How HIV Can Deplete White Matter in the Brain
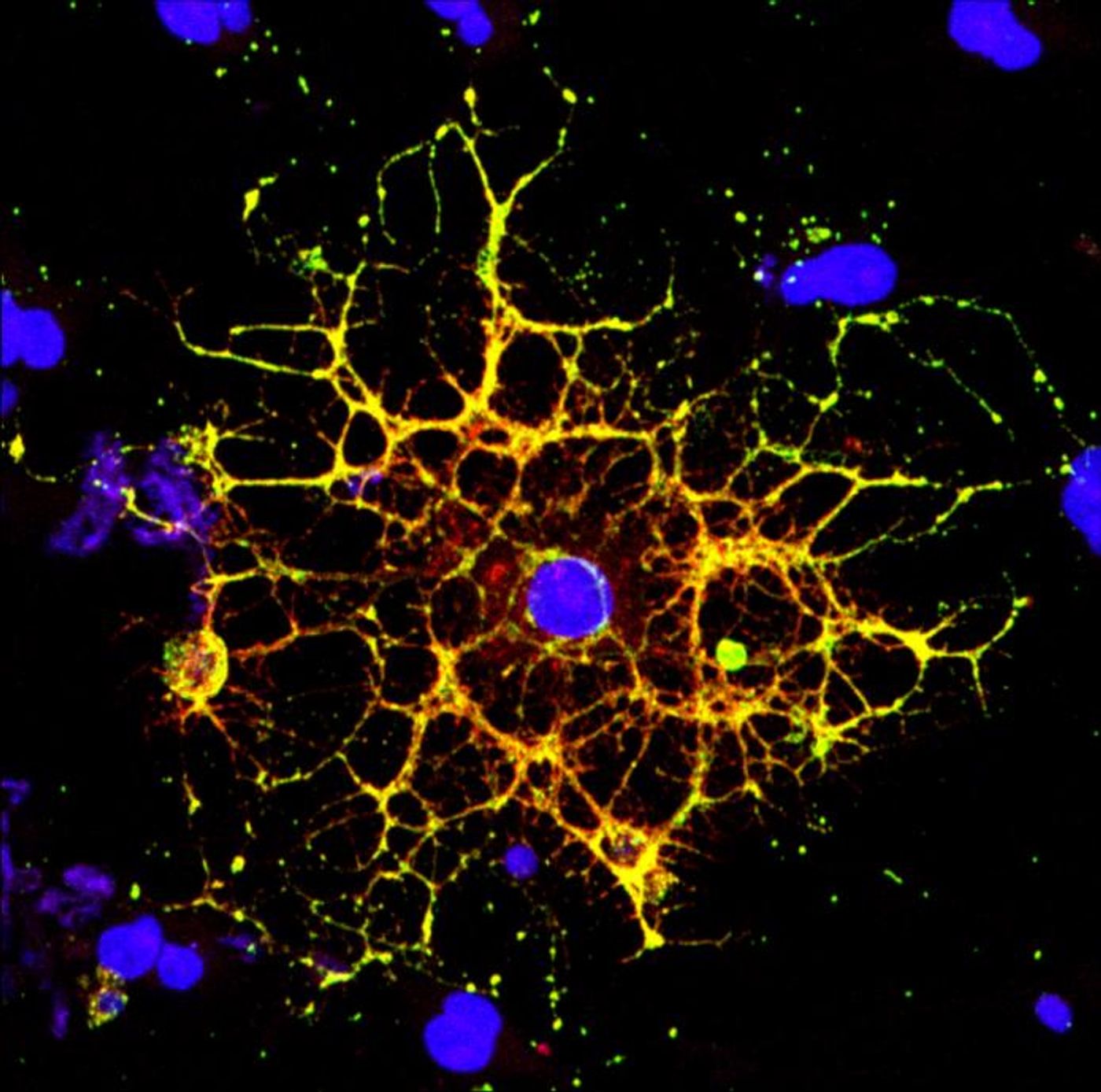
The brain is sometimes called grey matter, which is made up of neurons. But it also contains white matter, which are neurons that are encased in a fatty sheath known as myelin. The insulation myelin provides helps electrical signals move along neurons more rapidly. Clinicians and researchers have long known that in the brains of HIV patients, there is a loss of white matter. Reductions in white matter have been linked to motor and cognitive dysfunction.
"When people think about the brain, they think of neurons, but they often don't think about white matter, as important as it is," noted co-senior study author Judith Grinspan, a research scientist at Children's Hospital of Philadelphia. "But it's clear that myelination is playing key roles in various stages of life: in infancy, in adolescence, and likely during learning in adulthood too. The more we find out about this biology, the more we can do to prevent white matter loss and the harms that can cause."
Scientists have now learned more about why HIV patients lose white matter. While previous work has indicated that HIV treatments known as antiretroviral therapy (ART) can contribute to this problem, new work has shown that the virus itself plays a role too. Reporting in Glia, researchers used cell culture models to show that HIV can prevent brain cells called glia, which generate myelin, from maturing. Thus, HIV disrupts the production of white matter. The researchers were also able to restore the production of white matter by these cells when they applied a drug that blocks that process.
"Even when people with HIV have their disease well-controlled by antiretrovirals, they still have the virus present in their bodies, so this study came out of our interest in understanding how HIV infection itself affects white matter," said co-senior study author Kelly Jordan-Sciutto, a professor in the University of Pennsylvania's School of Dental Medicine. "By understanding those mechanisms, we can take the next step to protect people with HIV infection from these impacts."
It had been suggested that since HIV doesn't infect neurons, it was having an impact on the brain in an indirect way. In this study, the researchers isolated fluid from a culture of HIV-infected macrophages and exposed rat oligodendrocyte precursor cells to that fluid. This exposure didn't kill the cells, it stopped them from maturing and becoming functional. Myelin production was then reduced.
"Immune cells that are infected with the virus secrete harmful substances, which normally target invading organisms, but can also kill nearby cells, such as neurons, or stop them from differentiating," Grinspan explained. "So the next step was to figure out what was being secreted to cause this effect on the oligodendrocytes."
The scientists suspected that an excess of a neurotransmitter called glutamate was part of this mechanism. When they used a chemical to lower glutamate activity, the precursors were once again able to mature into oligodendrocytes. They also knew the integrated stress response might be playing a role. When they investigated, they confirmed that this response was active in the cultured precursor cells. The HIV-infected macrophages were found to be releasing glutamate. This was also reversible.
"If you blocked glutamate, you prevented the activation of the integrated stress response," Jordan-Sciutto said.
This work could help create treatments to address the cognitive impairments that are associated with HIV infection.
"HIV is a human disease, so it's a hard one to model," says Grinspan. "We want to find out if this model recapitulates human disease more accurately than others we've used in the past."
"When we put people on ART, especially kids or adolescents, it's important to understand the implications of doing that," added Jordan-Sciutto. "Antiretrovirals may prevent the establishment of a viral reservoir in the central nervous system, which would be wonderful, but we also know that the drugs can cause harm, particularly to white matter.
"And then of course we can't forget the 37 million HIV-infected individuals who live outside the United States and may not have access to antiretrovirals like the patients here," she said. "We want to know how we can help them too."
Sources: AAAS/Eurekalert! via University of Pennsylvania, Glia