Some Bacteria Gain Resistance Even Without Exposure to Antibiotics
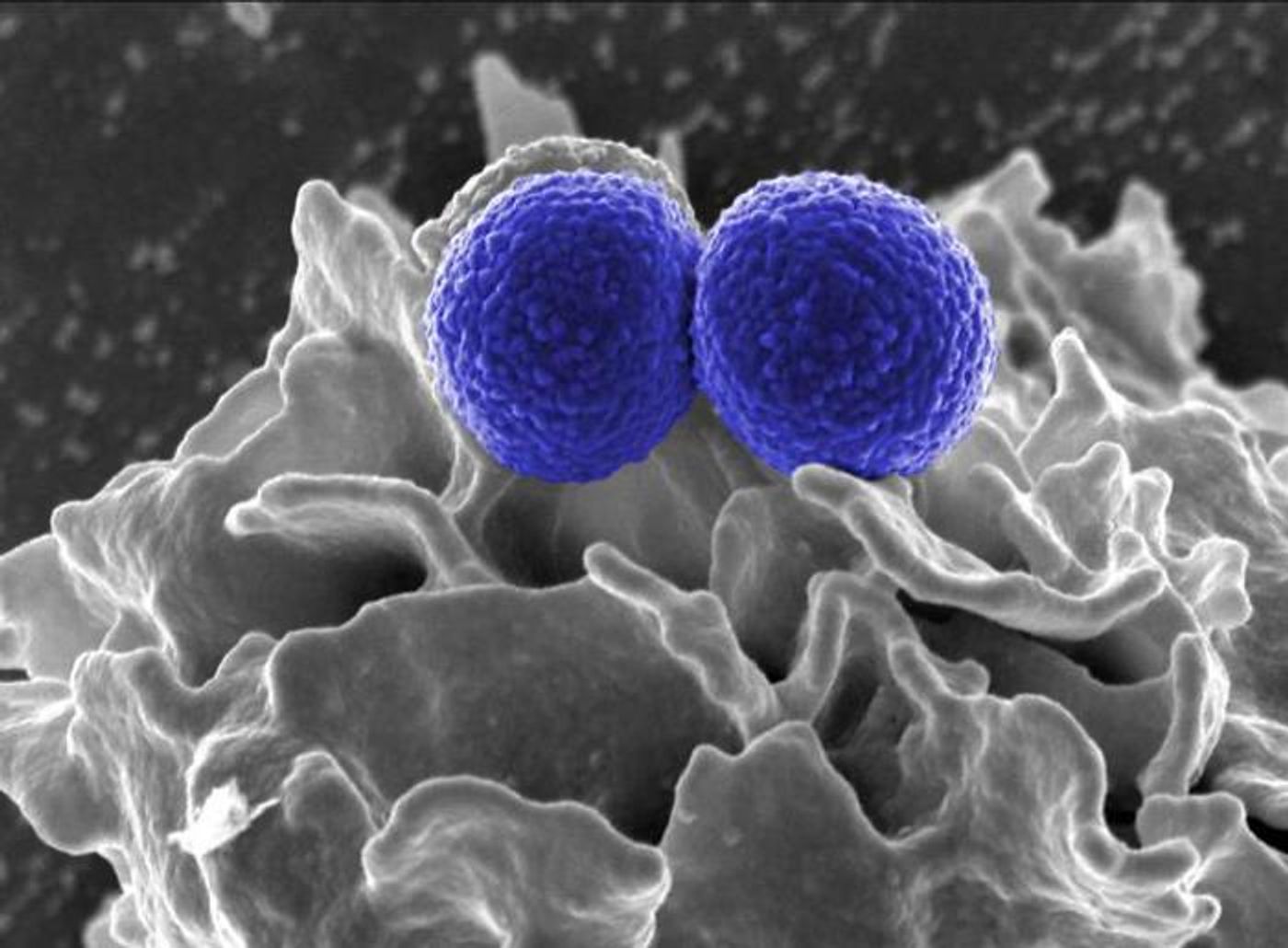
Humans share the world with vast numbers of bacteria. While most are harmless and some are even beneficial to us, there are very dangerous ones that seem to be getting worse. Many pathogenic microbes have evolved in recent decades and have become resistant to common treatments we’ve relied on to treat those infectious pathogens. It’s long been demonstrated that many bacteria have gained resistance to antibiotics after being exposed to them, but new research has found that bacteria are able to evade drugs that they have not ever encountered.
Reporting in Science, Assistant Professor Mary Dunlop (BME) and postdoctoral fellow Imane El Meouche, a study co-author, have identified a connection between antibiotic resistance and a short-term bacterial survival technique.
Bacteria use something called an efflux pump, which sits in their cell membrane, to push drugs and toxins out of their cell (as illustrated in the video below). The pumps can be crucial to surviving exposure to a drug, but they come at a high cost for the cell. It takes a lot of energy to make them, and they create a vulnerability in the cell membrane. Bacteria have to weigh the cost of their production against the need for survival.
“Pumps are well known to be very important for antibiotic resistance,” said Dunlop. “We found that cells that have more of these pumps are not only inherently more resistant to antibiotics, but they are also in a position where they mutate to achieve a higher level of drug resistance. Expression of pumps may be a stepping stone to drug resistance.”
The researchers expected that in their experiments, bacteria that were exposed to antibiotics would be the ones to develop resistance. It turned out, however, that microbes could develop genetic mutations that were likely to cause resistance even without drug exposure. The scientists decided to engineer bacteria that would create various levels of efflux pumps to determine the impact on resistance.
Next, said Dunlop, they examined how efflux pump expression, the growth rate of cells, and an enzyme that repairs DNA called MutS were connected. If bacteria have to change their DNA forever in order to become resistant to a drug, a protein that repairs the genome is probably affected, the researchers hypothesized.
They were correct; they found that efflux pump and MutS protein expression is inversely correlated in bacteria. If bacteria generate more pumps, they make fewer MutS enzymes.
Slow cell growth is known to cause more mutations in growing cells, so the researchers thought the effect might be similar. The mutations induced by slow cell growth is a likely cause of genetic resistance, just like an increase in efflux pump number is.
“Not only are bacteria resistant because they are expressing efflux pumps, but they are also more prone to mutation through these other connections,” said El Meouche. “What I find interesting is how varying expression of certain genes can lead to permanent genetic changes in the future.”
Dunlop and El Meouche still have to determine exactly how these processes result in antibiotic resistance. “We know a lot about genetic changes that pass through a population from events like the hostile environment of an infection,” said Dunlop. “But we don’t know a lot about that very first step of how an individual bacterium changes from being susceptible to resistant.”
Sources: Phys.org via BU, Microbiology and Molecular Biology Reviews, Science