Immune responses can be unequal and misguided, resulting in certain conditions like allergies and autoimmune disorders. A new testing method developed by scientists from Thomas Jefferson University provides a brand-new opportunity to predict an individual’s immune response to different antigens.
The new testing method, called “CaFlux,” quantifies the strength of the immune response to a particular antigen, like pollen or bacterial components. CaFlux is more sensitive and quicker to yield results than any other similar method to date, and it’s able to test a wide variety of antigenic targets.
"A future application of this test could help determine who might respond with a sneeze versus who might respond with anaphylactic shock before it happened,” explained senior author Yuri Sykulev, MD, PhD.
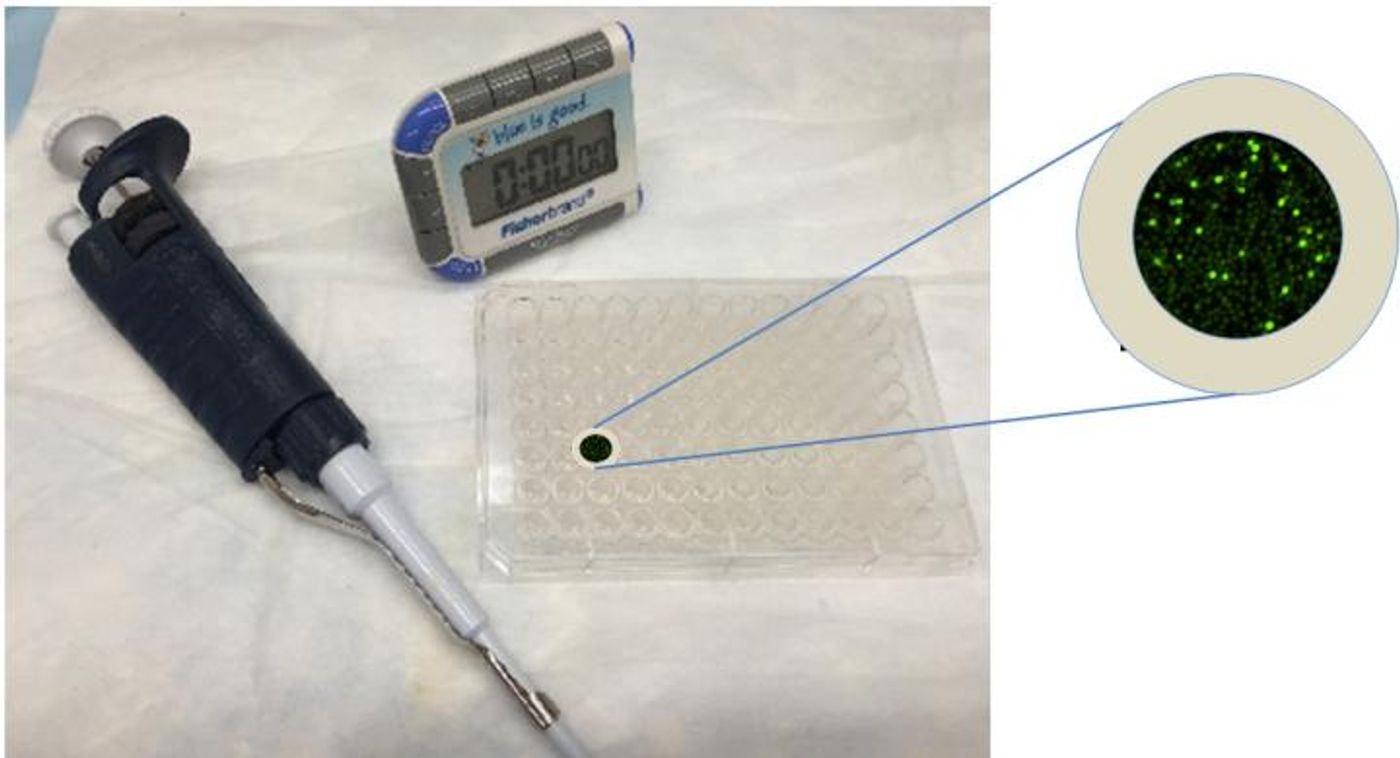
The CaFlux process begins with immune cells that are known to respond to potential antigens. A variety of antigens are then flowed over the immune cells to look for immune cell-antigen connections. If an antigen and immune cell pair occurs, the joining of their receptors triggers the influx of calcium through calcium channels, and green fluorescence proteins are activated, detected with a microscope, and measured with image-reading software.
The stronger the connection, or the more capable an immune cell is in binding to an antigen, the more calcium ions that can flow into the cell through the channels, and the brighter the glow of green fluorescent protein. Quite the opposite happens when a weaker match occurs: less calcium and a much dimmer glow.
CaFlux can accurately depict the number of T lymphocytes that respond in each sample of antigens, as well as how powerfully and how quickly each cell responds to antigen. The applications for CaFlux in the clinical setting are numerous; doctors could potentially be able to predict how an individual would react to certain antigens. This could help doctors decide treatment options for patients considering organ transplantation, those with autoimmune disease and allergies, and individuals with cancer.
To test CaFlux in a real-life setting, researchers used T lymphocytes from a bone marrow transplant recipient, testing for immune cell reactivity to cytomegalovirus (CMV). Infections from cytomegalovirus rarely cause problems in people with healthy immune systems, but they can be deadly for immunocompromised people, like those who receive immunosuppressants before a bone marrow transplant.
The CaFlux results showed a slow and weak T lymphocyte response to CMV antigens, suggesting that the individual’s immune system was not prepared to fight off a CMV infection.
"That weak response was mirrored by what happened in the clinic," said oncologist Neal Flomenberg. "The patient's CMV reactivated while the immune system was still rebooting and unable to mount a strong response against CMV, and he had to be treated for the infection. Had we been able to monitor this patient's immune system's ability to respond to CMV, we may have been able to tailor his treatment to better keep the CMV in check."
The new CaFlux test could help doctors avoid dangerous situations by knowing ahead of time how one patient might respond to certain immune targets. The current study was published in the journal
Nature Communications.
Source:
Thomas Jefferson University