Treating Untreatable Heart Failure with Cardiac Macrophages
Immune cells called macrophages contribute to an untreatable type of heart failure. At least, this type of heart failure is untreatable for the time being. From Massachusetts General Hospital (MGH), scientists identify key differences between how different types of heart failure develop. Bringing these differences to light could aid in the creation of new treatments for heart failure.
A specific type of heart failure characterized by “preserved ejection fraction” is also called diastolic heart failure. Ejection fraction is a measure of how much blood is getting pumped out the heart with each heartbeat. When ejection fraction is “preserved,” it means that the heart is contracting normally, but its ventricles do not relax normally.
Diastolic heart failure is directly compared to systolic heart failure, a result of “reduced” ejection fraction. This type of heart failure deals with the opposite problem: the heart muscle’s inability to contract normally.
Symptoms of both diastolic and systolic heart failure are similar, but it’s very likely that each condition requires a different treatment approach. In the present study, MGH scientists focus on diastolic heart failure, which makes up about 50 percent of all human heart failure cases.
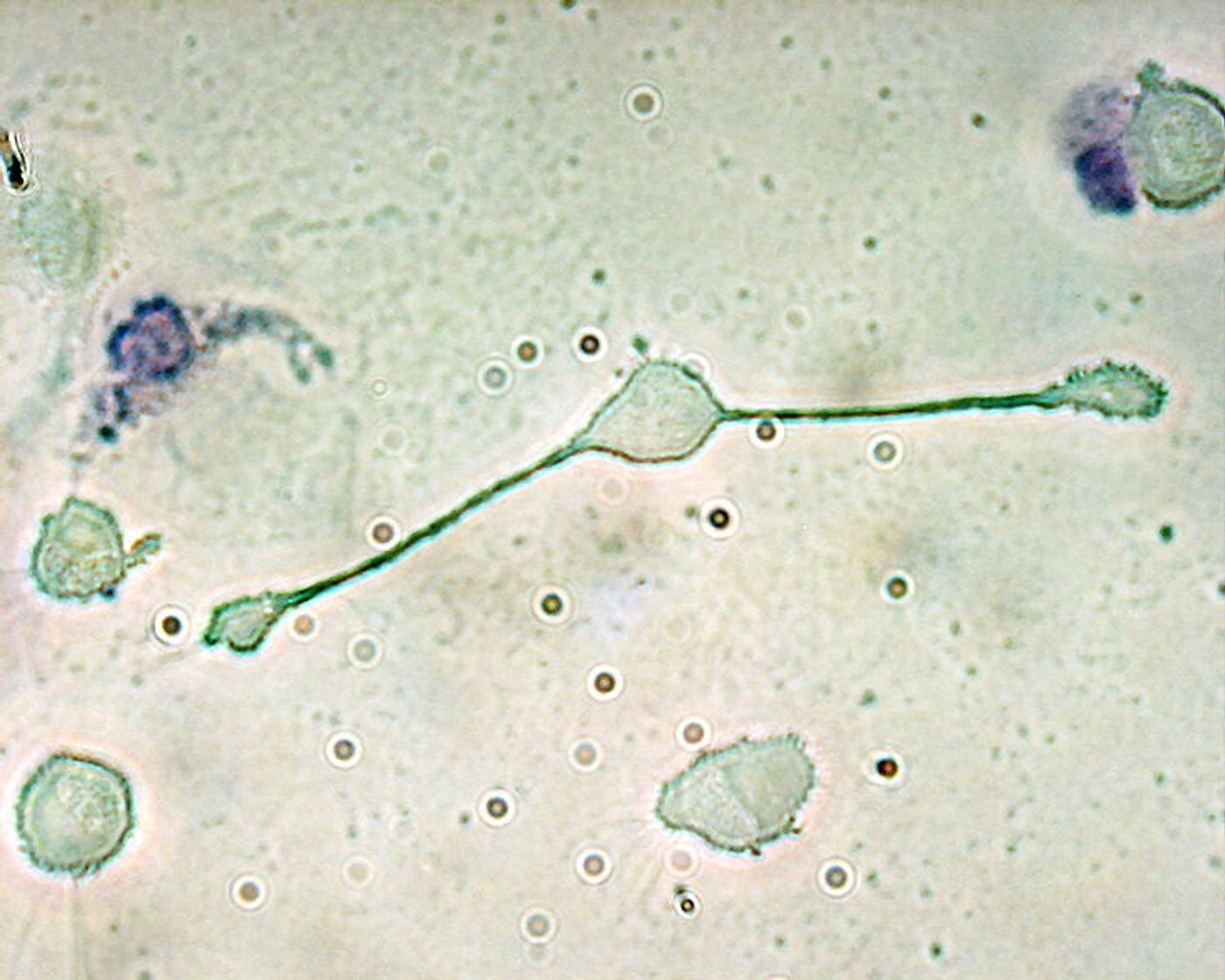
"We show that macrophages - white blood cells primarily known for removing cellular debris, pathogens and other unwanted materials - are actively involved in the development of [preserved ejection fraction]," explained lead author Maarten Hulsmans, PhD, from MGH. "These findings put macrophages on the map when it comes to [diastolic heart failure] therapy and open up previously unexplored treatment options."
To identify a potential set of solutions for diastolic heart failure, scientists first needed to better understand how the disease develops: when cellular interactions in the heart, including macrophages, lead to disease instead of promoting normal heart activities.
In a healthy response, macrophages activate cells called fibroblasts to “reinforce” tissue damaged by a heart attack. But if macrophages activate too many fibroblasts, damaged tissues become stiff, which only makes cardiac function worse.
In their study, researchers used two mouse models of diastolic heart failure, assessing the cellular repercussions of preserved ejection fraction. Initially, they saw elevated levels of macrophages in the left ventricle as well as more evidence of interleukin (IL)-10, a chemical messenger of the immune system that promotes fibroblast activation.
In one of the models, research induced IL-10 deficiency in cardiac macrophages. This resulted in lower macrophage levels and, subsequently, lower cardiac fibroblast activity.
"Through their participation in the remodeling of heart tissue, these macrophages increase the production of extracellular matrix, which reduces diastolic relaxation,” Hulsmans explained. “Our findings regarding the cell-specific knockout of IL-10 are the first to support the contribution of macrophages to [diastolic heart failure]."
With the findings from Hulsmans’s new study come hopes for new drug development based on the new understanding of the relationship between heart muscle cells, macrophages, and fibroblasts.
The present study was published in the Journal of Experimental Medicine.
Sources: American Heart Association, Massachusetts General Hospital