How a Virus Can Help Treat Alcoholic Liver Disease
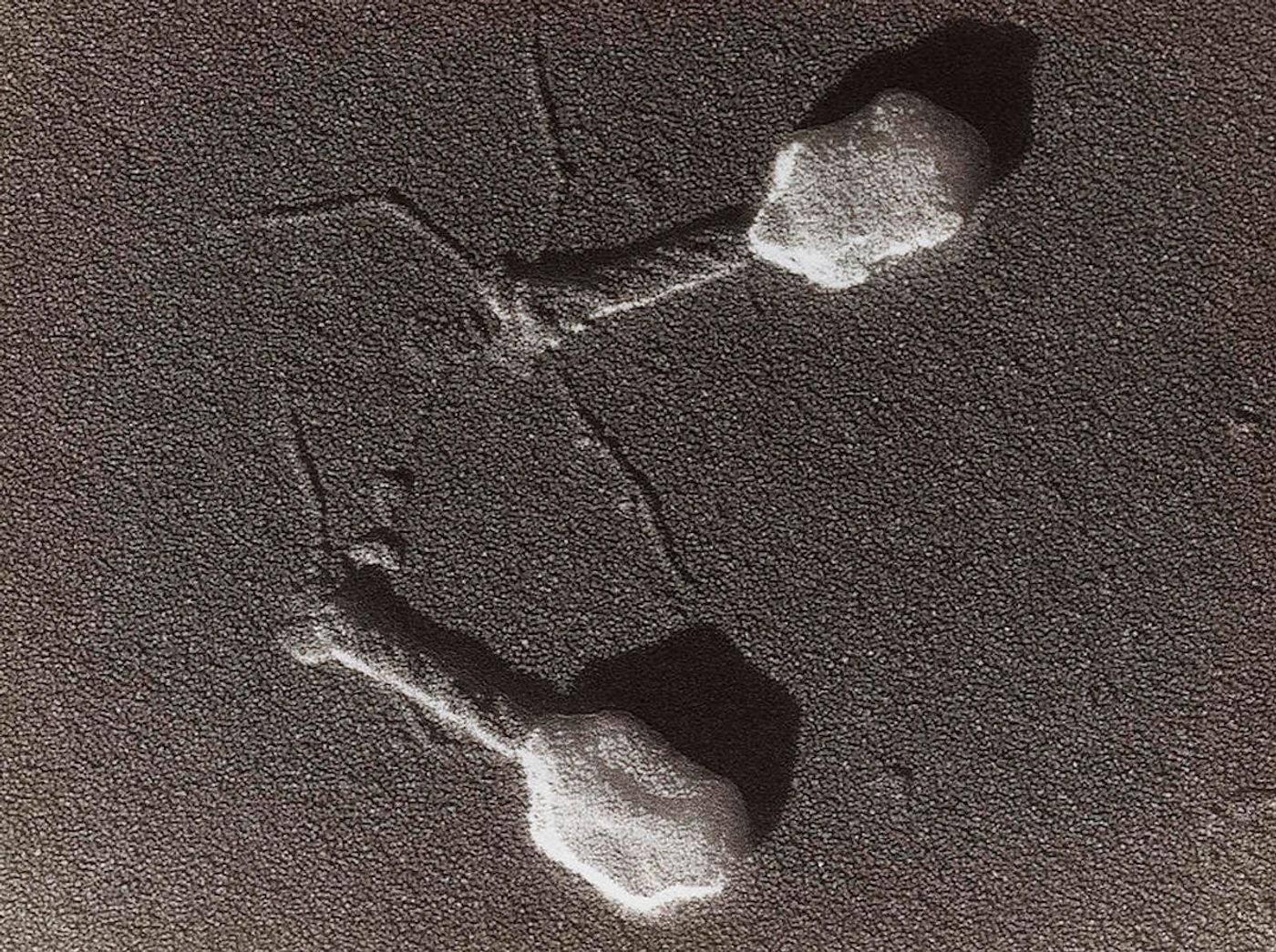
Viruses don't only infect humans, some, called bacteriophages or phages, infect bacteria. Before antibiotics were developed, phages were considered as a potential treatment for bacterial infections. Now that antibiotic-resistant infections are seen as a growing threat to public health, scientists are again beginning to consider them as a treatment. There have already been a few cases in which patients with bacterial infections that didn't respond to antibiotics were successfully treated with phages. Reporting in Nature, scientists have now found that phage therapy may be a treatment option for alcoholic liver disease.
"We not only linked a specific bacterial toxin to worse clinical outcomes in patients with alcoholic liver disease, we found a way to break that link by precisely editing gut microbiota with phages," explained the senior author of the study Bernd Schnabl, MD, a professor of medicine and gastroenterology at the University of California San Diego School of Medicine.
The most severe type of liver disease linked to alcohol is called severe alcoholic hepatitis; as many as 75 percent of patients with the disorder die within 90 days of being diagnosed. Corticosteroids are a treatment option but aren't very effective. The only cure is a liver transplant, which is only available for a limited number of patients. There are around 14,000 people on the liver transplant waiting list, and only about 8,000 are performed every year in the United States.
Liver cells can suffer direct damage from alcohol, and the alcohol also has a detrimental impact on the bacterial community in the gut. Studies in mice have shown that this change in the gut microbiome can make bacteria more likely to grow in the liver and exacerbate liver disease caused by alcohol. Researchers want to know more about the influence of gut bacteria on liver damage and whether phages can help relieve symptoms of liver disease.
In this study, the researchers found that a bacterium called Enterococcus faecalis, which is normally present at low levels in a healthy human gut, makes a toxin called cytolysin that can damage liver cells. People that have alcoholic hepatitis also have higher levels of cytolysin-generating E. faecalis.
The higher the levels of E. faecalis, the worse the liver disease is. In patients with alcoholic liver disease, over five percent of bacteria found in stool samples was Enterococcus, but there is little to none in those without the disease. E. faecalis is present in about 80 percent of patients with alcoholic hepatitis, and 30 percent of them test positive for cytolysin. About 90 percent of patients that carry cytolysin die within 180 days of being admitted to the hospital, compared to four percent of patients without cytolysin.
"Based on this finding, we believe detection of the cytolysin-gene in feces from patients with alcoholic hepatitis could be a very good biomarker for liver disease severity and risk of death," Schnabl said. "One day we might be able to select patients for tailored therapies based on their cytolysin status."
The scientists collected four phages that target E. faecalis that generates cytolysin, and treated mice carrying E. faecalis with these phages. The bacteria were eliminated from the mice, and there was no sign of alcohol-induced liver disease. Phages that did not target E. faecalis had no impact.
"This phage therapy has only so far been tested in mice, and a clinical trial will be required to test the safety of this approach, and validate our findings in patients with alcoholic hepatitis," Schnabl said.
Learn more about how phage therapy has successfully treated infection from the video.
Sources: AAAS/Eurekalert! via University of California San Diego, Nature