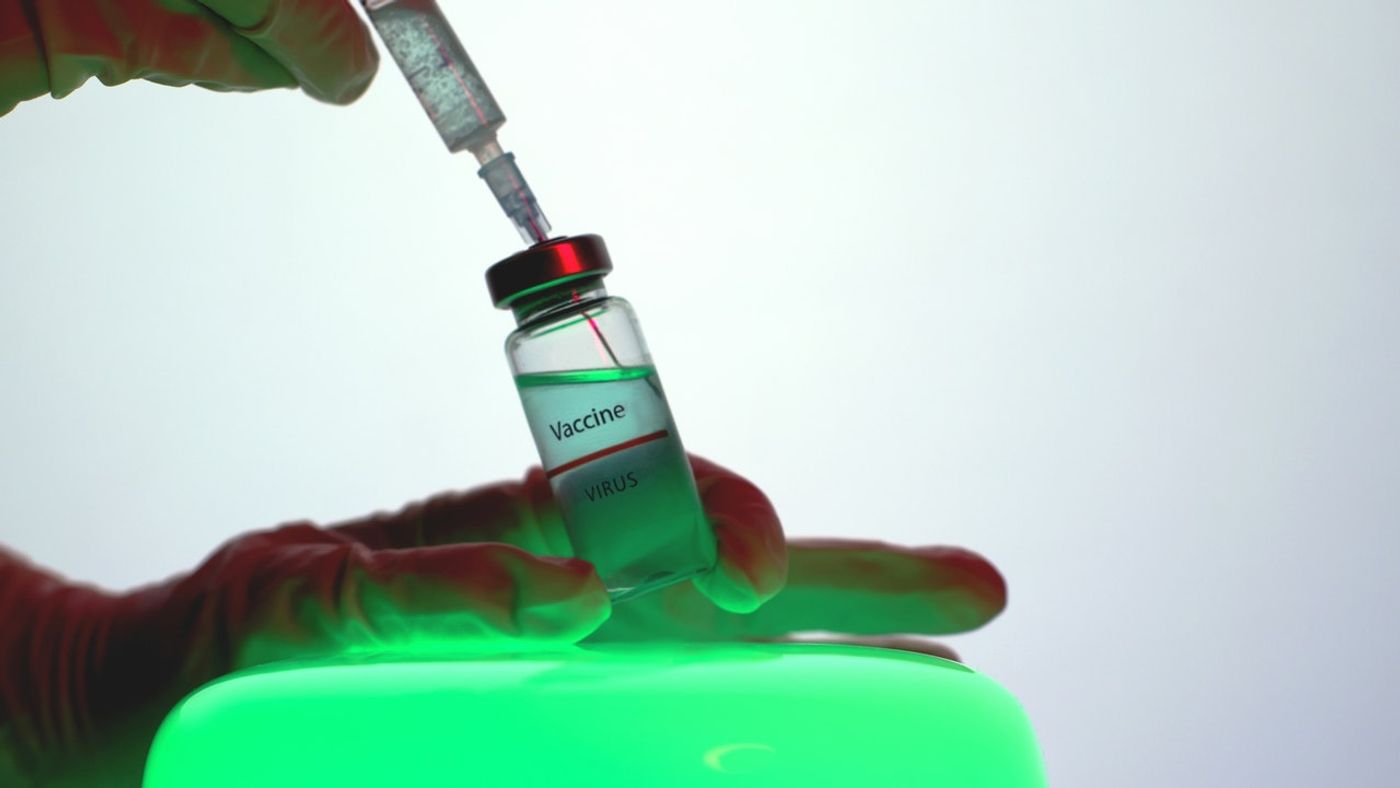
Yes, You Should Get Your Flu Vaccine.
A recent study published in Science Translational Medicine has provided fresh insights on how our immune systems protect us against the influenza virus and how vaccinations play a critical role in building these defenses. Immunologists at the University of Chicago studied the complex interplay between pre-existing immunity and vaccinations with a particular focus on cellular responses of B cells, a white blood cell that produces antibodies.
Influenza viruses fall into two main types, A and B, and routinely spread throughout communities during the annual seasonal flu epidemics. The proteins on the surface of the flu viruses tend to change as a result of mutation events, which means immune cells need to keep up by synthesizing antibodies that can recognize and neutralize “new” structural and functional proteins on the season’s dominant strain.
Once infected with the virus, the researchers found that the first wave of antibodies in circulation was produced by “old” B cells — ones that were primed by flu infections at some point during an individual’s childhood years. These antibody sequences pulled from the immune memory banks might recognize conserved proteins that don’t mutate much over time, but they are often unable to disarm and neutralize the virus.
"Most interestingly, we found that people who were actively sick with influenza had old antibodies that predominantly targeted parts of the virus that don't change -- but those antibodies specifically targeted non-neutralizing sites," said Haley Dugan, first author of the publication. "When we tested these same antibodies in mice, they weren't able to protect them from being infected with influenza."
Flu vaccinations help turbocharge this pre-existing immunity but triggering the production of antibodies that not only target conserved viral regions but are also able to neutralize viruses, creating a more robust shield against the fever, chills, and sore throat associated with the flu. In addition, those that received the vaccine also generated antibodies against newly mutated regions in the latest seasonal strain.
These findings are of particular relevance for drug developers on the quest for a universal flu vaccine. First, scientists need to understand what exactly tips the balance between neutralizing and non-neutralizing antibody production. Before this study, much of this remained a gray zone, with age, infection history, and vaccination status believed to play key roles.
Co-first author, Jenna Guthmiller said: "For people who have caught the flu, their pre-existing immunity may make them susceptible to infection or increase the severity of their influenza symptoms if their antibodies are targeting 'bad' or non-neutralizing viral sites."
This study revealed the mechanisms behind why seasonal flu vaccines are so imperative, primarily by tacking on neutralizing antibodies against newly-mutated viral proteins to pre-existing immune repertoires.
"This study provides a major framework for understanding how pre-existing immunity shapes protective antibody responses to influenza in humans," concluded the study’s lead author, Patrick Wilson. "We need more studies to determine whether the targeting of specific neutralizing and non-neutralizing viral sites directly impacts a person's likelihood of becoming ill."
Sources: Science Translational Medicine, EurekAlert!