About 15% of patients with Lyme disease develop peripheral and central nervous system involvement, often accompanied by debilitating and painful symptoms. New research shows that inflammation plays a causal role in the array of neurologic changes associated with Lyme disease, according to a study published in The American Journal of Pathology.
Researchers at the Tulane National Primate Research Center and Louisiana State University Health Sciences Center also showed that the anti-inflammatory drug dexamethasone prevents many of these reactions.
"These results suggest that inflammation has a causal role in the pathogenesis of acute Lyme neuroborreliosis," says Mario T. Philipp, PhD, professor of microbiology and immunology, and chair, Division of Bacteriology and Parasitology, Tulane National Primate Research Center, Covington, La.
Lyme disease in humans results from the bite of a tick infected with the spirochete Borrelia burgdorferi (Bb). As Bb disseminates throughout the body, it can cause arthritis, carditis, and neurologic deficits. When the nervous system is involved, it is called Lyme neuroborreliosis (LNB). Clinical symptoms of LNB of the peripheral nervous system may include facial nerve palsy, neurogenic pain radiating along the back into the legs and feet, limb pain, sensory loss, or muscle weakness. Central nervous system involvement can manifest as headache, fatigue, memory loss, learning disability, depression, meningitis, and encephalopathy.
To understand further the neuropathologic effects of Bb infection, researchers infected 12 rhesus macaques with live B. burgdorferi; two animals were left uninfected as controls. Of the 12 Bb-inoculated animals, four were treated with the anti-inflammatory steroid dexamethasone, four with the non-steroidal anti-inflammatory drug (NSAID) meloxicam, and four remained untreated. Half of each group was studied for eight weeks postinoculation and the other half for 14 weeks.
The researchers examined the role of inflammation in the nervous systems of Bb-infected animals. Significantly elevated levels of the inflammatory mediators interleukin-6 (IL-6), IL-8, CCL2, and CXCL13 were observed, as well as pleocytosis (increased cell counts, primarily white blood cells) in the cerebrospinal fluid of all infected animals - except in those treated with dexamethasone. "Chemokines such as IL-8 and CCL2 are known to mediate the influx of immune cells in the central nervous system compartment during bacterial meningitis, and CXCL13 is the major determinant of B cell recruitment into the cerebrospinal fluid during neuroinflammation," explained Dr. Philipp.
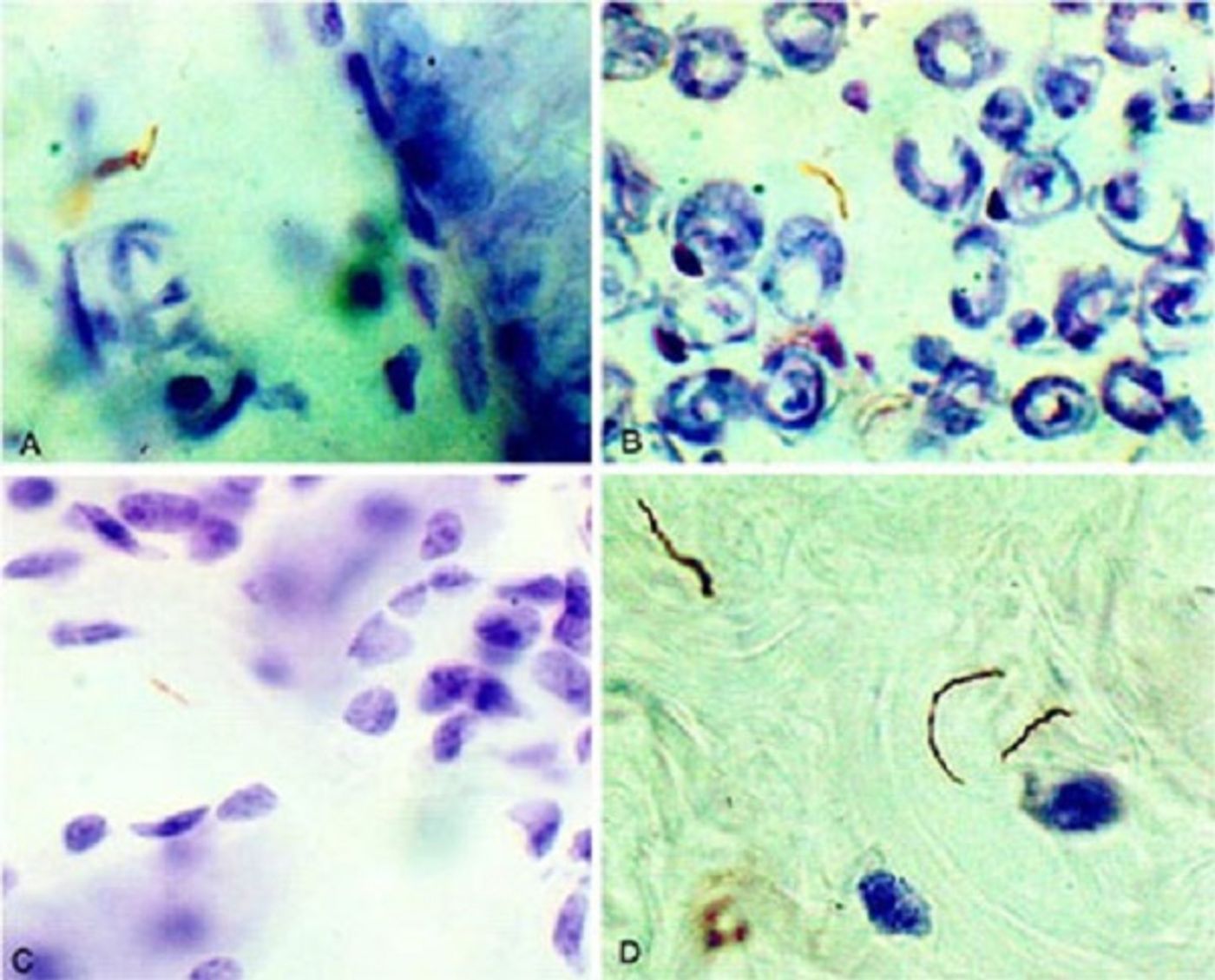
