The Impact of Antibiotics on Gut Microbes
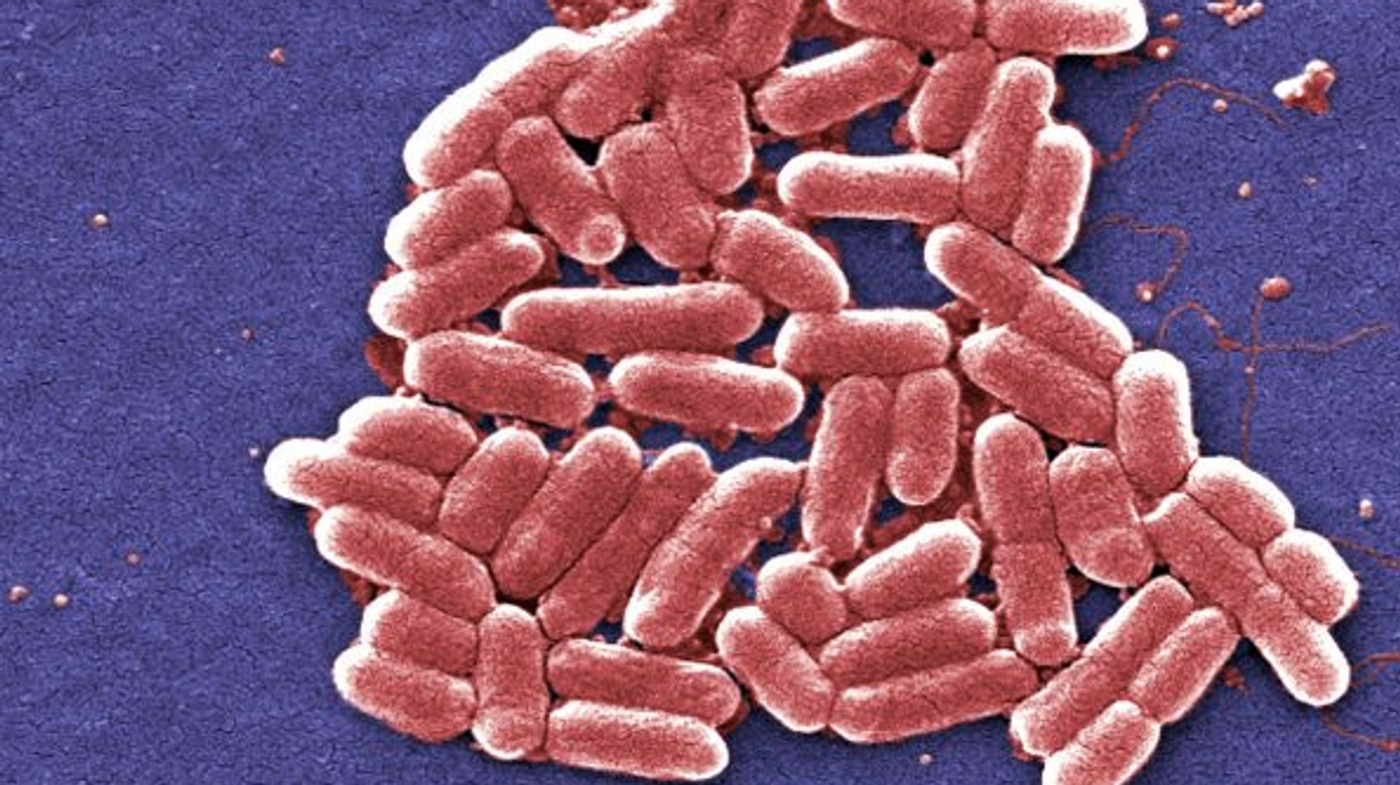
Our bodies play host to trillions of microorganisms; we carry about one bacterial cell for every human cell. That community of microbes, our microbiome, plays a critical role in our health and researchers are learning more about it (hear about that research in the video). New work has focused on how antibiotics impact the gut microbiome. The microbes that live in the gut have to be able to respire in that environment. The research, reported in eLife, has shown that antibiotics have an effect on the availability of electrons in the gut, which impacts the growth of bacteria, who compete for those electrons.
"The gut microbiome consists of a community of microbes which, when disturbed, exposes the host to risks such as infection," said first author Aspen Reese, who led the study while a graduate student at Duke University. "While it was already known that antibiotics kill or prevent the growth of bacteria in the gut, it was not clear exactly how and when those changes affect the gut environment."
The researchers used a mouse model to investigate the impact of broad-spectrum antibiotics, which can kill a wide variety of bacteria. They measured redox potential in the gut, which can indicate how easy it is for organisms to respirate.
They found that antibiotics increase redox potential. This occurred in mice that were treated with antibiotics, as well as mice that were engineered to lack an immune system.
"We also saw that as antibiotics removed bacteria and reduced their metabolic rates in the mouse gut, there was an increase in oxidizing agents called electron acceptors," explained Reese. "This new environmental state meant that the microbial community which recolonized after treatment looked very different from the original community."
Some bacteria sprang back after the antibiotic treatments stopped, including some that have the potential to be harmful; those bacteria that thrived after treatment stopped were able to use the electron acceptors in the environment to aid their growth. That rapid expansion used up the available resources and the gut returned to normal, but the original microbial community was not necessarily reestablished.
"Antibiotics may drive some microbe species extinct in a gut community, so new microbial immigrants from outside the mouse - in this case from an untreated mouse in the same cage - were likely needed to return the microbiota to its original state," noted senior author Lawrence David, Assistant Professor of Molecular Genetics and Microbiology at Duke University.
The research suggests that changes in the redox potential may relate to intestinal disorders and bacterial growth in the gut. Heightened redox potential is to be expected in inflamed guts, the researchers noted.
"In the future, our work could help inform the development of drugs that either include chemical alterations of redox potential, or that introduce competitors for excess electron acceptors, to help treat microbial disorders or prevent antibiotic-associated infections," Reese concluded.
Sources: AAAS/Eurekalert! Via eLifeSciences, eLife