Persistent Infections Promote Long-Term Immunity
Both natural and artificial bestowal of long-term immunity comes with risks. The same pathogen or vaccine that is conferring resistance protects an individual from disease and simultaneously poses a risk for disease later in life when an individual is vulnerable due to age, illness, or both.
Researchers from the Washington University School of Medicine studied the balance of risks and benefits that come with persistent infections, looking for ways to improve vaccine development and treatment designs for diseases like leishmaniasis, where initial exposure to the parasite prevents subsequent infections later in life.
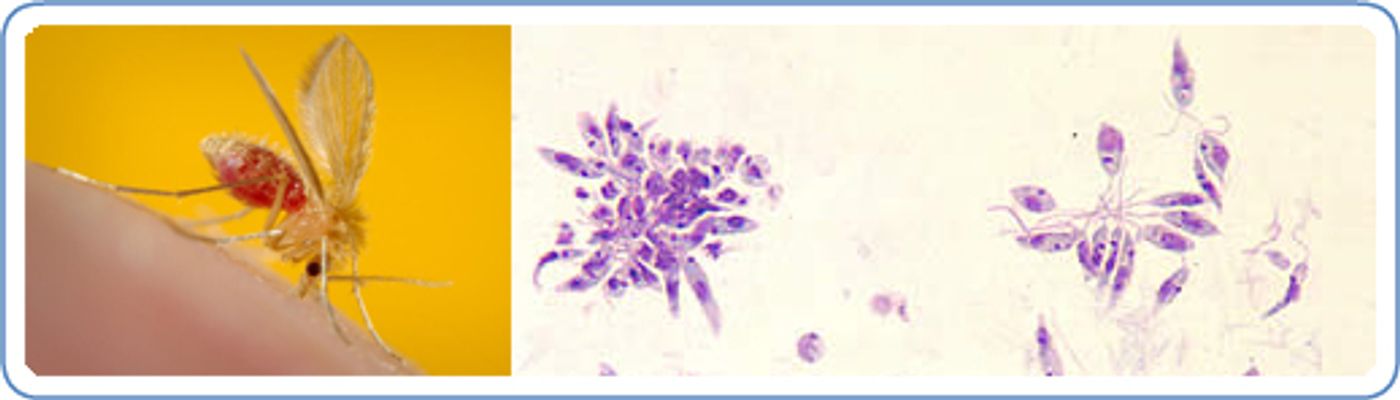
Leishmaniasis is a parasitic disease found in individuals who live in the tropics, subtropics, and southern Europe; it is classified as a “Neglected Tropical Disease.” The disease is spread via the bite of a phlebotomine sand fly, which harbors the pathogen responsible for the infection. The parasite can cause either skin sores - “cutaneous leishmaniasis” or an infection of internal organs like the spleen, liver, and bone marrow - “visceral leishmaniasis.”
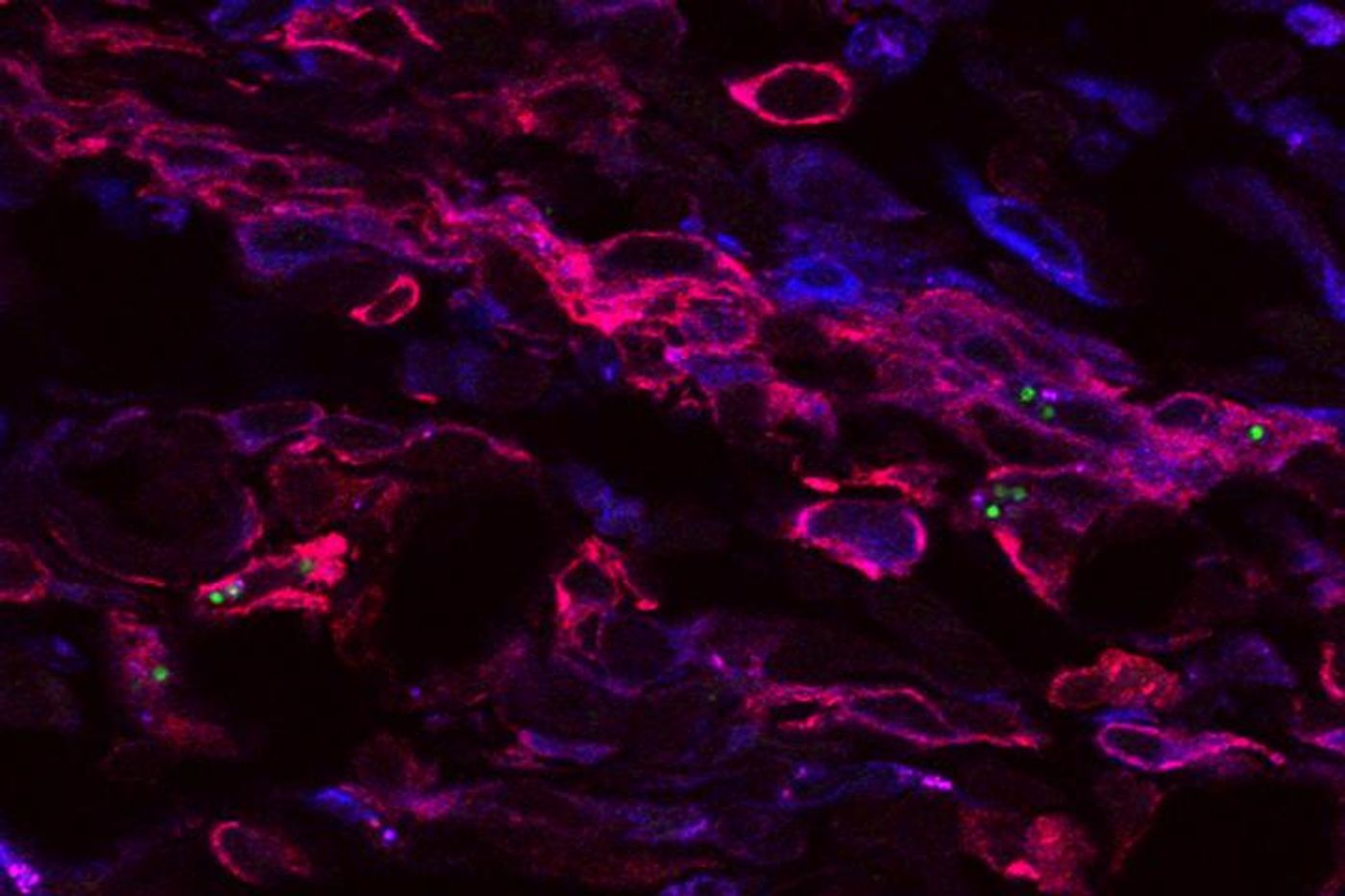
Washington University scientists studied leishmaniasis parasites in mice, designing fluorescent markers that could distinguish different types of cells. From the markers, they found that a large majority of the parasites that persisted after an infection seemingly cleared shacked up inside of the very immune cells capable of killing them. But other than that strange finding, the parasites appeared to be normal in shape and size.
Another bizarre discovery was that although the parasites were continuing to multiply, the total number of living parasites stayed the same over time. "We were unable to show directly that the parasites were being killed,” explained senior author of the study Stephen Beverley, PhD. “But some of them must have been dying because the numbers weren't going up."
