SARS-CoV-2 Has Multiple Routes Into Cells
Since the pandemic virus, SARS-CoV-2 emerged on the scene late last year, it’s left a trail of devastation around the globe, and is estimated to have caused the deaths of at least 1.13 million people. Case counts are continuing to rise, and scientists are still racing to learn everything they can about this virus, how it causes infection and the COVID-19 illness in humans, and how to treat or prevent it.
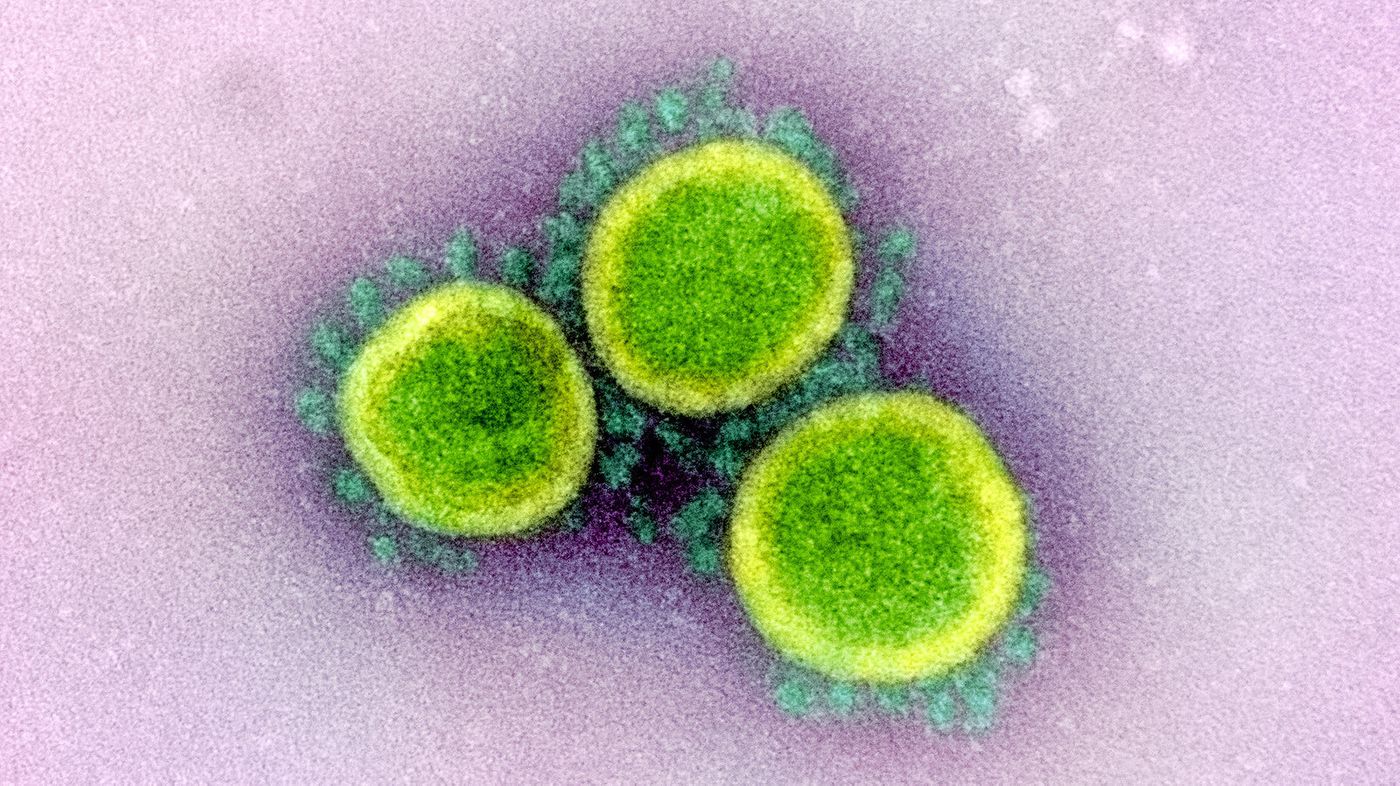
Viruses have a spike protein, which allows them to latch onto host cells and merge with the host cell membrane so a virus can get inside. We’ve known for some time that the spike protein of SARS-CoV-2 can bind to receptors called ACE2 on cells in the nasal and lung tracts. But virologists know that viruses often employ multiple strategies to infect cells.
In new work reported in Science, investigators have now identified another receptor called neuropilin-1, which can also allow the SARS-CoV-2 virus to gain entry into host cells. Not all cells express the same receptors, and neuropilin-1 receptors are also found on many cell types throughout the body.
"That SARS-CoV-2 uses the receptor ACE2 to infect our cells was known, but viruses often use multiple factors to maximize their infectious potential" explained study author Dr. Giuseppe Balistreri, head of the research group Viral Cell Biology at the University of Helsinki.
SARS-CoV-2 can infect the upper respiratory system, so it’s not limited to host cells in the lungs like some respiratory viruses. Since it can inhabit the nasal mucosa, it can spread quickly.
"This virus is able to leave our body even when we simply breathe or talk," said Balistreri.
"The starting point of our study was the question why SARS-CoV, a coronavirus that led to a much smaller outbreak in 2003, and SARS-CoV-2, spread in such a different way even if they use the same main receptor ACE2", noted study author Ravi Ojha, a researcher in the Balistreri lab.
Balistreri worked with a team led by Professor Olli Vapalahti, University of Helsinki to analyze the genomic sequence of SARS-CoV-2, which was reported in January.
Balistreri said that looking at it, "...something surprised us. Compared to its older relative, the new coronavirus had acquired an extra piece on its surface proteins, which is also found in the spikes of many devastating human viruses, including Ebola, HIV, and highly pathogenic strains of avian influenza, among others. We thought this could lead us to the answer."
That led them to consult with other researchers including giant virologist Ari Helenius at ETH Zurich, and cancer biologist Professor Tambet Teesalu of the University of Tartu, Estonia, and they found that this extra piece can bind to neuropilin-1.
Independently, another group from the University of Bristol in the UK has reached the same conclusion about neuropilin-1; their work is outlined in the video.
The researchers were also able to stop SARS-CoV-2 from entering cells by using antibodies to block neuropilin-1. Infection in a cell culture model was significantly reduced with this strategy.
"If you think of ACE2 as a door lock to enter the cell, then neuropilin-1 could be a factor that directs the virus to the door. ACE2 is expressed at very low levels in most cells. Thus, it is not easy for the virus to find doors to enter. Other factors such as neuropilin-1 might help the virus [find] its door,” said Balistreri.
"It is currently too early to speculate whether blocking directly neuropilin could be a viable therapeutic approach, as this could lead to side effects,” cautioned Balistreri. “This will have to be looked at in future studies. Currently, our laboratory is testing the effect of new molecules that we have specifically designed to interrupt the connection between the virus and neuropilin. Preliminary results are very promising and we hope to obtain validations in vivo in the near future."
Sources: AAAS/Eurekalert! via University of Helsinki, Science