The Therapeutic Potential of Bacteriophages
There are vast numbers of viruses in our world, and some of them, called bacteriophages, only infect bacteria. These phages were considered and tested as a therapeutic long ago, but after the introduction of antibiotics, they were left behind. Now researchers and clinicians are once again investigating their usefulness as many antibiotics become less effective in the face of antibiotic-resistant bacteria. Learn more from the video.
Phages were used to successfully treat a severe multidrug-resistant infection in 2017 in San Diego. In 2018, the University of California San Diego opened a phage therapy center. Last year, a cystic fibrosis (CF) patient was treated with phage therapy after they received a lung transplant subsequently developed a bacterial lung infection.
Graham Hatfull, a Howard Hughes Medical Institute (HHMI) Professor at the University of Pittsburgh was contacted by a colleague that knew about two cases in which CF patients were battling chronic Mycobacterium infections. For both patients, a complicated search had to be performed to find the phage that was suited to combat their infection.
"These bugs didn't respond to antibiotics," Hatfull said. "They're highly drug-resistant strains of bacteria. These really are severe, life-threatening infections." But Hatfull has amassed a huge collection of bacteriophages, and while he had not set out to use any of them therapeutically, his team responded to the call and found some candidate phages. For one patient, sadly, their discovery came too late. The other patient was treated with a cocktail of phages that had been tested for safety, twice every day for six weeks. Most signs of the infection disappeared. The infection has not indicated that it's becoming resistant to the treatment either.
"We're sort of in uncharted territory," Hatfull added. The case is straightforward, however. "We purified the phages, we gave them to the patient, and the patient got better.”
Currently, there is no framework for characterizing phages as therapeutics. They still remain in the realm of experimental therapies, and work will have to be done to make them more acceptable. We may find the need to develop novel therapeutics for antibiotic-resistant drugs pressing enough to act quickly, however.
It’s also worth noting that phages have an as-yet-undetermined impact on the bacterial community in the gastrointestinal tract, the gut microbiome, which is gaining recognition as a powerful influencer of health.
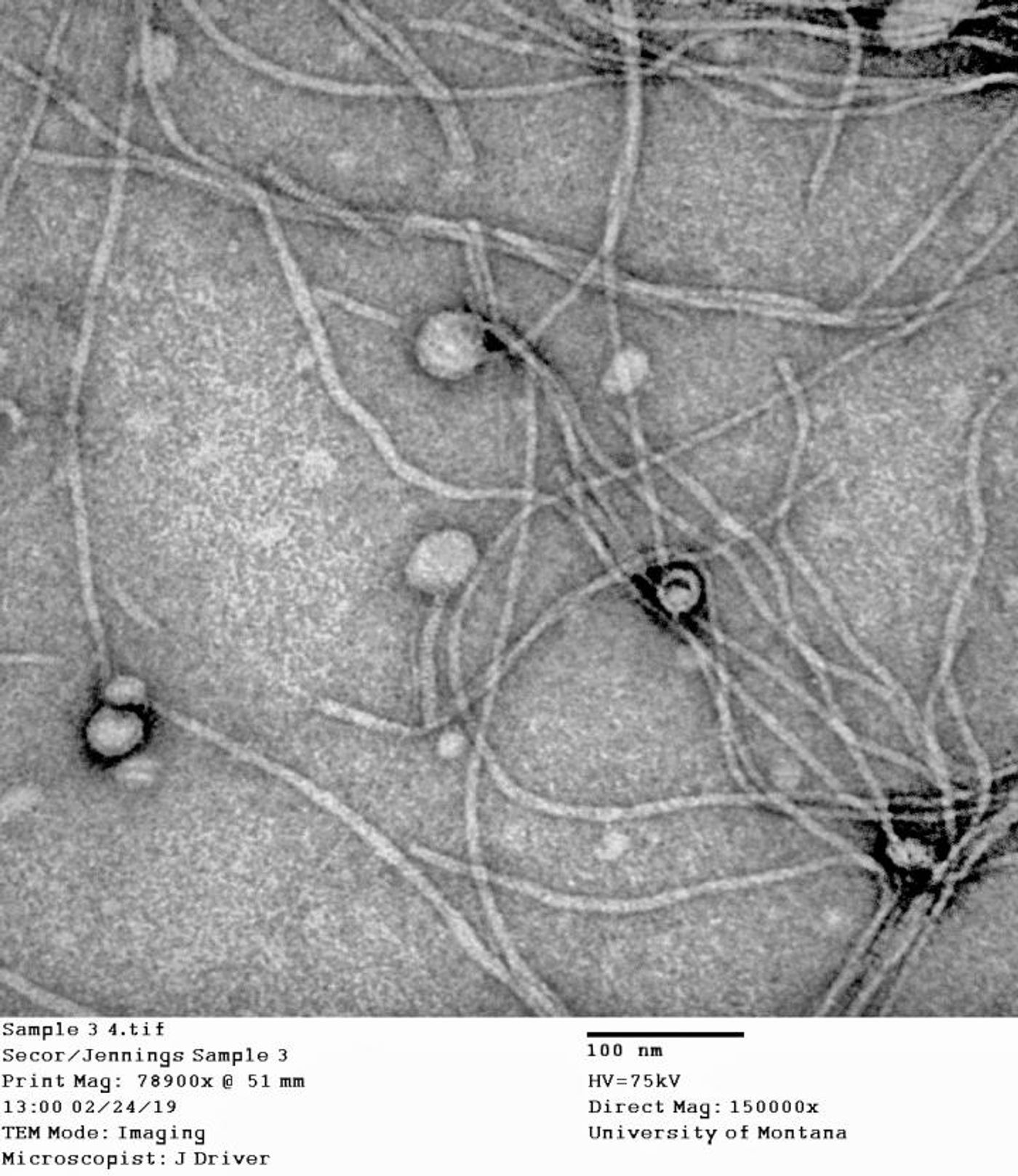
Recent work by University of Montana (UM) researchers has investigated the impact of the Pf bacteriophage on a bacterium that causes multi-drug resistant infection, Pseudomonas aeruginosa. “..we asked ourselves if it was possible that these Pf bacteriophages interacted directly with the human immune system," said Patrick Secor, an assistant professor at UM who was a co-author on the study, which was reported in Science.
The work revealed that the phage was found more often in older, chronic wounds. The phage also triggered an immune response. The study authors suggested that a vaccine against these phages could help stop the bacterial infection, and that other pathogenic bacteria may also be assisted in creating persistent infection by phages.
Sources: Science Daily via Howard Hughes Medical Institute, AAAS/Eurekalert! Via University of Montana, Science, Nature Medicine