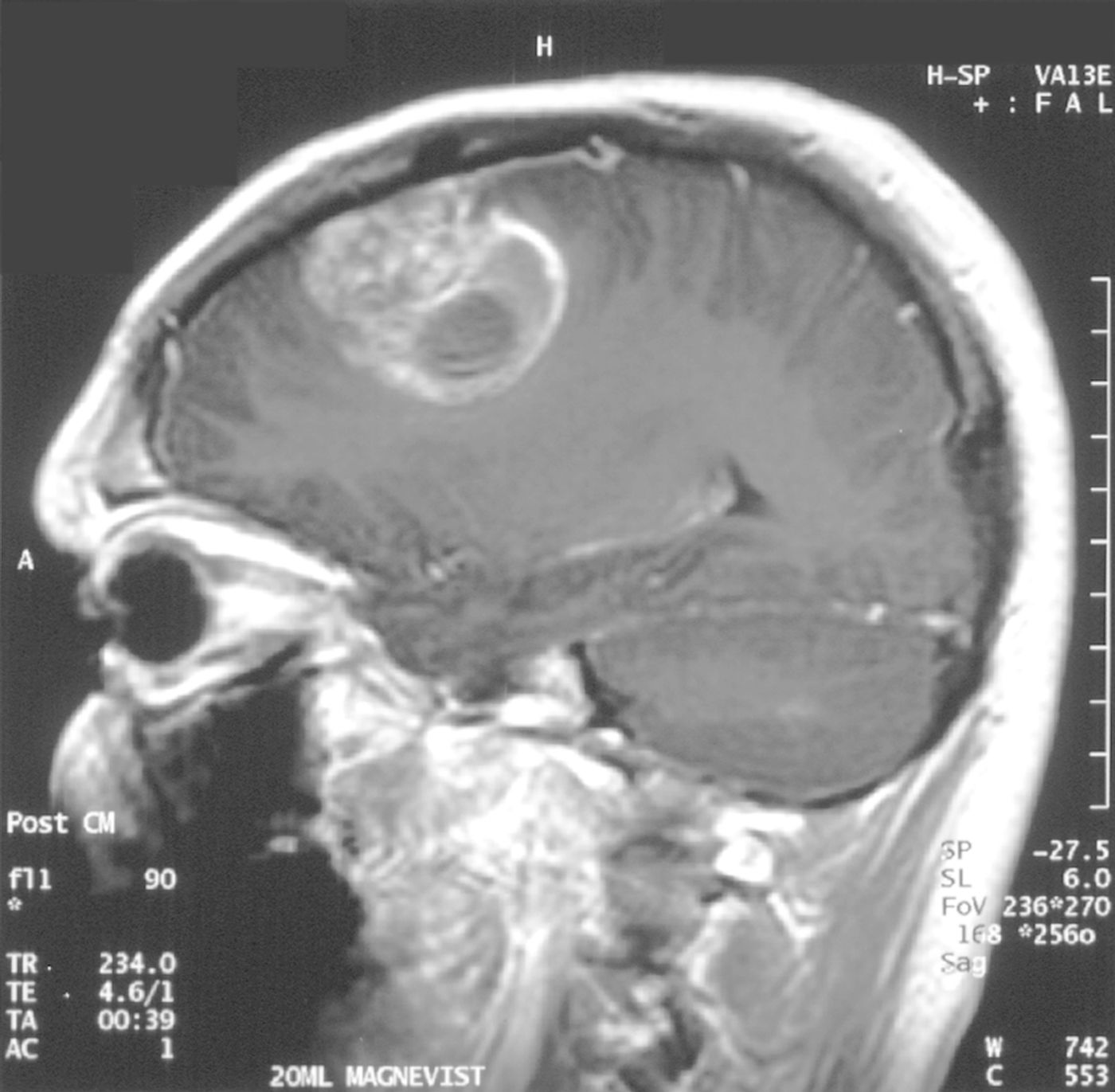
How does brain cancer escape the immune system?
One of the most lethal forms of brain cancer owes most of its deadliness to its evasion of the immune system - a nasty trick that prevents T cells and other immune defenses from doing their job. In a new study from Brigham and Women’s Hospital, scientists learn a little bit more about how tumors play hide-and-seek with the immune system, potentially uncovering new ways to detect and treat brain cancer.
Glioblastoma is a type of cancer that develops from astrocytes, supportive cells that live in the brain. This type of brain cancer is very malignant; tumor cells multiply quickly and tap several blood vessels for a steady supply of oxygen and nutrients. Glioblastoma tumors are usually found in the cerebral hemispheres of the brain and make up 15.4 percent of all primary brain tumors. Likelihood of developing glioblastoma increases with age, especially for men. The median survival for adults with glioblastoma is two or three years.
The new study focuses on extracellular vesicles (EVs), which glioblastoma tumor cells, like other cells, produce. EVs are known for their role in intercellular communication; cells often discard EVs as they undergo apoptosis, or programmed cell death. But in the case of brain cancer, tumor cells produce EVs to suppress the immune response.
EVs help tumors do so by providing a protein called PDL-1, which contributes to T cell deactivation. Cancer cells also “hijack” immune checkpoints to prevent the immune system from mounting an anti-cancer attack. EVs also contain DNA and RNA that help tumor cells not just survive, but flourish in the human body.
"This is the first time that anyone has observed that immune checkpoints can operate through extracellular vesicles and not just through the cell surface," explained co-corresponding author Sean Lawler, PhD. "This is a new concept, suggesting that these vesicles can work more distantly from the tumor cells."
In the study, researchers also found traces of DNA from EVs in the blood of glioblastoma patients, indicating EVs as a potential biomarker for the disease.
Researchers also analyzed blood samples from both healthy people and from glioblastoma patients. Out of 21 samples, researchers found elevated PDL-1 DNA in isolated EVs in 14 samples. The more PDL-1 DNA, the largest the tumors tended to be.
The findings of this study indicate a new opportunity for scientists to use EVs as a biomarker for glioblastoma, but studies with a larger group of participants are needed to confirm the significance of the results.
The present study was published in the journal Science Advances.
Sources: American Brain Tumor Association, Nature Reviews Drug Discovery, Brigham and Women’s Hospital