Amping Up Immunity to Respiratory Viruses by Targeting Memory T Cells in the Lungs
While we've learned that infection with the SARS-CoV-2 virus, which causes COVID-19, can cause problems in many organ systems, the lungs can sustain significant damage in many severe cases. Researchers are trying to learn more about how immune cells in the lungs react to the virus, which could inform the development of a vaccine for SARS-CoV-2 and other viruses. Scientists at the Salk Institute have now learned that it's easier than thought to activate immune cells that reside in the lungs and are involved in long-term immunity. The findings have been reported in the Journal of Experimental Medicine.
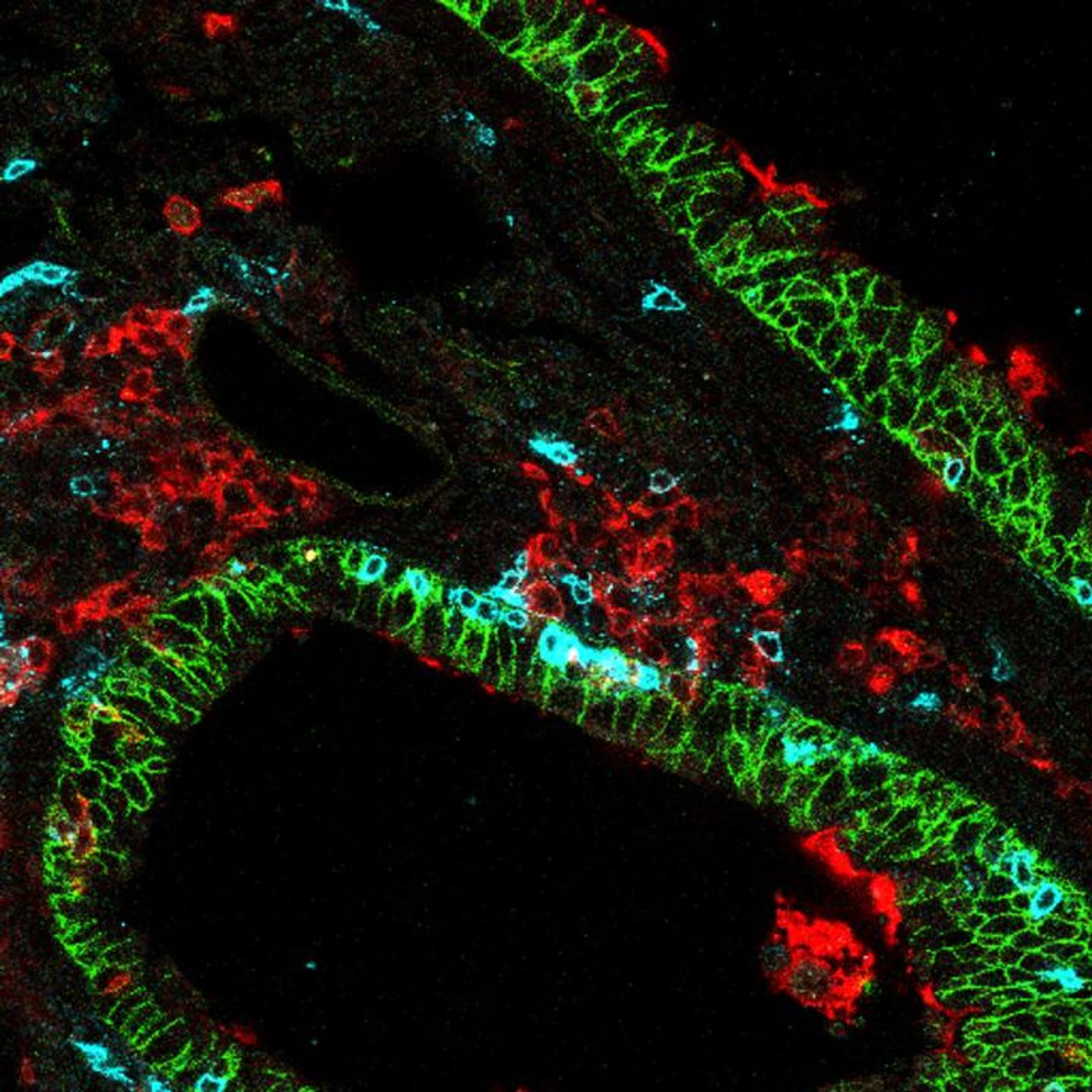
"Inside our lungs exist long-lived killer T cells that recognize specific viruses and protect us against reinfection, should we encounter the virus again. Our results have elucidated the manner by which these cells see the virus upon reinfection and provide rapid immunity," said the study leader, Salk Professor Susan Kaech, director of Salk's NOMIS Center for Immunobiology and Microbial Pathogenesis. "It also may help us understand long-term immunity as it relates to coronavirus."
If our body is exposed to a pathogenic invader like the flu virus, a type of immune cell called killer T cells can destroy these invaders, or take on a memory of them so that if there is a second encounter with the pathogen, the T cells can react more quickly. This is (a simplification of) how our body establishes long-term immunity, and vaccines take advantage of the process by giving the immune system just enough of exposure so that it will have the capacity to fight the pathogen if an infection ever happens.
While researchers know about the activation of memory T cells in organs like the lymph nodes, for example, dendritic cells are known to play an important in T cell activation in part by exposing the T cells to fragments of the pathogen. Less is known about whether or how this happens in some other organs like the lungs.
In this study, the researchers used a mouse model to remove various types of dendritic cells one at a time to see whether the memory T cells in the lungs would recognize a second infection.
"At first, our results were disappointing because it didn't seem like our experiments were working; the killer memory T cells in the lungs continued to recognize the virus after the deletion of many different messenger cell types," said first study author Jun Siong Low, now a postdoctoral fellow at the Institute for Research in Biomedicine (IRB) at the Università della Svizzera Italiana, in Switzerland. "Soon, we realized that these lung-resident killer memory T cells were special because they were not reliant on any single type of messenger cell. Instead, they could see the second influenza infection through a variety of different messenger cells, including non-immune cells like lung epithelial cells, which was a remarkably exciting finding."
Memory T cells in the lymph nodes need dendritic cells to react to a second exposure to a virus, so the physical location of memory T cells seems to dictate how they are reactivated. When they are infected, almost any kind of cell can reactivate memory T cells, suggesting that vaccines that work on the memory T cells in the lungs may be especially effective.
"We will take this knowledge into our next study, where we will examine whether lung-resident killer memory T cells form after a coronavirus infection," said Kaech. "Since not all infections induce killer memory T cells, we will determine if these cells form after a coronavirus infection and whether they can be protective against future coronavirus infections."
Sources: AAAS/Eurekalert! via Salk Institute, Journal of Experimental Medicine