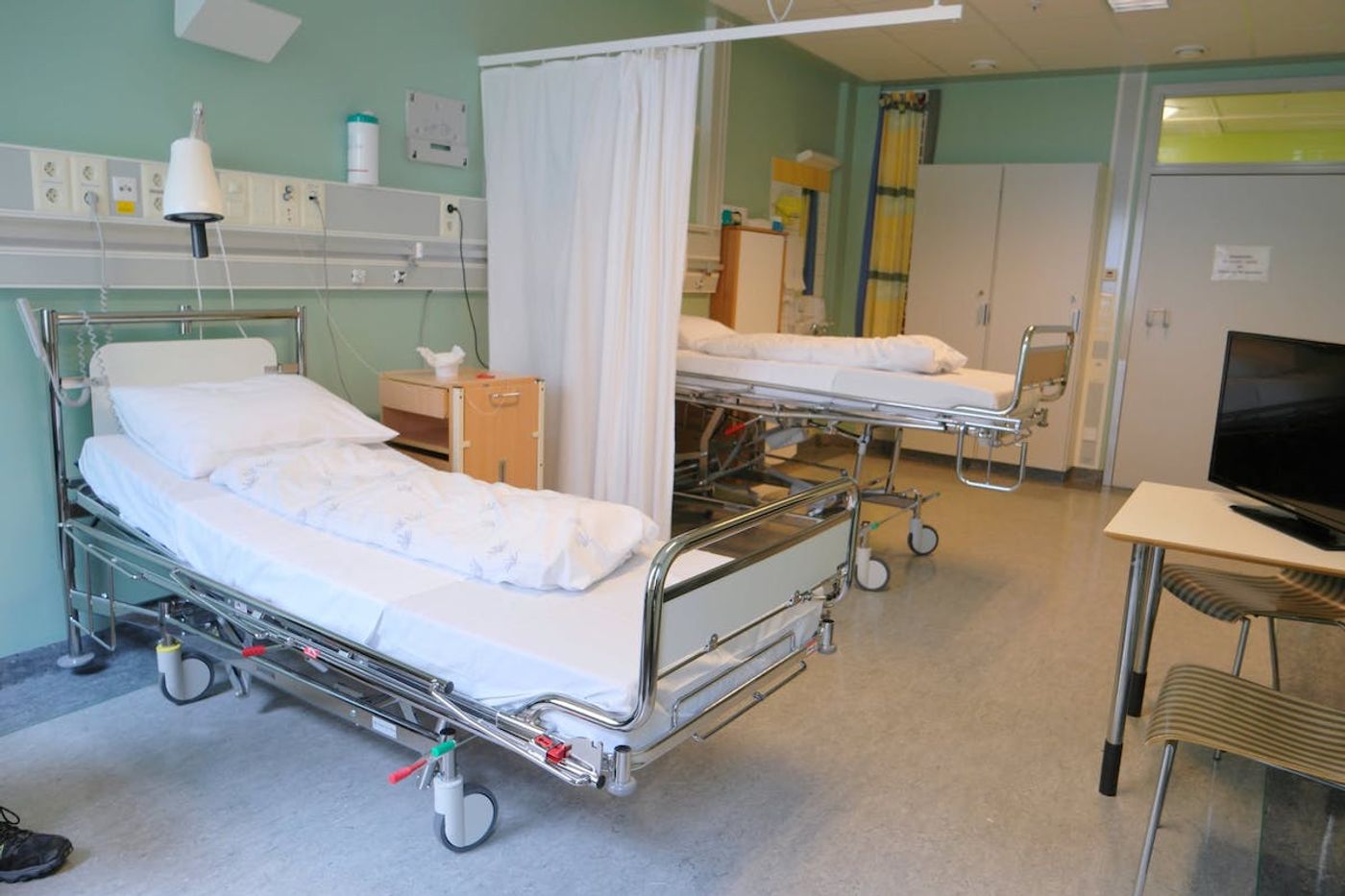
Hospital Curtains, Patients' Hands Harbor Drug-resistant Bacteria
While hospitals have encouraged staff to thoroughly and frequently wash their hands to stop germs from spreading, research has indicated that those efforts should focus on other areas as well. A recent study published in the American Journal of Infection Control (AJIC) showed that hospital privacy curtains can harbor colonies of bacteria. Another research group has reported in Clinical Infectious Diseases that around fourteen percent of hospital patients carry antibiotic-resistant bacteria in their nostrils or on their hands in the early days of a hospital stay, and can spread those germs to places they touch. That study also showed that about six percent of patients that didn’t have any drug-resistant microbes on their bodies eventually picked them up later in their stay.
While this work does not indicate that these drug-resistant microbes will sicken people, it does suggest that patients should also take an active role in preventing the spread of these multi-drug resistant organisms (MDROs).
"Hand hygiene narrative has largely focused on physicians, nurses and other frontline staff, and all the policies and performance measurements have centered on them, and rightfully so," said Lona Mody, M.D., M.Sc., an author of the Clinical Infectious Diseases study and University of Michigan geriatrician and epidemiologist. "But our findings make an argument for addressing transmission of MDROs in a way that involves patients, too."
"This study highlights the importance of handwashing and environmental cleaning, especially within a healthcare setting where patients' immune systems are compromised," said infectious disease physician Katherine Reyes, M.D., an author of the Clinical Infectious Diseases report. "This step is crucial not only for healthcare providers but also for patients and their families. Germs are on our hands; you do not need to see to believe it, and they travel. When these germs are not washed off, they pass easily from person to person and objects to person and make people sick."
Hospitals have gotten better at decontaminating rooms between patients, Mody noted. That may indicate that past patients are not to blame for the presence of these microbes. This research has not identified where the MDROs are coming from.
The AJIC study tracked the levels of bacterial contamination on freshly washed privacy curtains in Winnipeg’s Regional Burns/Plastics Unit of the Health Services Center. It showed that over fourteen days, 87.5 percent of curtains had picked up a dangerous pathogen, methicillin-resistant Staphylococcus aureus (MRSA). None of the curtains were in rooms where MRSA-infected patients were staying, either. A batch of curtains that were not put in patient rooms served as the control - none became contaminated in 21 days.
"We know that privacy curtains pose a high risk for cross-contamination because they are frequently touched but infrequently changed," said the lead author of the AJIC report, Kevin Shek. "The high rate of contamination that we saw by the fourteenth day may represent an opportune time to intervene, either by cleaning or replacing the curtains."
"Infection prevention is everybody's business," said Mody, a professor of internal medicine at the UM Medical School. "We are all in this together. No matter where you are, in a healthcare environment or not, this study is a good reminder to clean your hands often, using good techniques, especially before and after preparing food, before eating food, after using a toilet, and before and after caring for someone who is sick, to protect yourself and others."
Sources: Science Daily via Elsevier, AJIC, AAAS/Eurekalert! via Michigan Medicine, Clinical Infectious Diseases