Immune Network Prevents Organ Damage During Parasitic Infection
A parasite called Trypanosoma cruzi causes one of five diseases designated by the Centers for Disease Control and Prevention as “neglected parasitic infections.” It’s called Chagas disease, named after the Brazilian physician who discovered it for the first time over a century ago. The immune system has a plan in action to fight parasitic infections like Chagas disease, but only recently have scientists begun to fully understand exactly how immune cells get the job done.
T. cruzi triggers a unique response in the immune system that revolves around the release of an immune messenger called a cytokine, specifically interleukin (IL) 17. Just enough IL-17 can clear a T. cruzi infection, which destroys heart and digestive muscle when unchecked, but too much IL-17 can cause chronic tissue damage. As is common with the immune system, a regulatory pathway is put in place to prevent tissue damage from happening.
Aware of all of this, Osaka University scientists were interested in going one step further to understand the immune response to Chagas disease. Going into their new study, the knew that before IL-17 is produced in response to a T. cruzi infection, production of another cytokine, IL-23, leads to an influx of CD4+ T cells, which ultimately are responsible for producing IL-17.
They were also curious about the involvement of a protein called BATF2, which is activated by cytokine signaling cells during T. cruzi infection. However, researchers were unsure of its direct connection to IL-17, if one existed.
During their newest study, published in The Journal of Experimental Medicine, Osaka scientists built on their entire body of preexisting knowledge to unwrap the details of the complex IL-17 network responsible for preventing multi-organ damage during Chaga disease and chronic tissue damage from excessive IL-17.
From their study, they saw that BATF2-deficient mice produced much more IL-17 and IL-23 in response to T. cruzi infection than mice with fully functional BATF2. However, it wasn’t clear whether BATF2 was actually necessary for killing the parasites.
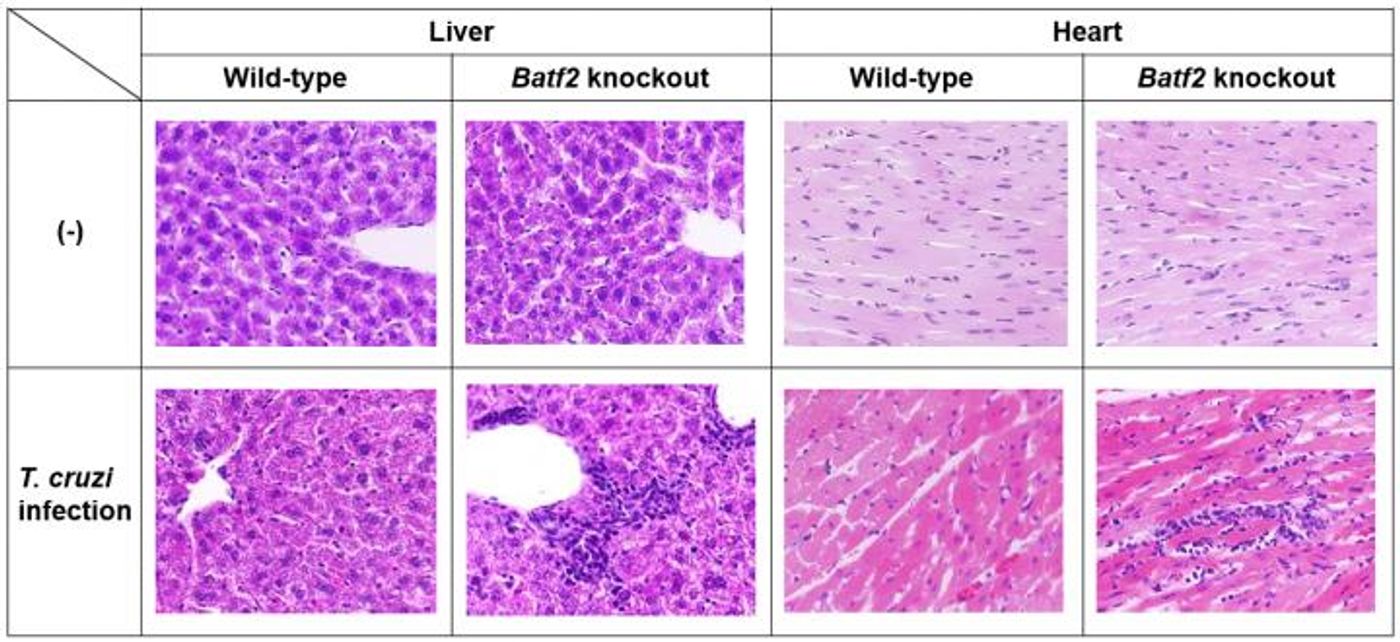
"When we infected both Batf2 knockout and control mice with the same amount of T. cruzi, the knockout mice had a lower number of parasites and improved survival, probably because of increased IL-17 levels," explained Hisako Kayama co-author of the report on the study. However, there was one problem. "The extent of immune activation and tissue damage was more severe.”
While the removal of BATF2 led to more IL-17 to better smother the T. cruzi infection, lacking the protein also led to chronic tissue damage from excessive IL-17 levels that regulatory immune cells couldn’t keep under control.
"This novel function of BATF2 prevents the excessive IL-17 response that would otherwise cause immunopathology during parasitic infection," explained corresponding author Kiyoshi Takeda.
The dual role of BATF2 made apparent in the present study is not thought to be unique to T. cruzi infection; similar BATF2 activity probably occurs in other types of infection, researchers say, because the protein has been seen expressed in several other cell types.
Chagas disease affects 6-7 million people worldwide, mostly in rural areas stricken with poverty.
Sources: Osaka University, CDC, Journal of Immunology