Scientists Unveil Unique Factors Contributing to Autoimmune Disease
Many autoimmune diseases come in waves, where symptoms temporarily get worse followed by a time of little to no signs of disease. There are a lot of factors that govern why and how an autoimmune disorder occurs, but a recent study was focused specifically on the quality of autoimmunity that causes flare-ups of disease. The same study ultimately resulted in the revealing of two key factors involved in this process, providing doctors and patients new hope for an autoimmune treatment.
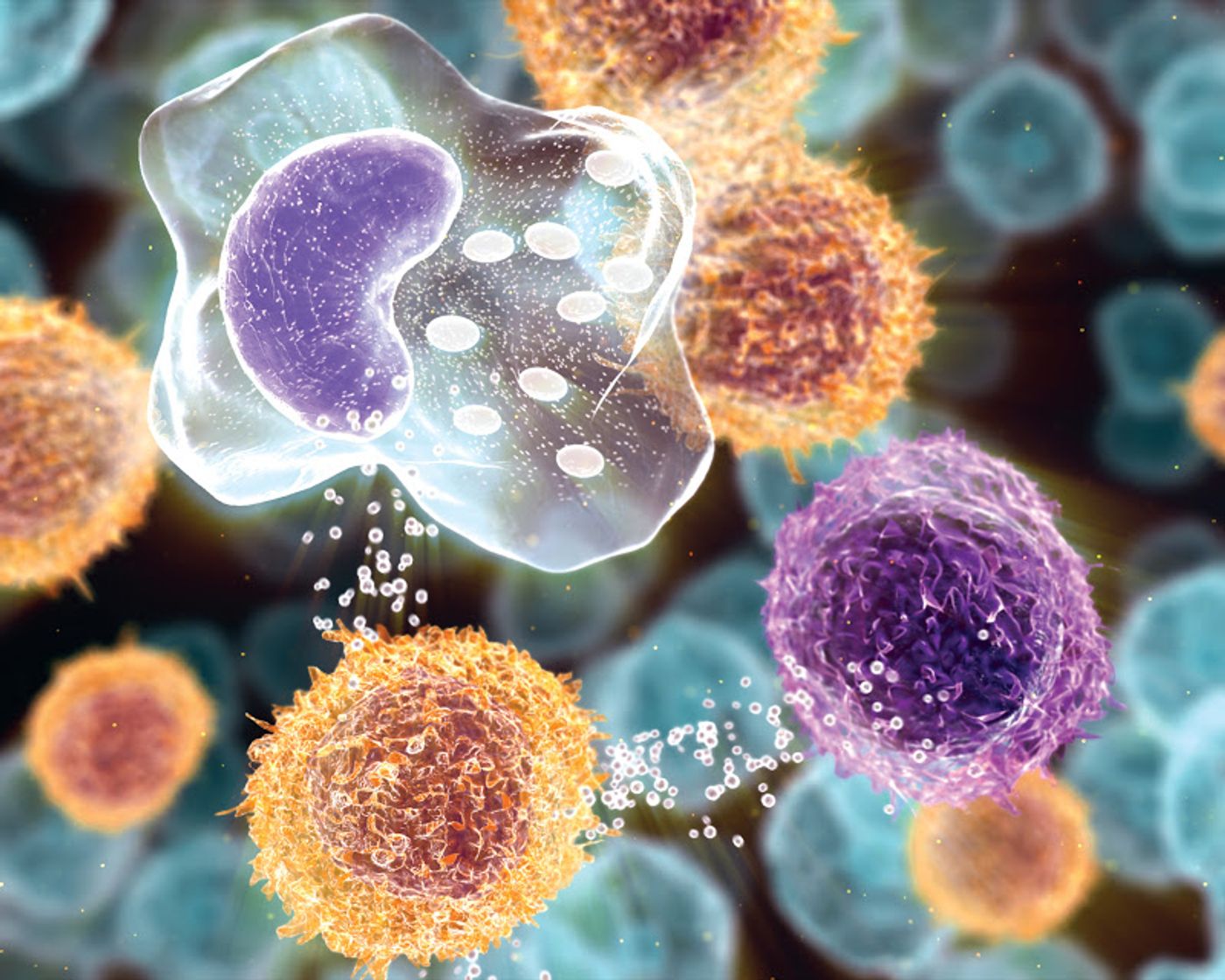
From the Schepens Eye Research Institute of Massachusetts Eye and Ear Infirmary, researchers focused on a mouse model of dry eye disease, an autoimmune disease that shares molecular similarities with multiple sclerosis, rheumatoid arthritis, inflammatory bowel disease, and another chronic inflammatory eye disorder called uveitis. The common denominator is Th17 cells, which can continue living in the circulation for a relatively long time as memory cells.
They quickly identified interleukins (IL) 7 and 15, immune cytokines secreted by other immune cells that act as cell-signaling proteins. IL-7 and IL-15 play the role of memory regulation for Th17 cells, the researchers discovered. This enlightenment meant two new targets for treatments.
"By selectively targeting the production and expression of IL-7 and IL-15, we may be able to prevent the development of chronic autoimmune disorders,” explained senior author Reza Dana, MD, Msc, MPH. Dana’s study is the first to uncover how Th17 cells maintain memory.
During the study, when scientists neutralized IL-7 and IL-15, the result was a significant decrease in the number of memory Th17 cells, further highlighting the potential for the two interleukins as targets for a new autoimmune disease treatment.
"In the case of dry eye disease, many of the treatments are showing limited efficacy in patients that do not have a highly inflamed eye," Dana said. "Targeting the chronic, immune nature of autoimmune diseases may be a better strategy for controlling these conditions."
Dana’s study was recently published in the Journal of Autoimmunity.