A Newborn's First Breath Forges A Lifetime of Immunity
More than ten thousand liters of air enter the lungs on a given day, but it’s not just oxygen that fills the lungs; pathogens and pollutants also hitch a ride into the body via breathing. To combat these invaders, the immune system employs an intricately-designed mechanism that simultaneously keeps pathogens at bay and soothes the lung tissue to allow for healthy exchange of oxygen and carbon dioxide with each breath.
A new study in mice explored how a newborn immune system “learns” how to preserve the delicate balance between remaining dormant and actively mounting a response against any bacteria, virus, or other foreign agent that enters the lungs after birth.
During this study, scientists at the CeMM Research Center for Molecular Medicine of the Austrian Academy of Sciences identified a series of immune cells and molecules specifically designed to keep this balance, cells that newborn lungs employ upon first breath.
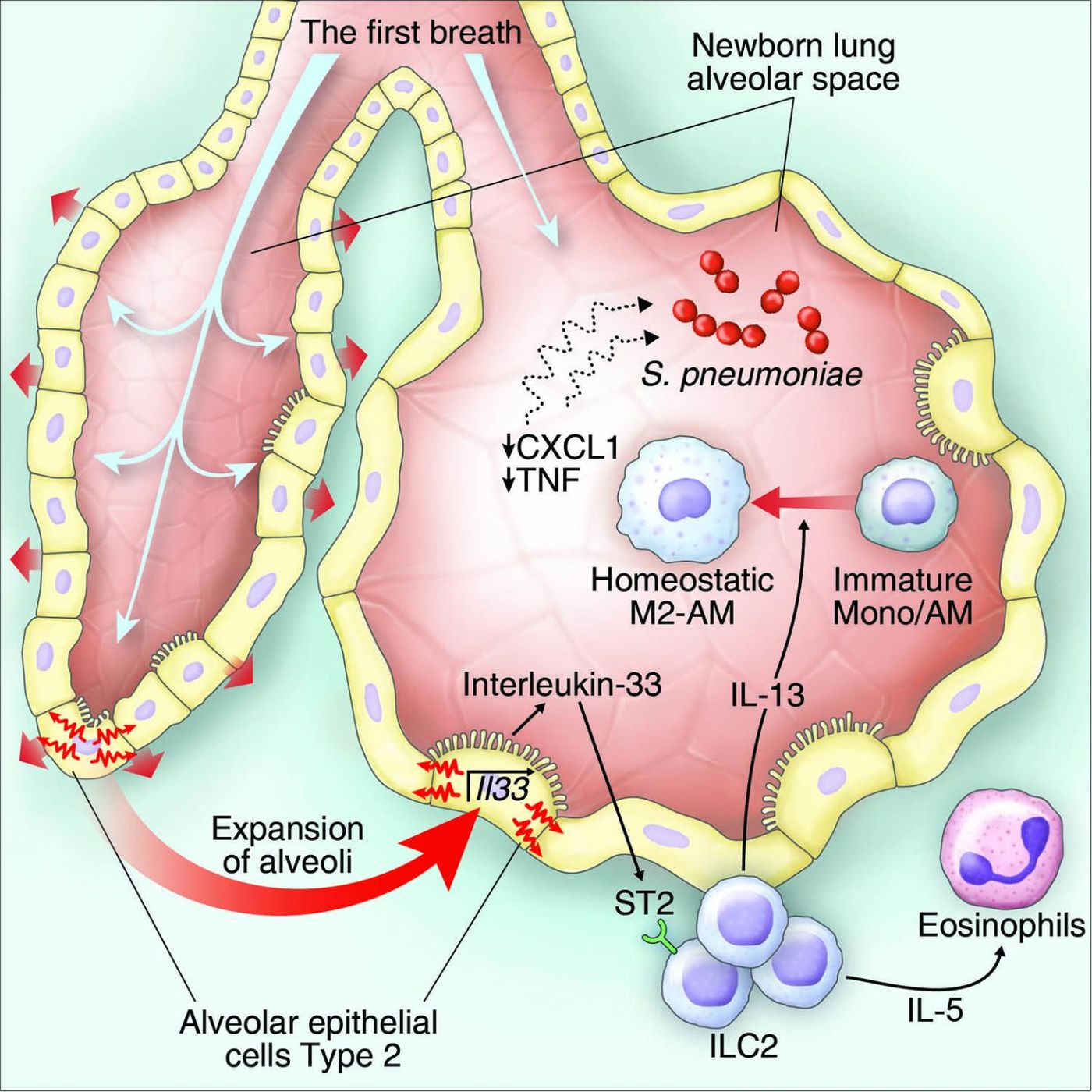
Upon birth, “spontaneous ventilation” occurs that immediately stimulates the release of a cytokine called interleukin-33 (IL-33). This chemical messenger then signals to type 2 innate lymphoid cells (ILC2s) which, according to IL-33 direction, travel into the lung tissue to release another cytokine, IL-13. This cytokine then induces macrophages in the lung tissue to become anti-inflammatory, allowing the peaceful exchange of gases necessary for respiration.
In addition to respiratory tissue, ILC2s are found in gastrointestinal and skin tissue where they seem to perform a completing opposite role; some studies have shown that they promote allergic inflammation. Whether ILC2s stimulate anti- or pro-inflammatory macrophages seems to depend on which interleukin signals to them. In the case of newborn lung maintenance, it is anti-inflammatory activity instructed by IL-33.
"Now we understand that right after birth, ILC2s are responsible for the differentiation of alveolar macrophages into specialized cells that keep the immune system in check and ensure that the lungs stay calm and healthy to ensure proper gas exchange,” explained first author Simona Saluzzo, PhD Student at CeMM.
However, overactive anti-inflammatory macrophages can also have a negative impact on the lungs, preventing the immune system from adequately attacking pathogens. “The mechanism that maintains the lung function of gas exchange at the same time explains why bacterial pneumonia is the primary cause of death by an infectious disease in Western countries,” explained senior author Sylvia Knapp.
The delicate balance required in the lungs for both immune defense and adequate gas exchange has never been so clearly evident. Given the ubiquity of environmental pollutants and pathogens, it is vital that the immune system flawlessly maintains homeostasis in the lungs, either on its own or with clinical intervention.
Knapp’s study was recently published in the journal Cell Reports.
Sources: Current Immunology Reviews, Advances in Immunology, CeMM Research Center for Molecular Medicine of the Austrian Academy of Sciences