Gene Editing Tools Reveal Two Key Genes Involved in Influenza Infection
Using CRISPR/Cas9 gene editing tools, researchers identified two genes responsible for suppressing the immune system and allowing the influenza virus to infect human lung cells. From the University of Chicago Medical Center, scientists describe how these genes can change the therapeutic approach to the flu.
Flu treatments are limited, and vaccines don’t always work. The flu virus is notorious for mutating, changing so scientists have to change treatments every year. The new genetic screening tool identified key genes involved in the immune response to the flu, and the same tool could also help uncover key genes involved in other diseases.
"The next wave of antiviral treatments will be in part directed toward the host, so our work helps us get a better understanding of what proteins and pathways are utilized by the influenza virus,” explained lead author Julianna Han.
The CRISPR/Cas9 gene editing tools enabled scientists to knock out specific genes, meaning they suppressed expression of those genes in human lung cells. How does it work? Researchers used those tools to create a library of modified human epithelial lung cells, each missing a different gene, so scientists can see which changes impact the response to flu.
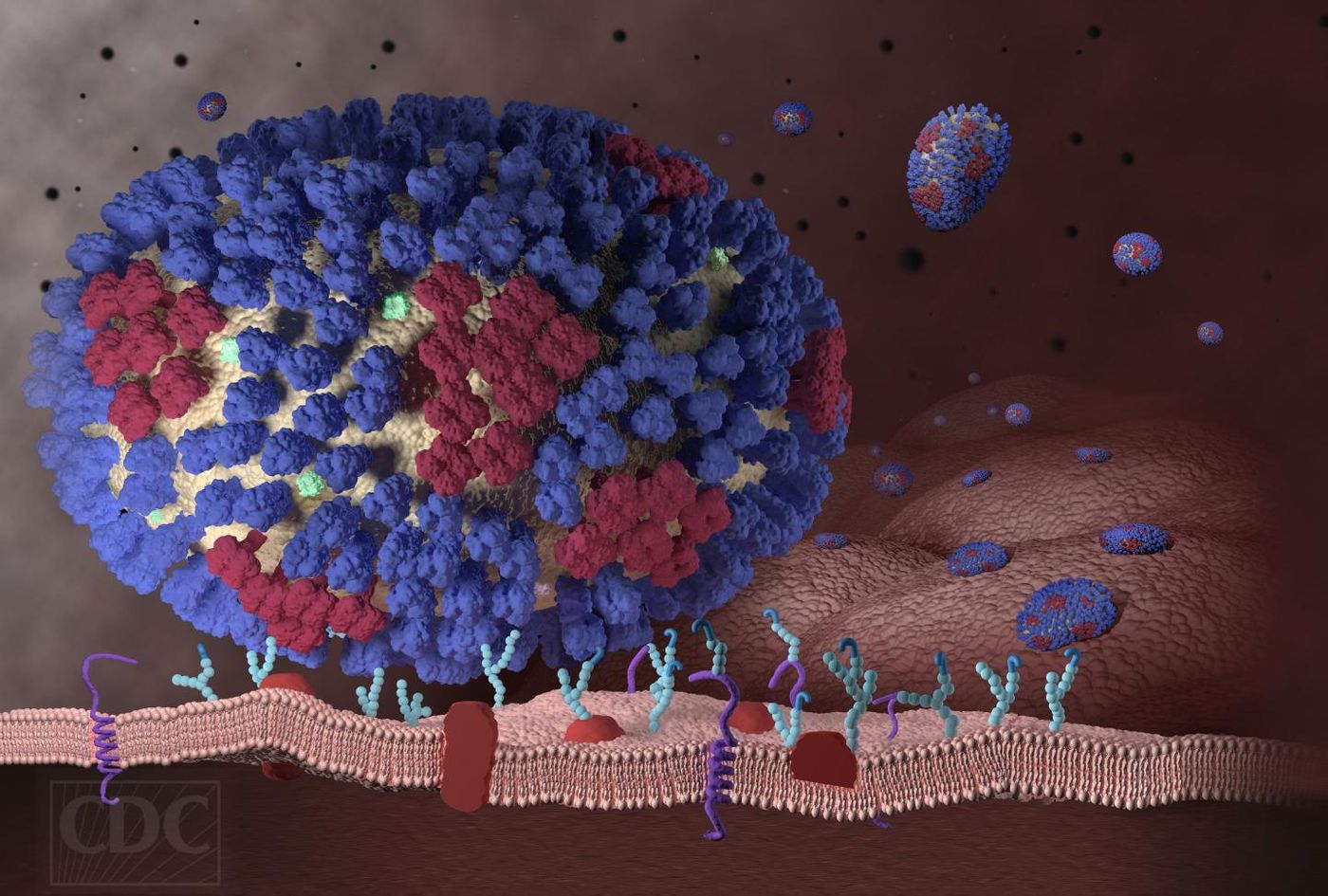
Human epithelial lung cells line the airways, making them the first cells to be infected with the flu virus. In their studies, researchers collected nearly 19,000 different genetic variations of the cell in their genetic library. They exposed each cell to the H5N1 flu strain, an influenza A virus also known as bird flu. Essentially using process of elimination, researchers began looking for genes that affected the virus’s ability to infect and replicate and those that helped the cell resist viral infection.
After several experiments, researchers found several cells that were resistant to the flu. Two genes united these cells, SLC35A1 and CIC. SLC35A1 expression produces a protein involved in the flu virus’s cell-surface receptors. Without SLC35A1, the flu virus couldn’t bind and infect the host cell.
CIC is suppresses the cellular immune response to pathogens. Without CIC, cells can promote the production of antiviral and inflammatory genes. Researchers found that CIC is also important for other strains of flu and some RNA viruses.
Study researchers pointed out that if altering the SLC35A1 or CIC genes is applied as an anti-flu strategy, this alteration can only be temporary, eventually allowing the immune system to fight the flu and then return to normal. Temporary, not permanent, action would be necessary to avoid autoimmune disorders where the immune system overreacts.
"By turning off CIC, we now allow for expression of antiviral genes that are able to respond to the flu infection," explained Balaji Manicassamy, PhD. "But it's also probably regulating inflammatory gene expression in autoimmunity and some cancers. It's a new twist that may be broadly applicable to other diseases besides the flu."
The present study was published in the journal Cell Reports.
Sources: University of Chicago Medical Center