body-wide bacterial infection: inflammatory, systemic, and lethal. From the Medical College of Georgia at Augusta University, scientists describe a new type of drug that could successfully treat both conditions.
Systemic inflammatory response syndrome (SIRS) describes the inflammatory reaction to either trauma or infection, initiated by increasing levels of a peptide called N-formyl. The response to N-formyl levels after trauma is essentially the same as the immune reaction to sepsis, a systemic bacterial infection. Patients experience elevated heart rate, fever, declining blood pressure, and swelling. Antibiotics treat sepsis, but how can trauma-induced SIRS be treated?
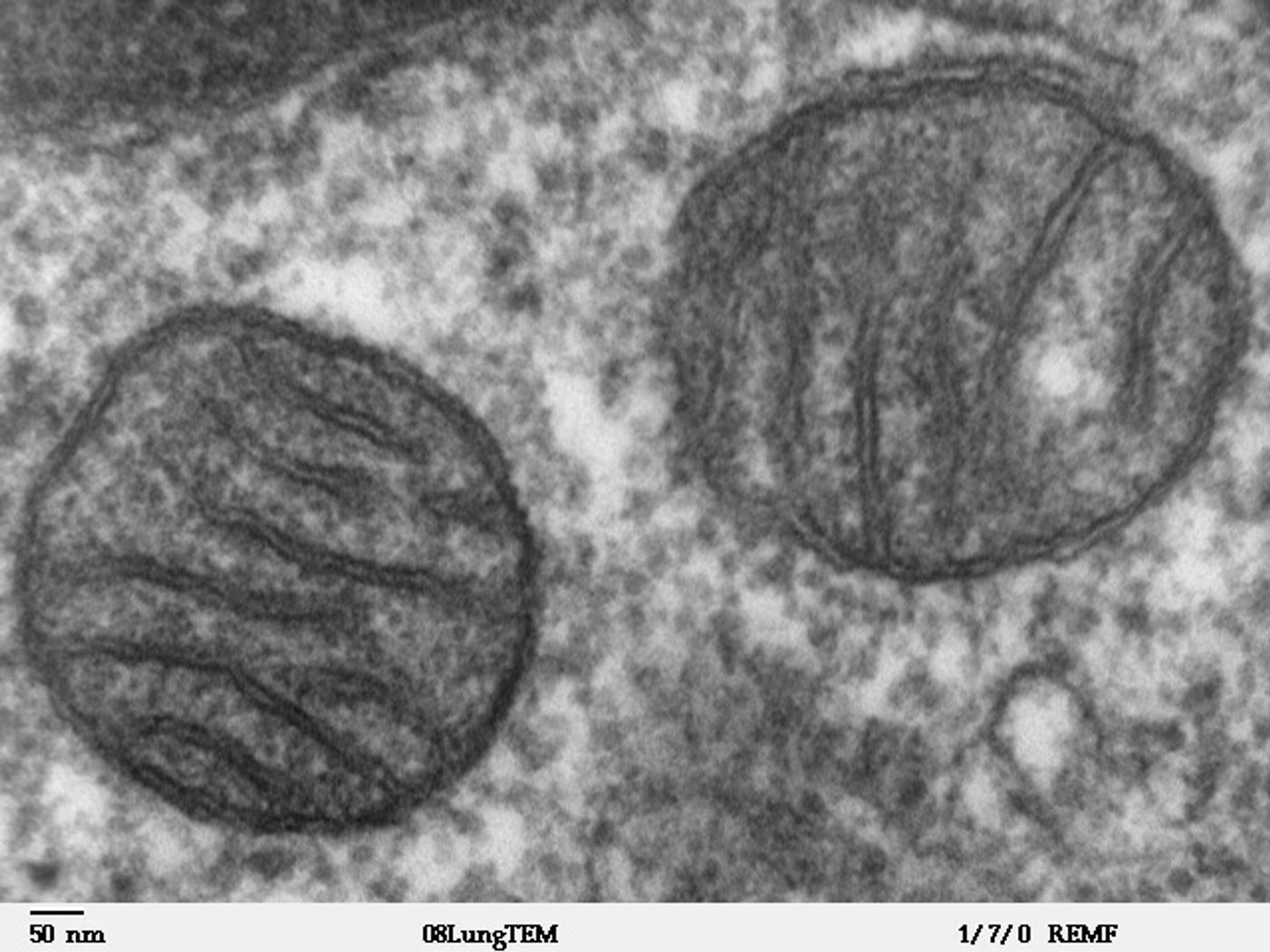
N-formyl peptides are released by damaged mitochondria, the organelles infamous for being the “powerhouse of the cell.” More specifically, mitochondria use N-formyl peptides to make energy for the body’s cells. When mitochondria are damaged as a result of trauma, they leak their contents, including N-formyl peptides, into the blood, which circulates all over the body.
Increasing levels of N-formyl peptides outside of the mitochondria is dangerous, as they impair vascular function by creating holes in the endothelium, the innermost layer of the blood vessel. A drug called deformylase deconstructs N-formyl peptides, making them harmless. Therefore, deformylase could be used to treat both sepsis and trauma-induced SIRS.
"Trauma releases fragments of mitochondria that still carry the signature from bacteria," explained senior author Dr. Camilla Ferreira Wenceslau. All mitochondria are believed to have originated from an age-old partnership between a cell and an aerobic prokaryote - a single-cell organism with no clear nucleus or organelle structure (bacteria are prokaryotes). Modern mitochondria have their own genome and two membranes.
The research team’s “danger theory," as Dr. Patricia Martinez Quinones describes it, is that “mitochondria used to be bacteria so when their contents are released our body treats them like an infection.”
Researchers tested their theory with both a mouse model of sepsis and human aortic endothelial cells incubated with N-formyl-rich plasma taken from trauma patients. In the mouse model, deformylase application improved vascular function and survival by 28 percent. In the human cells, deformylase preventing the endothelium from leaking fluid.
These findings offer deformylase as a new treatment option for SIRS, and they also highlight circulating levels of mitochondrial DNA and N-formyl peptides as biomarkers for improving diagnosis and treatment of trauma and sepsis patients.
Sources: Scitable by Nature Education, Medical College of Georgia at Augusta University