Immune cells are not predestined to be either effector or memory cells, scientists from the Virginia Tech Carilion Institute find in a new study. In fact, by understanding the signaling pathway of certain inflammatory cytokines, scientists can potentially prompt more cells to become memory cells after an infection in order to improve vaccine efficacy.
If you’ve ever had the chickenpox and later were around someone who had them, you know that you didn’t have to worry about getting sick again. Although not all diseases and illnesses render us immune against that specific pathogen for the rest of our life, our body is able to store memory B lymphocytes for the next time we encounter the pathogen. Memory cells stimulate quicker antibody production when a pathogen infects the body for the second or third time. This is also the part of the immune function that make vaccines an effective preventative measure.
Vaccines present just enough pathogenic material to our immune cells for memory cells to be produced without causing a full-blown version of the disease. Then when the disease is encountered later, the body is already equipped to fight the infection.
New research surrounding the cell signaling between immune cells that stimulate memory cell production have scientists believing that they can improve the production of memory cells to make vaccines work more effectively.
"Central memory cells allow for such a quick response to antigens that infection typically doesn't have a chance to form. You might not even know you've been infected," said Paul McDonald, a researcher from Virginia Tech. He is also first author on the study paper, published in
Nature Communications this week.
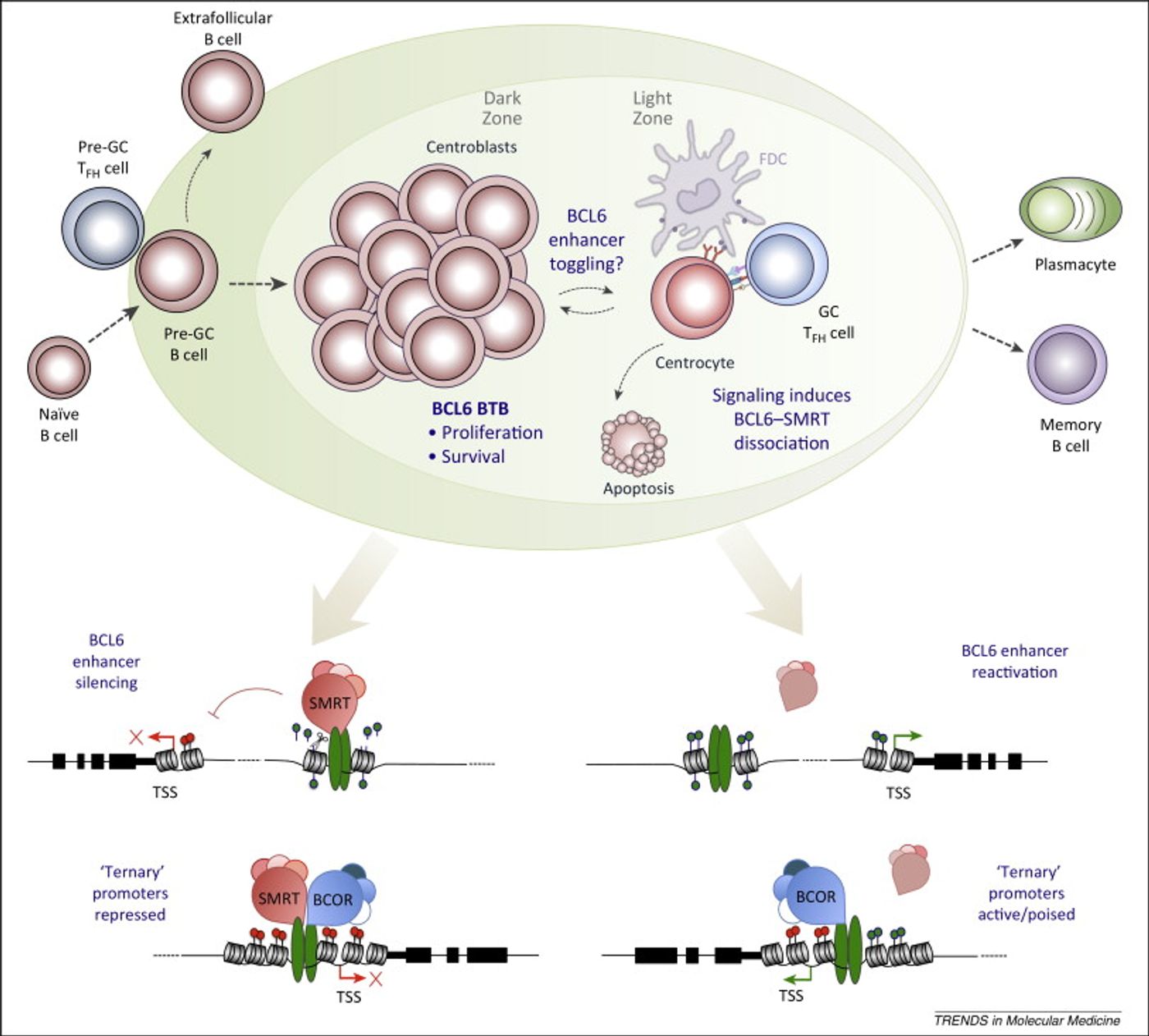
Production of a cell-signaling cytokine, interleukin-2 (IL-2), increases until the peak of an infection, and as these levels drop effector cells stimulate production of a protein called Bcl-6. In response, T follicular helper (TFH) cells are produced from remaining effector cells. TFH cells help facilitate B cell differentiation into antibodies (
Annual Review of Immunology).
What scientists did not know until now, however, is that in addition to stimulating production of TFH cells, Bcl-6 also induces memory cell production.
In addition, the team found that the “effector cells not only have both the T follicular helper cells and central memory profiles, but they also expressed receptors for two different proteins: interleukin-6 and interleukin-7.”
These cytokines aid in TFH cell development and memory cell regulation, and McDonald’s team found that they could also be the determining factor in whether an effector cell becomes a TFH cell or a memory cell.
"Formation of these [memory] cells is critical for a vaccine to work well,” McDonald said.
Source:
Medical News Today