Infection with Bb led to many histopathologic findings in infected animals not treated with dexamethasone, such as leptomeningitis, vasculitis, focal inflammation in the brain and spinal cord, and necrotizing focal neurodegeneration and demyelination in the cervical spinal cord. Evaluation of the dorsal root ganglia showed inflammation with neurodegeneration, along with significant apoptosis of neuronal and satellite glial cells (which surround sensory neurons), in all infected animals with the exception of those treated with dexamethasone. Researchers were able to quantify the protective effect of dexamethasone treatment in protecting both satellite glial cell and neuronal apoptosis; in contrast, meloxicam treatment was only effective in protecting against satellite glial cell apoptosis and only after prolonged administration.
The dorsal roots of animals infected with live Bb (but not treated with dexamethasone) showed the presence of abundant lymphocytes and monocytes. Interestingly, reactions near the injection sites were histologically different from the more diffuse inflammation found along the spinal cord. The pathology found in the dorsal root ganglia and sensory nerves may explain the localized pain and motor deficits that Lyme disease patients experience close to the origin of the tick bite.
Some patients with Lyme disease also show evidence of demyelinating neuropathy and slowing nerve conduction. Nerve conduction studies in motor and sensory nerves of the macaques showed that the Bb infection resulted in specific electrophysiological abnormalities (increased F wave latencies and chronodispersion) that could be prevented with dexamethasone.
Although antibiotics are the standard and necessary first-line treatment for Lyme disease, the results show the potential therapeutic impact of anti-inflammatory or immune-modulatory agents for Lyme-related neuroborreliosis. Most of the neuropathological changes produced by Bb infection were prevented by dexamethasone, a broad-spectrum steroidal anti-inflammatory drug, whereas the nonsteroidal anti-inflammatory drug meloxicam was generally ineffective or only partially effective. Analyses of the differences in the mechanisms of action of both drugs may provide a blueprint for the development of new adjuvant treatments for LNB.
"Importantly, we found necrotizing myelitis and degeneration in the spinal cord, neurodegeneration in the dorsal root ganglia, and demyelination in the nerve roots only when lymphocytic inflammatory lesions were also observed in both the central nervous system and peripheral nervous system," Philipp says. "Our results suggest that ongoing cytokine activation in the nervous system can contribute to the persistent symptoms of fatigue, pain, and cognitive dysfunction that patients sometimes experience despite having been treated for Lyme disease."
[Source: Elsevier Health Sciences]