SARS-CoV-2 Disrupts the Blood Brain Barrier
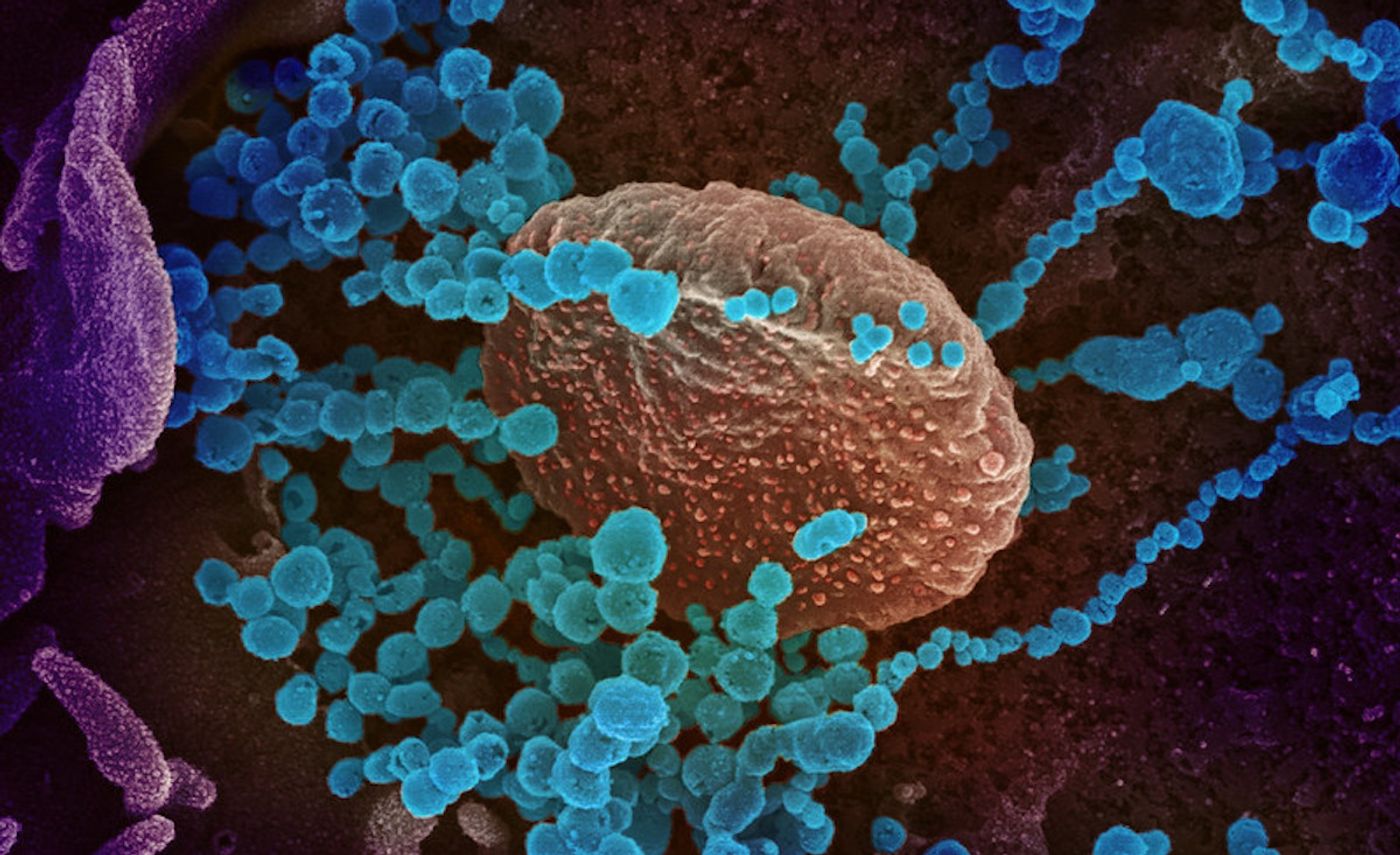
SARS-CoV-2, which causes COVID-19 has to get into cells to cause infection. It does so with a spike protein on its surface; this spike protein can attach to receptors on human host cells. For example, the spike protein can bind to ACE2 receptors on the surfaces of cells that line the nose and lungs. While the virus was first known as one that affected the respiratory system, clinicians and researchers now know that it can affect other tissues including blood vessels, and neurological symptoms like dizziness, brain fog, and headache have been observed in many patients.
Researchers are trying to learn more about how the virus may impact the brain. Scientists have now reported in the Neurobiology of Disease that the spike protein of the SARS-CoV-2 virus can disrupt the blood-brain barrier.
"Previous studies have shown that SARS-CoV-2 infects host cells by using its spike proteins to bind to the angiotensin-converting enzyme 2 (ACE2) on the host cell surface," explained principle study author Servio H. Ramirez, Ph.D., a Professor of Pathology and Laboratory Medicine at the Lewis Katz School of Medicine at Temple University. "Since ACE2 is a major binding target for SARS-CoV-2 in the lungs and vasculature of other organs in the body, tissues that are behind the vasculature, that receive blood from affected vessels, are at risk of damage from the virus."
What has been unclear is whether ACE2 is also normally found in the brain's blood vessels or if COVID-19 causes conditions that change the expression pattern of ACE2.
In this work, the researchers assessed the postmortem brain samples of (previously) healthy individuals as well as people that were hypertensive or had dementia. The scientists found that ACE2 can be found throughout the blood vessels in the frontal cortex of the human brain, but the level of ACE2 receptors is significantly increased in people that had hypertension or dementia.
Using a cell culture model, the scientists also determined that when cells were exposed to the spike protein or a portion of it called subunit 1, there were declines in the integrity of the endothelial barrier. Subunit 2 appeared to have a direct impact on the function of the blood-brain barrier.
"This is of importance because unlike subunit 1, subunit 2 of the spike protein doesn't bind to ACE2, meaning that a breach to the blood-brain barrier could occur in a manner that is independent of ACE2," noted the first study author, postdoctoral fellow Tetyana P. Buzhdygan, Ph.D.
Additional research with microfluidic devices that were meant to mimic capillaries suggested that the spike protein can increase the permeability of their walls.
"Our findings support the implication that SARS-CoV-2, or its shed spike proteins circulating in the bloodstream, could cause destabilization of the blood-brain barrier in key brain regions," Dr. Ramirez said. "Altered function of this barrier, which normally keeps harmful agents out of the brain, greatly increases the possibility of neuroinvasion by this pathogen, offering an explanation for the neurological manifestations experienced by COVID-19 patients."
We still have more to learn about the lasting neurological impacts of the virus, as well as whether it's able to directly infect neurons behind the blood-brain barrier. It does appear that a different human coronavirus, SARS-CoV, was able to invade the CNS directly.
"The viral genome has not been found yet in the specific cell types of the brain," said Dr. Ramirez. "The next steps in our work are to look for genomic viral copies in different parts of the brain using autopsy material from COVID-19 cases and to investigate the pathogen's ability to neuroinvade using different cell culture and tissue-engineered constructs."
Sources: AAAS/Eurekalert! via Temple University Health System, Neurobiology of Disease