Beverly and the rest of the research time believe that this continuous multiplication is the process responsible for long-term immunity and protecting people with infections like leishmaniasis from getting the same infection twice.
"It seems that our immunologic memory needs reminding sometimes," said first author Michael Mandell, PhD. "As the persistent parasites replicate and get killed, they are continually stimulating the immune system, keeping it primed and ready for any new encounters with the parasite."
"People had been thinking of the role of the immune system in persistent infection in terms of mowing down any pathogens that reactivate in order to protect the body from disease," Beverly said. "What was often overlooked was that in the process of doing this, the immune system is constantly being stimulated, which potentially promotes protection against future illness."
A sand fly (left) and Leishmania parasites in culture (right). Source: Public Health Image Library
The next step for Beverly and his team might be to research developing a vaccine that mimics the pattern of “reminding” to keep the body immune to a particular disease, even if it poses a risk of infection to the individual receiving the vaccine. “For some of these organisms, solid, long-term protection may come at the price of persistent infection,” Beverly explained.
This approach could be applicable to many other diseases other than leishmaniasis that also cause persistent infections: tuberculosis bacteria, herpes and chickenpox viruses. Leishmaniasis alone causes tens of thousands of deaths every year.
Beverly’s study was recently published in the journal Proceedings of the National Academy of Sciences.
Sources: CDC, Washington University School of Medicine